In Conditions
Follow this topic
Bookmark
Record learning outcomes
Scarring affects over 20 million people in the UK and while nearly half of people are aware of emotional problems relating to scarring, less than a quarter know about the physical impact that it can have, according to research from The Scar Free Foundation.
Most scars fade over time, but they don’t always completely disappear, and some may become raised and/or have a different texture to the surrounding skin. Severe scarring can cause pain, itching and a loss of movement – it can even affect people’s ability to breathe and cause emotional challenges, according to Leanne Skuse, head of skin camouflage at the Changing Faces charity.
“Acquiring a visible difference, such as scarring, not only has a physical impact on a person, but can have an emotional one too,” she says. “Loss of identity is something that a lot of our community speak about. Who they see in the mirror no longer matches the mental image they have of themselves, and this can be challenging to cope with.”
Layer up
The skin is the body’s largest organ and, despite being just a few millimetres thick, makes up around one-seventh of a person’s body weight. Its main function is to prevent water loss and protect the inside of the body from the outside environment, including bacteria, viruses, parasites, heat and the sun’s UV rays. It also has other essential roles, such as controlling the internal body temperature and helping people to sense the world around them. An average square inch of skin contains 650 sweat glands, 20 blood vessels and more than 1,000 nerve endings.
Skin has three layers:
- The epidermis is the waterproof outer layer that gives skin its colour. It’s constantly getting rid of old, dead cells and making new ones, which means the epidermis can repair itself when it gets damaged – this process can lead to scar formation
- The dermis is a layer of tissue beneath the epidermis. It gives skin its strength and elasticity and protects the body from physical stress. It also makes sweat and oil, and contains blood vessels, hair follicles and nerve endings that detect heat, pressure and pain
- The hypodermis is a deeper layer of fat and tissue that helps to insulate the body. It attaches skin to the bones and muscles, providing essential padding and protection, and contains the nerves and blood supply. It also contains elastin, the protein that helps tissues return to their normal shape after stretching.
Healing and scarring
Scarring is part of the body’s natural healing process after skin tissues are damaged, usually by an injury, infection or surgery. When the skin gets damaged, its tissues break down and release large amounts of a protein called collagen. Collagen fibres build up at the injury site, as a form of scaffolding for new skin cells, and help to heal and strengthen the wound. The blood supply to the damaged area of skin also increases. This healing process continues for several months, causing the scar to become raised and lumpy. Over time, the collagen build-up breaks down and the blood supply reduces again, causing the scar to gradually become smoother and softer.
Most scars will fade over time. However, scar tissue often has a different texture to the skin it replaces. The epidermis can usually repair itself easily, but if the dermis is affected, rebuilding is more complex, leading to a more noticeable scar.
“The process of scar healing begins as soon as the wound is starting to heal and can carry on at a cellular level for one to two years,” says Lesley Gilchrist, registered midwife and co-founder of My Expert Midwife. “Age and skin type can influence how a scar heals and how long it can take to heal – the longer it takes to heal, the thicker it can form.”
Antiaging skincare tips
As skin ages, it becomes more prone to dryness, itching, blotchiness, sun damage, fine lines and wrinkles. Lower levels of oestrogen during the menopause also reduces oil and collagen production and slows down skin’s cell renewal process. Following a healthy skin care regime, from the early-40s, may help to reduce signs of ageing as people get older. Here are a few tips to pass on to pharmacy customers:
- Protect the skin from sun damage with sunscreen products of SPF50, covering up whenever possible and staying in the shade
- Apply moisturiser daily to the face, body and lips and a retinoid-containing serum to the face in the evenings for extra hydration
- Use anti-ageing skincare products – these often contain anti-oxidants, hyaluronic acid, vitamin A-derivatives (retinols), collagen-boosting peptides and vitamin C
- Use an eye cream to reduce the appearance of fine lines, and a firming neck cream
- Clean the skin with a gentle exfoliating cleanser to remove dirt, make-up, bacteria and dead skin cells
- Stop smoking – smoking can prematurely age the skin
- Eat plenty of fruit and vegetables, protein and healthy fats to keep the skin nourished from within
- Get enough sleep, as this helps the body to rest and renew itself.
