A bug's life
In Conditions
Follow this topic
Bookmark
Record learning outcomes
This month, as millions of children head back to school, we find out how to prevent and treat the creepy crawlies that kids can pick up on the playground

As summer draws to a close and children prepare to go back to school, parents may be anxious about them bringing home more than just their homework. Infectious ailments and pesky parasites spread like wildfire in confined school environments, with head lice, threadworms and scabies topping the list of parental bugbears. And it's not just parents who may be worried. Customers returning from summer holidays in far-flung, exotic locations may have been unlucky enough to pick up some nasty parasites on their travels.
Head lice
Head lice are very common €“ NHS Choices estimates that one in three children suffer an infestation at some point each year. However, this is unlikely to provide much comfort to a distressed child or anxious parent. According to community pharmacist Sultan Dajani, pharmacies should be the first port of call when head lice strike: €Pharmacists play a key role in providing free support, confidential advice and critically fast access to effective head lice treatments before the infestation gets any worse and grips the whole household.€
Head lice are wingless insects that cannot jump, fly or hop between heads. Despite the social stigma surrounding head lice, they are not caused by poor hygiene and appear to have no preference when it comes to hair. €A child's hair can be long, short, straight, curly, light, dark, clean or dirty €“ head lice aren't fussy where they live,€ says Jerome Lemaire, marketing director, RB. Girls aged four to 11 are most at risk, probably because of how they interact, as the main method of transmission is through prolonged, head-tohead contact. Head lice can be picked up by sharing haircare products such as brushes, or clothing like hats and scarves, although this is rare as lice are unlikely to survive longer than 24 hours without a human host.
Another common misconception is that lice always cause the scalp to itch. In fact, this only occurs if the sufferer develops an allergy to the lice and this often doesn't start until several weeks after the infestation has taken hold. In rare cases, sufferers' may develop a rash on the back of their neck due to a reaction to lice droppings. Treatments should only be applied if a live louse is found on the head. Different treatment methods include physically acting products, chemical insecticides and wet combing, which can also be used for detection. Wet combing is more accurate than dry because lice become motionless when wet.
Concerns about insecticide resistance, as well as some parent's reluctance to apply chemicals to their child's scalp, means that many healthcare professionals (HCPs) no longer recommend chemical-based treatments. However, many HCPs believe that physically acting treatments are just as effective. Ian Burgess, director of the medical entomology centre at Insect Research and Development Ltd, says: €Clinical studies have shown non-pesticide [physically acting] treatments to be highly effective at eradicating head lice, so I would recommend these as a first choice treatment option.€
Such products contain dimeticone; isopropyl myristate and cyclomethicone; or coconut, anise and ylang ylang, which block lice air holes, causing suffocation and dehydration. Treatments vary in their suitability and application, so the manufacturer's instructions should be read carefully. €Treatments fail if not enough product is used, it's not applied thoroughly, not checked to see if it has worked and not repeated as required. To prevent infestation, the best thing is to check regularly €“ once a week €“ using a detection comb and treat straight away,€ advises Ian.
Head hunting
The wet combing method can be recommended to help parents detect head lice:
- Wash hair using an ordinary shampoo and apply plenty of conditioner
- Use a normal comb to straighten and detangle the hair
- Slot a detection comb in at the roots so that it lightly touches the scalp
- Draw the comb down to the ends of the hair and check for lice
- Work through the hair section-by-section until it is all combed through
- Rinse out the conditioner and repeat in the wet, washed hair
- Repeat on days five, nine and 13 to remove newly hatched lice
- Continue until no live lice are found for three consecutive sessions.
Pharmacy plays a key role in providing free support, confidential advice and critically fast access to effective head lice treatments
Threadworms
Threadworms are tiny parasites that infect a person's large intestine. They are the most common type of worm infection in the UK, with children under the age of 10 being particularly susceptible. Threadworms are white and around 1cm long, making them look like small pieces of thread around a child's bottom or in their stools. They may also be visible on pyjamas or bedding.
Threadworms lay their eggs around an infected person's bottom, usually at night, and secrete mucus that can cause itching. Threadworms are very contagious and can be easily transferred. If eggs get stuck onto fingertips while scratching, these can be transferred to the mouth or surfaces, where they can survive for up to three weeks. If eggs hatch around the anus, they can then re-enter the bowel to become adults. In addition, eggs that are airborne, for instance after shaking an infested sheet, may be swallowed and then hatch in the intestine.
Sufferers can be asymptomatic or they may develop itchiness around their bottom, or vagina in girls, which can worsen at night and affect sleep. Severe or persistent infections may cause reduced appetite, weight loss, insomnia, bedwetting or secondary bacterial infections around the anus due to scratching. If somebody in the home has threadworms, everybody should be treated, regardless of whether they're infected, as the risk of transmission is so high. Treatment is usually a single dose of mebendazole. However, this can be repeated two weeks later if required.
