In Conditions
Follow this topic
Bookmark
Record learning outcomes
Pregnancy can be both an exciting and worrying time, having a significant impact on a woman’s physical and mental health. Every pregnancy is different, but most pregnant women experience minor niggling health issues, such as heartburn or sickness, and some develop more serious pregnancy-related complications, such as pre-eclampsia.
Many minor health problems during pregnancy can be managed with self help measures and suitable over-the-counter medicines. Before taking any medicines during pregnancy, women should check with a pharmacist, midwife or GP, as many medicines can cross the placenta and reach the developing baby.
Constipation and piles
Women may get constipated early on in pregnancy due to fluctuating hormones. Managing (and preventing) constipation involves regular exercise, eating high-fibre foods and drinking plenty of water (or water-based drinks). Certain iron supplements for anaemia can cause constipation.
Hormonal changes can also lead to piles (haemorrhoids) – these enlarged blood vessels around the rectum and anus can become sore and itchy. The pharmacy team may be able to suggest a suitable ointment, cream or gel to ease the symptoms.
“Constipation can also cause piles,” says Dr Hana Patel, NHS GP and GP medico-legal expert witness. “If this is the case, women should try to keep their stools soft and regular by eating plenty of food that’s high in fibre, including wholemeal bread, and drinking fluid throughout the day.”
Sickness
Nausea and vomiting in early pregnancy is often called ‘morning sickness’, but it can happen at any time of day or night. Pregnancy sickness affects up to nine in every 10 pregnant women and is a common cause of hospital admissions. The symptoms tend to clear up by weeks 16-20 of pregnancy. Most cases can be treated with oral rehydration, dietary advice, rest, and prescribed anti-sickness medicines (anti-emetics). Avoiding foods or smells that trigger the sickness, and eating small, frequent meals of plain carbohydrate-rich foods, such as crackers, may help. Some women find acupressure is helpful too.
New international research at the University of Cambridge (published in Nature Mental Health) has confirmed that pregnancy sickness is caused by a hormone produced by the growing baby – called growth differentiation factor 15 (GDF15). GDF15 is also produced in low levels in the mother’s body outside of pregnancy. The severity of pregnancy sickness depends on how much of the hormone is produced by the baby, and how much exposure the mother had to this hormone before her pregnancy.
“The more sensitive she is to this hormone, the sicker she will become,” says Professor Sir Stephen O’Rahilly, who led the study. “Knowing this gives us a clue as to how we might prevent this from happening.”
Hyperemesis gravidarum is a more severe form of nausea and vomiting, affecting up to three in every 100 pregnant women and putting the life of the mother and baby at risk. This needs to be treated in hospital with IV fluids to prevent dangerous levels of dehydration and malnourishment.
“I would recommend that women call 111 or get advice if they’re vomiting and have very dark-coloured urine or haven’t passed urine in more than eight hours, are unable to keep food or fluids down for 24 hours or feel severely weak, dizzy or faint when standing up,” says Dr Patel.
“Pregnancy sickness affects up to nine in every 10 pregnant women”
Indigestion and heartburn
Indigestion and heartburn (acid reflux) affects up to 80 per cent of pregnant women, especially as the pregnancy progresses. It may be caused by hormonal changes and the growing baby pressing against the mother’s stomach. The symptoms may be eased with diet and lifestyle changes, such as eating small meals regularly, sitting up straight during and after eating, sleeping more upright, and cutting down on caffeine and rich, spicy or fatty foods. Other possible food triggers include chocolate, mints, citrus juices and tomatoes.
“Try and eat healthily,” says Dr Patel. “You’re more likely to get indigestion if you’re very full, so also consider changing your eating and drinking habits. Look at your sleeping position as this can make indigestion symptoms worse, while stopping smoking and avoiding alcohol can reduce symptoms.”
If lifestyle changes don’t help, women should speak to the pharmacy team, GP or midwife. Antacids and alginates can often ease indigestion and heartburn, but it’s important to make sure these are suitable for pregnant women. A GP may prescribe a proton pump inhibitor (PPI) if the symptoms are severe and antacids haven’t worked.
Incontinence
In October 2023, the Government announced a new nationwide pelvic health service to ensure that all women are offered a self-assessment of their pelvic health as early as possible in pregnancy – and by 18 weeks at the latest.
Stress incontinence is a common problem during and after pregnancy, where urine leakage occurs after coughing, laughing, sneezing or movement. This is often a temporary problem due to relaxed pelvic floor muscles (which support the bladder, bowel and uterus). However, around one in three women also experience urinary incontinence three months after pregnancy, due to birth injuries.
“Women can strengthen their muscles by doing pelvic floor exercises,” says Dr Patel. “This helps to reduce or avoid stress incontinence after pregnancy. All pregnant women should do pelvic floor exercises, even if they are young and not suffering from stress incontinence now.”
Vaginal discharge and thrush
Many women notice that their vaginal discharge changes during pregnancy – either in quantity or in texture. A healthy vaginal discharge is usually thin, clear or milky white, and doesn’t smell unpleasant. Some pregnant women become more prone to thrush (white cottage-cheese-like discharge, itching and irritation), especially during the third trimester.
There’s no evidence that thrush can harm an unborn baby but it can be very uncomfortable. Pregnant women should speak to their GP or midwife before using any thrush treatments. They may be prescribed clotrimazole cream or pessary. Oral anti-thrush tablets aren’t suitable for women who are pregnant or breastfeeding.
“Maternity support pillows can help with posture when sitting”
Swollen ankles
It’s normal to get some swelling in pregnancy, especially in the legs, ankles, feet and fingers, caused by a build-up of fluids. This tends to be worse at the end of the day and further into the pregnancy.
“Wear comfortable shoes and socks,” says Dr Patel. “Women should avoid tight straps or anything that might pinch if their feet swell. Try to rest with their feet up as much as they can. Drinking plenty of water helps the body get rid of excess water.”
Women should always get any new swelling checked out by their midwife or GP, especially if it occurs suddenly. This can be a sign of pre-eclampsia, which affects around one in 25 pregnancies. Other signs of pre-eclampsia include high blood pressure and protein in the urine – these are usually picked up during routine antenatal checks.
Stretch marks
There’s no specific treatment for stretch marks, and there’s usually no way to prevent them. These narrow, streak-like lines on the tummy, and sometimes upper thighs and breasts, affect around eight in every 10 pregnant women. The lines can be pink, red, purple or brown, depending on the mother’s skin colour. Sometimes they can be itchy. There are many skin creams and oils claiming to remove stretch marks, but there’s little evidence to show these work.
“After the baby is born, the marks may gradually fade into paler scars and become less noticeable,” says Dr Patel. “They probably won’t go away completely. Gaining pregnancy weight steadily may help minimise the effect of stretch marks. During pregnancy, it’s normal to put on weight over a relatively short period.”

Stretch marks occur in eight out of 10 pregnant women.
Back pain
Many women experience back pain in pregnancy. This is often due to ligament changes as the body gets ready for labour, which then puts more pressure on the joints of the lower back and pelvis. Good posture is important – bending the knees and keeping the back straight when lifting – and wearing flat shoes. Maternity support pillows can help with posture when sitting, especially later on in the pregnancy. Women should discuss pain relief with their GP and midwife, but they can usually take paracetamol to ease pain during pregnancy.
If the back pain is affecting their day-to-day life, women may be referred to a specialist physiotherapist. It should always be checked by a healthcare professional if it’s accompanied by fever, vaginal bleeding, pain on urination or pain under the ribs. Back pain later in pregnancy can be a sign of early labour.
Newborn health
Caring for a newborn can be a steep learning curve – from feeding choices and changing nappies to washing and sleep routines. Many parents worry about whether their baby is well and thriving, as lots of health issues can arise in the early days. If parents are concerned about anything, or their baby isn’t feeding well or is sleepy or irritable, parents should tell their midwife or GP straightaway.
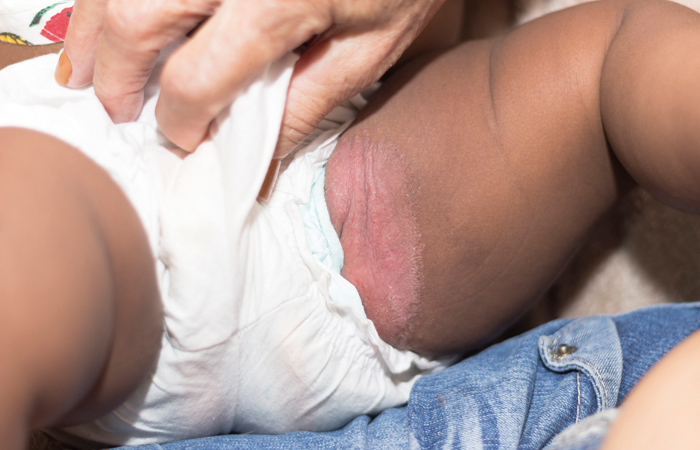
Nappy rash: Nappies should be changed regularly, and the baby’s skin should be kept clean and dry, using water or fragrance-free, alcohol-free baby wipes. A thin layer of barrier cream can protect the skin, while a nappy rash cream can treat the symptoms. A GP may prescribe a steroid cream or ointment, an antifungal cream and/or antibiotics if there’s significant redness and soreness.
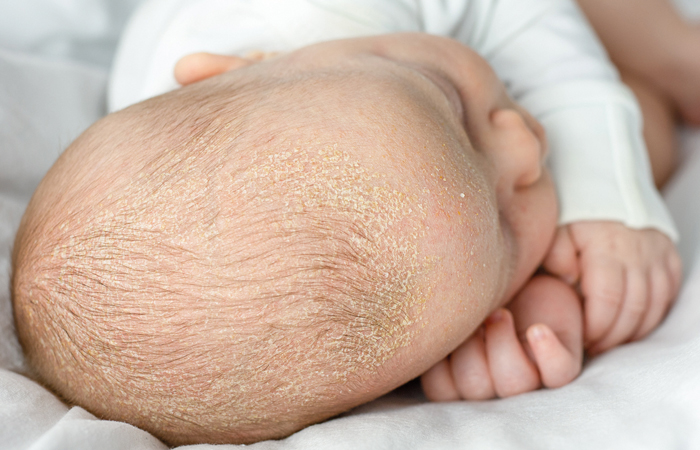
Cradle cap: These patches of greasy, scaly skin on the scalp are harmless and don’t bother the baby. Parents can loosen the scales by gently massaging an emollient onto the baby’s scalp and then gently brushing them away with a soft brush, followed by washing with baby shampoo. They should speak to a GP if the skin is bleeding or leaking fluid, as this may be a sign of atopic eczema.
Dry skin: Most newborns may have peeling or flaky skin in the first few days. Spots and rashes are also common. Parents should use only plain water on their baby’s skin for at least the first month – no perfumed or medicated skincare products. If the baby’s dry skin becomes cracked, a midwife or GP may advise using a plain emollient.
Diarrhoea and vomiting: Most babies have loose stools or bring up some milk (called posseting) from time to time. If parents are worried that their baby has diarrhoea or is vomiting, they should speak to their midwife, health visitor or GP. It’s important to make sure the baby doesn’t become dehydrated.
Trapped wind: Some babies are prone to trapped wind, especially after a feed. Babies with colic can be difficult to settle, have frequent crying episodes and appear to be in distress. Parents should speak to their midwife to rule out other causes and, if the baby is bottle-fed, discuss switching to a special type of infant formula milk.