Different types of scars
Normal fine-line scars are caused by a minor wound, such as a cut, or surgery. This raised line will fade and flatten over time, usually in under two years. These scars may initially be itchy as they heal
Keloid scars occur when too much collagen is produced at the site of a wound. The scars are raised and can be pink, red or a similar colour to the surrounding skin. They keep growing, even when the wound has healed. They’re often itchy or painful and can restrict movement if they’re tight and near a joint. If someone has had one keloid scar, they’re at risk of more keloid scars in the future
Hypertrophic scars are also caused by excess collagen at the site of a wound, but these don’t keep growing larger. They may continue to thicken for around six months, before gradually improving over a few years. They tend to be more common in young people and people with black or brown skin
Burn scars can cause scar contractures, when the skin tightens and restricts movement
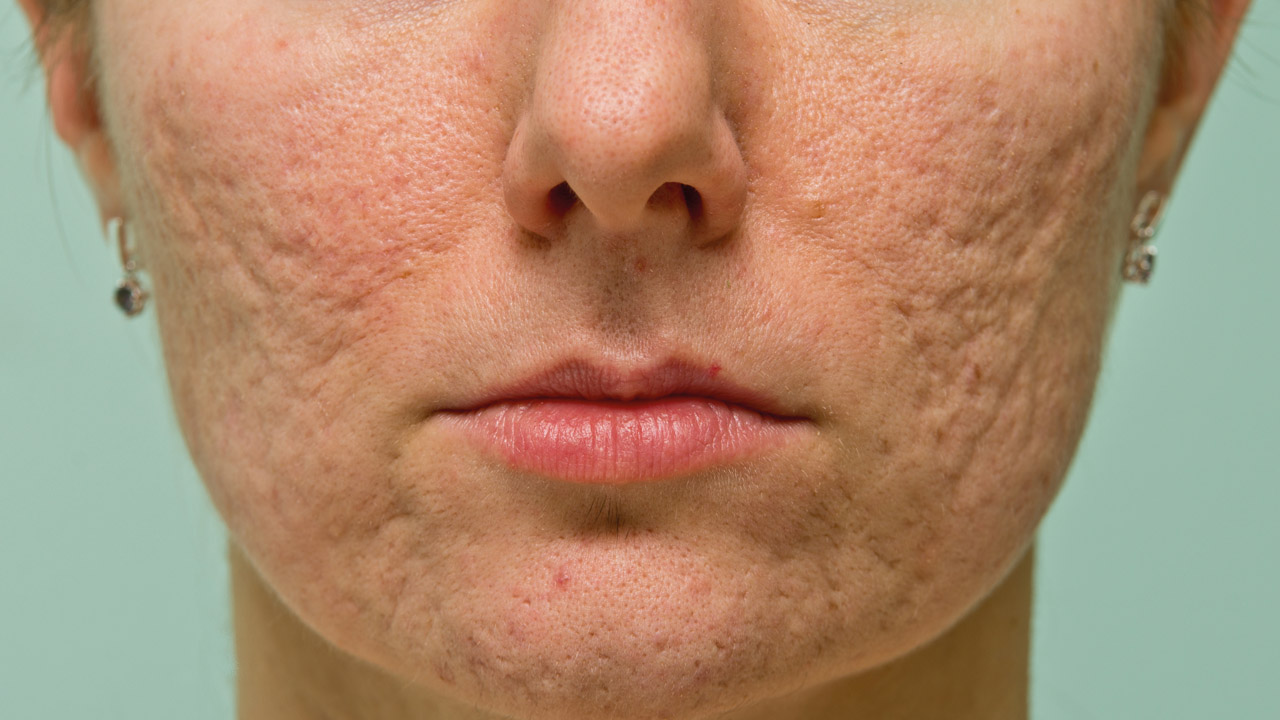
Pitted or sunken scars are dents in the skin caused by skin conditions such as acne and chickenpox. These may also be caused by deeper injuries and may be known as ‘ice pick’ scars
Stretch marks occur when the dermis overstretches and tears, causing narrow streaks or lines to appear on the skin’s surface. This may happen during pregnancy or during a growth spurt. Stretchmarks start off as red lines and then get paler.