Although mebendazole is 90 to 100 per cent effective at killing the adult worms, it doesn't kill eggs, so strict hygiene measures should be in place for six weeks to accommodate the usual life span of a threadworm. This should involve:
- Vacuuming regularly
- Thoroughly cleaning the whole house
- Washing hands and scrubbing underneath fingernails regularly
- Showering daily, preferably in the morning
- Not biting or sucking fingernails
- Not sharing personal items
Preventing an infection can be difficult, particularly in children. However, maintaining good hygiene standards can significantly reduce the risk. If children are infected, wearing gloves at night can help prevent scratching. Although threadworms only infect humans, their eggs can get caught up in animal fur; therefore pets should be groomed regularly, too.
Scabies
Scabies is a highly contagious skin infection which occurs as tiny mites burrow into the skin. €Scabies is the great mimic,€ says Ian. €The majority of people have their first points of infestation on their hands or wrists, coupled with an itch that is more or less generalised, bilateral and worse at night, but it doesn't affect the back, with an itchy rash on the inside of the thighs or around the midriff. People who come out with odd spots on their forearms, lower legs and various other parts probably don't have scabies.€
Scabies is primarily spread through prolonged, skin-to-skin contact. In rare cases, it may be spread by sharing clothing or personal items. However, mites can only survive for 24-36 hours without a host. In the UK, most outbreaks occur during winter, possibly due to people spending more time indoors in close proximity. However, prevalence is still low, with the Royal College of General Practitioners recording the overall incidence as just two to eight cases per 1,000 patients each year. €Scabies is actually quite rare,€ adds Ian. €The probability of someone presenting to the pharmacist with scabies is low, although it must never be forgotten.€
It can take up to eight weeks for symptoms to appear after the initial infection. However, if an individual has been infected before, symptoms may appear in just one or two days. Permethrin cream is usually the first treatment choice, although malathion lotion is also effective. Mites are resistant to soap and hot water, and cannot be scrubbed off. Prolonged contact with other people should be avoided until treatment is complete and all members of the household have been treated, regardless of whether they present symptoms. Certain topical creams (e.g. containing crotamiton) can help to relieve itching, and oral antihistamines can help to soothe itching and aid sleep.
Crusted scabies can occur in severe cases or in susceptible individuals, such as children or those who have a suppressed immune system. This often starts as normal scabies and develops into thousands or even millions of mites causing a non-itchy rash and thick, warty crusts on the skin, which may be mistaken for psoriasis. These customers should be referred to the pharmacist.
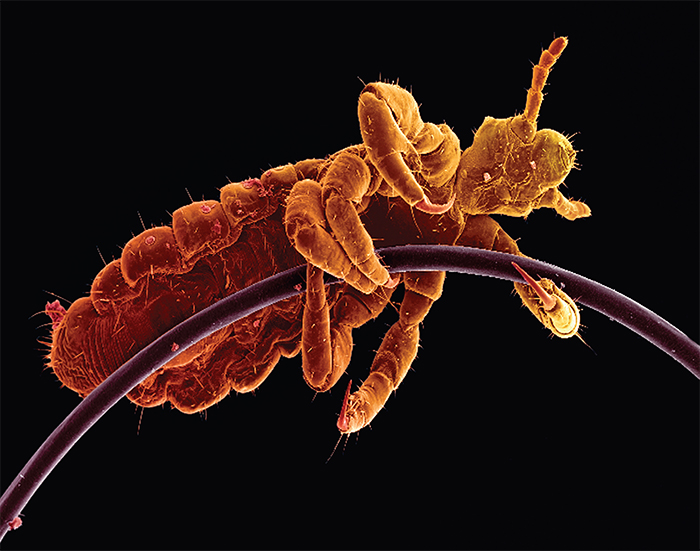 One in three children will suffer a head lice infestation at some point each year
One in three children will suffer a head lice infestation at some point each year
Tropical paradise?
According to the World Health Organization (WHO), there were 207 million cases of malaria worldwide in 2013, of which around 2,000 were in UK residents. Malaria is a serious tropical disease that is spread by mosquitoes infected with the Plasmodium parasite. Unless diagnosed and treated promptly, it can be fatal. Symptoms include a cycle of fever, sweats and chills; headaches; vomiting; muscle pain and diarrhoea. These usually begin seven to 18 days after infection, but can take up to a year. The WHO recommends the A, B, C, D guide to travellers:
- Awareness of malaria status
- Bite prevention via insect repellent, clothing and mosquito nets
- Check whether preventative medication is required
- Diagnosis via immediate medical advice if symptoms develop
Schistosomiasis, or bilharzia, is a condition picked up in fresh water in tropical and subtropical regions and, following malaria, is the second most common disease caused by parasites. Between 2011 and 2012, there were 77 reported cases in England, all of which were picked up while abroad. The acute condition develops a few weeks after infection and may be mistaken for malaria, as it produces similar 'flu-like symptoms. If untreated, the acute condition can turn chronic months or even years after infection. Chronic symptoms include developing cystitis, abdominal pain and blood in the urine, faeces or vomit. Customers should avoid infection by not swimming or wading in fresh water while abroad.
