In Conditions
Follow this topic
Bookmark
Record learning outcomes
Sexual wellbeing – a topic all pharmacy teams will know to treat with tact and consideration – is something many people find awkward to discuss. It requires a depth of knowledge as there are many conditions pharmacy teams need to be able to advise on, from sexually transmitted infections (STIs) to erectile dysfunction. And it is especially pertinent at this time considering the rising levels of STIs in the UK.
A worrying rise
Much of the discomfort people experience when discussing sexual wellbeing issues stem from people thinking that they might make a pariah of themselves in doing so, but many do not realise that these issues are less of a rarity than they think. While this should make the public feel more comfortable in seeking guidance, the increasing rate of STIs is a concern of the UK Health Security Agency (UKHSA), as some conditions have serious long-term health effects. Their latest study revealed STIs contracted in the UK increased by 24 per cent between 2021 and 2022, with a 50 per cent increase in gonorrhoea infections. Richard Angell, chief executive of the Terrence Higgins Trust, believes the surge is due to “the kind of calamitous synergy of crises in this area” referring to funding cuts, the monkeypox outbreak’s added pressure on an already strained system and a lack of prioritisation of sexual health services by the Government.
In comparing 2021 with 2022, the UKHSA found:
- 392,453 STIs were reported in England in 2022
- 50 per cent increase in gonorrhoea infections
- 24 per cent increase in chlamydia infections
- 15 per cent increase in syphilis infections
- Eight per cent increase in number of consultations at sexual health services
- 26 per cent increase in STI diagnoses in those between ages 15-24
- 21 per cent increase in chlamydia infections in young people – yet no increase in testing in this group.
Claudia Estcourt, professor of Sexual Health and HIV at Glasgow Caledonian University, said: “The data published by UKHSA is deeply concerning – levels of gonorrhoea in England are now at the highest ever level since data records began in 1918”, noting that “deep and persistent cuts to the funding of sexual health services across the UK” may be to blame for the explosion in STIs.
The age group most affected by STI transmissions are those aged 15-24, perhaps due to higher rates of partner change during these ages, explains the UKHSA. The Centers for Disease Control and Prevention suggests this may also be due to “young people [being] hesitant to talk openly and honestly about their sex lives” and hence do not understand the causes or means of prevention. Another possibility is that due to their age or perceived age, some young people are not automatically given STI tests when they visit health services. Richard suggests that a reason awareness is low is to do with the stigma surrounding STIs. “The problem is this is the one area where the crisis never breaks out into the media or the general population because it’s so stigmatised.”
“We’ve had a calamitous synergy of crises in this area”
Prevention
Professor Estcourt emphasises that community pharmacies have a huge role to play in combatting sexual illnesses: “Pharmacies have untapped potential in their ability to reach and assist a wide range of individuals, providing they are appropriately resourced and supported by specialist sexual health services.”
Many preventative methods for STIs overlap, and it is good practice to observe them all. Sexually active customers should:
- Use (external or internal) condoms each time sexual intercourse takes place. This significantly lessens the risk of contracting an STI, but does not eliminate it completely
- Use condoms or dental dams during oral sex
- Always use a new condom
- Cover sex toys in a (new) condom with each use
- Avoid sharing sex toys
- Wash sex toys after every use
- Avoid sharing needles
- Avoid touching sores or rashes on others
- If a sexual partner has contracted an STI, do not engage in sexual activity until their treatment is complete and they have tested negative for the infection.
Gonorrhoea, chlamydia, and syphilis cannot be contracted through casual contact, like hugging, sharing baths, swimming pools or cutlery. Misconceptions like these can lead to misunderstanding and stigmatisation, making it even more important for pharmacies to promote factual information.
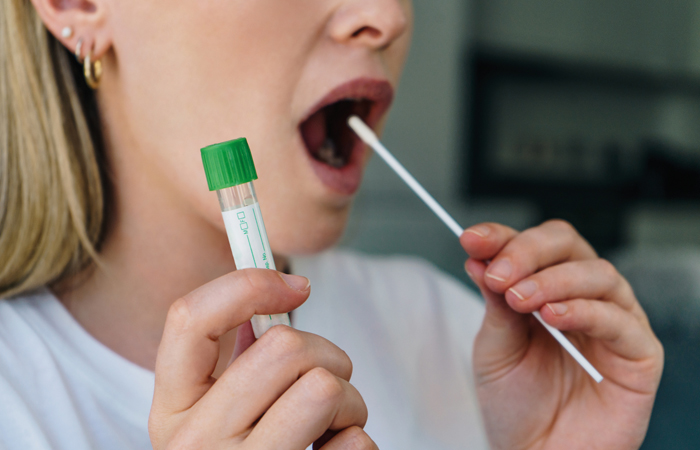
Many STIs show no symptoms if contracted orally, so it’s important to test frequently if sexually active.
Erectile Dysfunction
Many men experience erectile dysfunction (ED), when they are either unable to get an erection or are unable to keep an erection long enough to have sex. ED is often caused by stress, excess alcohol consumption or tiredness, but can also be due to:
- High blood pressure
- High cholesterol
- Diabetes
- Depression
- Anxiety
- Hormonal issues
- As a side effect of some medicines.
There are multiple ways to overcome ED naturally, such as drinking less alcohol (no more than 14 units a week), exercising daily, losing weight if one is overweight, and maintaining a healthy diet. As stress and anxiety are main contributors to ED, taking steps to reduce stressors will also help. Customers can be encouraged to explore self care practices like yoga, meditation, journaling, or therapy.
Alternatively, customers 18 and over can be recommended OTC treatments, now available in the pharmacy. This includes oral tablets containing sildenafil or tadalafil, or stimulating gels. Customers are advised to speak with a healthcare professional when considering using such products.
'The clap’
Gonorrhoea, the most common STI in the UK at the time of writing, is caused by a bacteria which lives in moist parts of the body. It can be contracted in the throat, rectum, penis, or vagina. Found in infected semen and vaginal fluids, it is spread through vaginal, oral, or anal sex or if one touches an infected area and then their own body. Sharing unwashed sex toys is also an easy way for the infection to spread.
Identifying the symptoms, however, is not as simple as identifying the causes. Symptoms can develop within two weeks, but it is common for symptoms to show after months, or not to show at all. One in 10 men do not experience any symptoms, while up to half of women too have no symptoms, according to the NHS. Gonorrhoea in the throat and rectum is mostly symptom-free, however discharge and feelings of discomfort in the rectum may occur. Eye contact with infected semen or vaginal fluid can lead to conjunctivitis.
If symptoms do develop, they may appear as:
- Thin, watery, green, or yellow discharge
- A burning feeling when urinating
- Bleeding after sex
- Bleeding between periods
- Heavier periods
- Pain or tenderness in the lower abdomen.
And in men:
- Swelling of the foreskin
- A burning feeling when urinating
- Yellowish, white, or green discharge from the tip of the penis
- Pain or tenderness in the testicles.
Confirmed infections are treated with a single antibiotic injection – azithromycin or ceftriaxone – or tablet forms are sometimes available.
Care against chlamydia
Another of the UK’s most common STIs is chlamydia, and it is routine for women under 25 to be offered a chlamydia test when visiting health services as a part of the National Chlamydia Screening Programme (NCSP). The NHS recommends that all sexually active persons aged 25 and under in the UK should test for chlamydia yearly, if not after each new sexual partner. This is particularly pertinent if condoms are not used, as chlamydia is passed on through unprotected sex – vaginal, oral, or anal – and through sharing sex toys, the touching of genitals or encountering infected semen or vaginal fluid in one’s eye.
Like gonorrhoea, symptoms are often absent completely. Approximately 70 per cent of women with chlamydia don’t have symptoms and around half of men, according to the NHS, which is why it is so crucial to test frequently.
Chlamydia can be contracted in the throat, rectum, eyes, penis, and vagina. Of the throat there are no symptoms, of the rectum there are usually no symptoms but possibly discomfort or discharge, while the eyes can become red or feel in pain and can produce discharge (conjunctivitis) if infected. Women can experience:
- Pain urinating, in the lower back or belly, in the pelvis or during sex
- Change in vaginal discharge
- Bleeding after sex or between periods.
Men may experience:
- Pain and swelling in the testicles
- Pain urinating
- Burning or itching in the urethra
- White, cloudy, or watery discharge from the penis.
The wait for test results is between seven and 10 days, but people may begin treatment of antibiotics before this if they are highly suspected to be infected. In many cases, Azithromycin will be administered for two to three days, or a longer course of Doxycycline may be prescribed over a week.

In most parts of the UK, people can order STI home-testing kits online.
“STIs contracted in the UK increased by 24 per cent between 2021 and 2022”
One to worry about
Syphilis, one of the more concerning STIs, can lead to serious health issues down the line if left untreated – specifically damage to the heart, brain, and nervous system. It is easily cured with antibiotics, but treatment needs to be administered in the first or second stage of infection. Caused by bacteria, syphilis is easily spread through vaginal, anal, or oral sex. Infection can also occur through contact with an ulcer on a partner’s penis, vagina, anus, the inside of their mouth or contact with a partner’s rash in the second stage. Sharing needles with an infected person is another way the infection can be contracted. A pregnant woman can also pass it on to her baby if she is infected, which can lead to increased risks of miscarriage, premature birth, and stillbirth.
Untreated syphilis can be passed on for up to two years before becoming latent or hidden, which is when it can lead to potentially life-threatening issues. It can take up to three weeks for the following symptoms to appear:
- Ulcers on the penis, vagina, or anus
- Sores in mouth, lips, hands, or bottom
- White or grey warty growths on the penis, vagina or around anus
- A rash on the palms of hands and soles of feet
- White patches in the mouth
- Flu-like symptoms of a high temperature, headaches
- Tiredness
- Swollen glands
- Patchy hair loss on the head, beard, and eyebrows.
Like many STIs, syphilis is treated with antibiotics and may begin before test results return. Antibiotics may be administered in capsule, tablet or injection form and course length will differ depending on how far along the infection is.
Talking about testing
There are many options available to get tested for an STI. Most tests will require a urine sample, a swab from the infected area or, rarely, a blood sample. Customers can set up testing via the National Sexual Health Helpline or visit a sexual health clinic, a contraceptive and young people’s clinic or a private clinic. Another option is to order a self-testing kit from a pharmacy or the NHS to do in private. All testing is free and confidential.
However, there are thought to be numerous issues with testing across the UK as depending on where you live, access to testing may not be readily available. “It is not consistent that you can get a hold of a postal STI and HIV test and where you can get hold of it, there’s often daily or weekly or monthly caps,” explains Richard.
Those aged 15-24 who are sexually active with new or multiple partners should be advised to test for STIs frequently. If test results indicate infection, sexual partners need to be contacted informing them that they may be at risk of infection. As some prefer to remain anonymous, clinics can contact sexual partners without mentioning the infected person’s name. It is also important to inform customers that treatment needs to be completed before engaging in sexual activity again, and customers should be advised to schedule a follow-up appointment to confirm their negative test result.
Richard also noted that now more than ever, people need to make use of their local pharmacy: “There is a vision of community sexual health in which the pharmacy could be your provider of choice for a huge proportion of your sexual health needs.”
Managing the menopause
The menopause is a natural occurrence that happens to anyone who has periods and describes the time when menstruation stops due to lower hormone levels, usually in those aged between 45-50.
Common symptoms can include mood changes, anxiety and problems with memory or concentration, hot flushes, difficulty sleeping, headaches, weight and skin changes, reduced libido and vaginal dryness.
There is much self care pharmacy teams can recommend to customers to cope with these common symptoms, especially focusing on sleep. Customers should try and keep their bedrooms cool, use a fan, and avoid drinking hot drinks before bed. Keeping a regular sleep routine (going to bed and waking up at the same time) will also help improve sleep quality. Caffeine and alcohol prohibit REM (rapid eye movement) sleep so limiting or cutting these out will lead to better sleep, too. Cutting back on alcohol and smoking will positively impact cardiovascular health, sleep quality and can decrease the number of hot flushes and night sweats experienced.
Relaxation techniques like yoga, meditation or journaling are methods customers can use to reduce stress and anxiety levels. Customers experiencing vaginal dryness can try using the OTC treatments available, including tablets, moisturisers and pessaries.