According to the British Association of Aesthetic Plastic Surgeons (BAAPS), some people naturally ‘make’ better scars than others. In general, patients with black skin or fair freckled skin and red hair tend to produce scars that take longer to heal, such as hypertrophic scars and keloids.
Management options
Many scars will heal over time, but several treatments can be used to make a severe scar less visible. These treatments include:
- Topical silicone gel or silicone gel sheets, which are applied directly to a scar to help soften and flatten it and reduce any itching and discomfort
- Pressure dressings, bandages or garments over a burn or skin graft to flatten and soften scars – these may be used for several months or even years
- Steroid (tape or injections) applied directly (and repeatedly at intervals) to reduce swelling and flatten a scar (e.g. keloid)
- Cryotherapy using liquid nitrogen to freeze keloid scars to stop them growing
- Skin needling involves rolling a small device covered in hundreds of tiny needles across a scar to reduce its appearance
- Surgery may release a tight scar, especially those caused by burns, or use a skin graft.
Pitted scars caused by active acne can be difficult to treat, and many treatments aren’t suitable for the face. It’s sometimes possible to cut out the deep scars or lift them to normal skin level. Dermabrasion and chemical peels may reduce the overall depth of scars and tighten the skin, while dermal fillers may be used to fill in pitted scars. Laser or light therapy can target blood vessels to reduce redness or remove the top layers of skin and encourage collagen to build up to create a flatter scar. All of these treatments should be carried out by a specialist healthcare professional.
Emollient creams don’t seem to have a direct effect on scars, but they can be used to stop a scar drying out and keep it supple. “When a scar is from an operation, such as a C-section, regular massage can help improve the healing process,” says Lesley. “Midwives usually advise women to wait until after their six-week check before beginning to massage a C-section scar. Using a massage oil with a regular massage technique can soften and aid the breakdown of scar tissue and can also reduce the uneven feel and appearance of the skin.”
Eczema skin colouring changes
Eczema can cause changes in normal skin colour, which can be both worrying and distressing. The changes may be caused by active eczema or by scratching, both of which increase the production of melanin pigment (which gives skin its colour).
The skin may develop lighter patches called hypo-pigmentation or darker patches known as hyper-pigmentation. Paler skin may look inflamed with red or dark pink patches; inflammation is harder to see on darker skin and often doesn’t look red. Severe eczema may only become more noticeable on darker skin if pigmentation develops.
Post-inflammatory pigmentation may occur after an eczema flare-up has settled down, and chronic scratching and rubbing can lead to dry, thickened leathery areas of skin with visible markings (called lichenification). These areas are always darker than the surrounding skin – dark pink on pale skin, and slate-grey on darker skin.
Eczema may also cause itchy bumps on the skin, especially on the body and forearms. This is more commonly noticed on darker skin, and any dry skin and scales may show up as a white or grey colour.
Any pigmentation changes can be improved by treating the underlying eczema and inflammation, but the discolouration may last for months and even years, even once the eczema has gone.
Regaining confidence
Everyone who lives with scars copes differently, and how well they cope doesn’t always match the severity, extent or visibility of their scars, according to charity, Changing Faces. Some people are proud of their visible difference and live fulfilling lives, while others find it emotionally challenging and struggle with some (or all) aspects of day-to-day life.
People with scars may be self-conscious and embarrassed and therefore avoid meeting new people. According to research by the Scar Free Foundation, 23 per cent of people with a scar said they have experienced short-term emotional or physical problems. If scarring is significant, and especially if it was caused by burns, patients may be referred to a clinical psychologist to help them come to terms with the emotional impact.
Some people also look for ways to make their scars less visible. Changing Faces’ Skin Camouflage Service involves applying specialist, highly pigmented creams and powders to a scar. These products can match the colour of the scar to that of the surrounding skin (as much as possible) but don’t change the skin’s texture and can’t change raised or indented skin. Skin camouflage can’t be applied to skin that is infected, inflamed, or broken.
“While self-acceptance is vital, having the option of being able to cover their scars, or any other marks, can give people the confidence they need to face the day, whether it’s an important work meeting or a social occasion,” says Leanne. “Other forms of support, from self-help to free one-to-one counselling, are also available so people with visible differences can manage their appearance-related concerns.”
Many organisations provide counselling, advice and support and self-help information to people with scars including: