In Conditions
Follow this topic
Bookmark
Record learning outcomes
With the average person walking an estimated 216,262,500 steps in their lifetime, it’s not surprising that pharmacy teams are often called upon to help customers with feet and leg complaints.
Common conditions
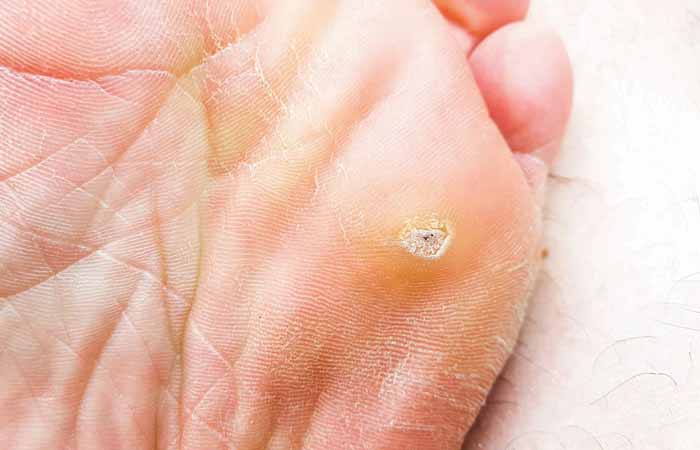
Verrucas
Verrucas are warts on the soles of the feet, with a black dot in the centre surrounded by a harder, white area. It is common to have several verrucas at once and up to 65 per cent resolve themselves spontaneously within about two years. However, over-the-counter (OTC) treatments can tackle them much faster, but must be used with care.
“Salicylic acid preparations (e.g. gels, paints, plasters) work by softening and gradually removing the infected skin, but care needs to be taken to protect the surrounding area when applying the preparations,” explains Jacquie Lee, medication safety officer and information pharmacist at Numark. “Soak the foot in warm water before applying treatment to soften the skin and use a pumice stone or emery board to remove dead skin before reapplying.”
OTC cryotherapy treatments are also available. These freeze the affected tissue but, again, there are risks of the liquid has dripping and causing burns.
General self care advice is to cover verrucas with waterproof plasters in communal areas to prevent spread, and if customers can’t face treating their own verrucas they could see a podiatrist, who can apply stronger treatments such as 70% salicylic acid.
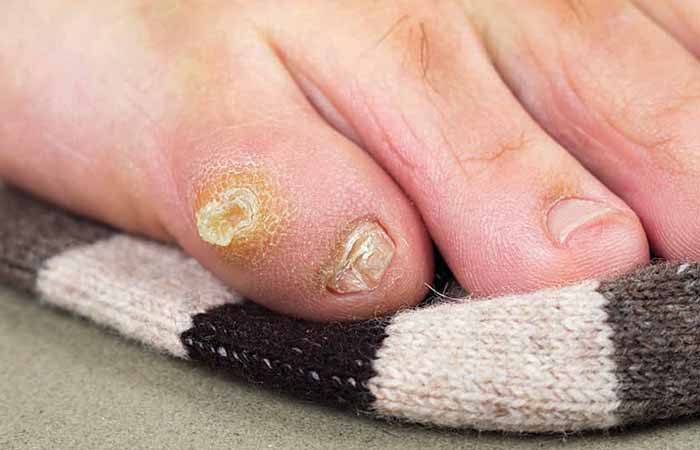
Corns and calluses
Corns are small circles of thick skin that develop on the tops and sides of toes exposed to excessive pressure or friction, such as from ill-fitting shoes.
Wearing correctly fitting shoes should prevent the formation of corns, but if they do appear, Jacquie recommends: “Salicylic acid plasters or pads can help break down thickened skin, protective pads and cushions reduce pressure and friction on affected areas, while moisturising creams help soften the skin and prevent recurrence.”
Untreated corns will become painful unless the pressure that caused them is taken away, so varying footwear every day will avoid continuous pressure patterns.
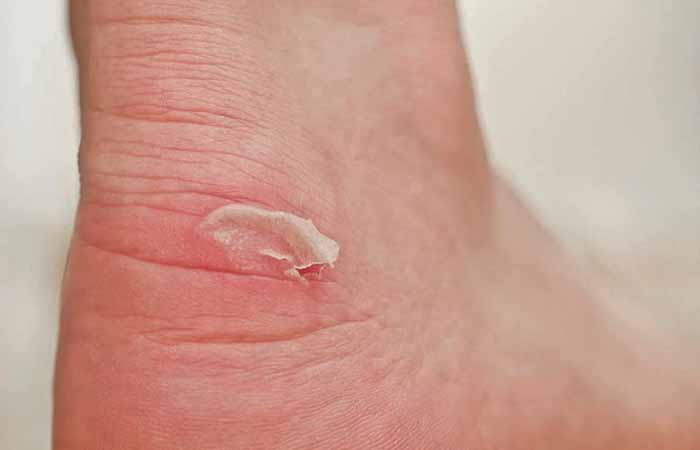
Blisters
Blisters are the skin’s way of protecting itself from excessive heat, moisture and friction, and can be prevented by covering tender spots with a friction-resistant dressing or plaster.
If they do occur, Jacquie recommends: “Hydrocolloid blister plasters can protect the area and promote healing, and antiseptic creams are advised for burst blisters to prevent infection.”
Customers with a blister oozing blood or yellow liquid should be directed to the pharmacist, as this indicates infection.
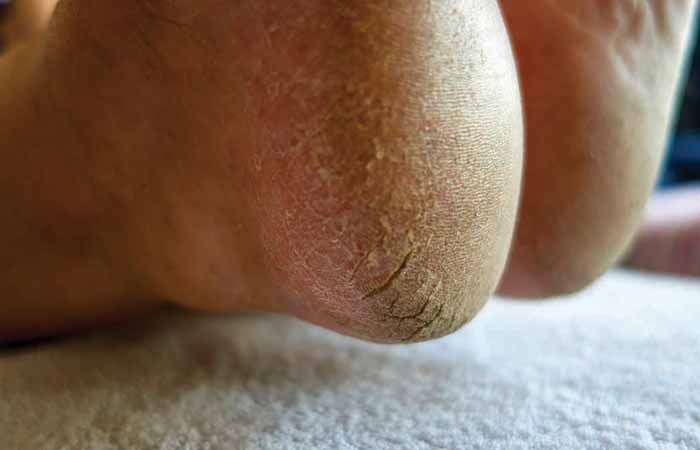
Cracked heels
Cracked heels can be caused by factors including standing up for long periods and wearing thin-soled shoes.
Products containing keratin can repair the cracks and stimulate cell re-growth. Filing the skin once a week can remove hard skin surrounding the cracks, followed by using a product containing a high urea content to attract water and lock it into the skin.
“Encourage daily moisturising, especially after bathing,” says Jacquie. “Recommend wearing socks after applying creams to enhance absorption and suggest cushioned footwear to reduce pressure on heels.”
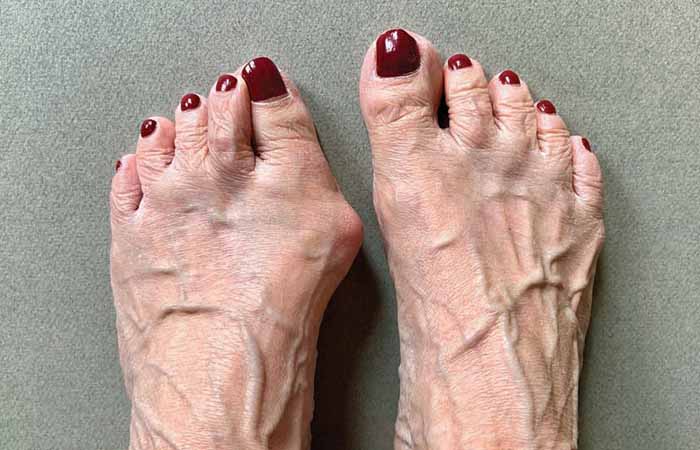
Bunions
A bunion is a deformity in which the big toe angles towards the second toe and leads to a bony lump on the side of the foot. Most bunions are genetic, but poorly fitting footwear makes the problem worse by squeezing the toes together.
Although some treatments can ease the pain of bunions, only surgery can correct them. However, the Royal College of Podiatry says some measures can prevent them in the first place, such as wearing sensible, well-fitting shoes, opting for wider shoes that provide toes with room to move, and keeping heel height to no more than 4cm.
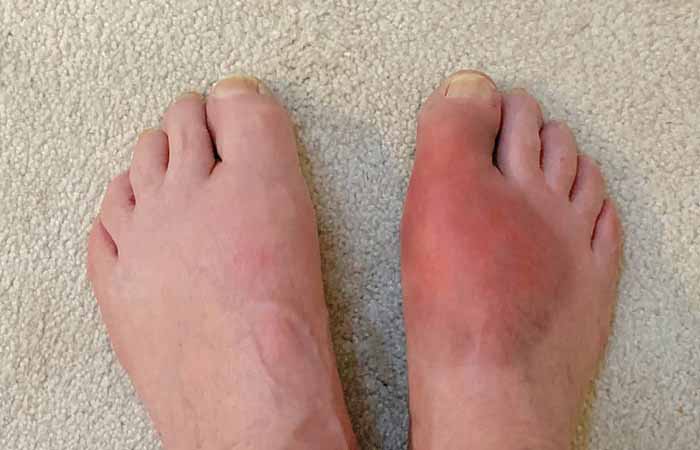
Gout
Gout is a type of arthritis caused by having too much uric acid in the blood that causes sudden, severe pain in a joint – usually the big toe, but it can be in other joints in the feet, ankles, hands, wrists, elbows or knees – and hot, swollen, red skin over the affected area.
People might have a higher chance of getting gout if they are overweight, drink alcohol, have been through the menopause, take medicines such as diuretics, or medicines for high blood pressure (such as ACE inhibitors), have high cholesterol, high blood pressure, kidney problems, osteoarthritis or diabetes, or have had surgery or an injury.
An attack of gout usually lasts a couple of weeks if left untreated. Non-steroidal anti-inflammatory (NSAID) painkillers such as ibuprofen can help the pain, but if the patient does not get treatment, future attacks may last even longer, and cause lasting damage to joints. People who have frequent attacks or high levels of uric acid in their blood may need to take uric acid-lowering medicine.
Gout can come back every few months or years, but making healthier lifestyle choices can prevent future attacks. Pharmacy teams can advise customers to maintain a healthy weight, try not to drink more than 14 units of alcohol a week, exercise regularly, and quit smoking.
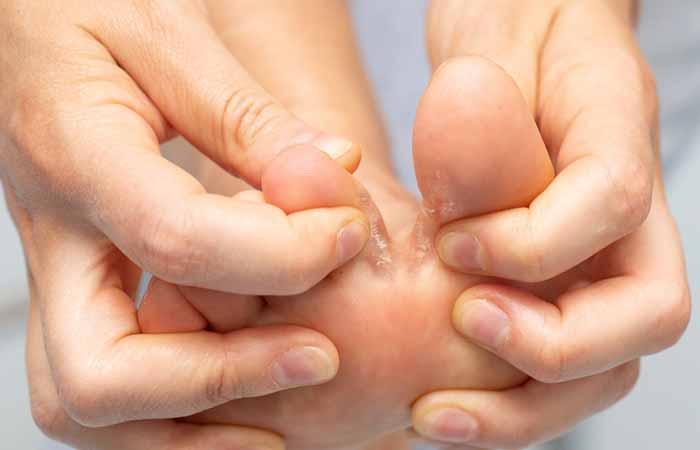
Athlete’s foot
The itchy, scaly, cracked skin of athlete’s foot – also known as tinea pedis – is a common skin infection that will affect around a quarter of all adults at some time in their lives. Caused by a combination of bacteria and fungus, it creates dry and cracked skin – usually between the toes – as well as blisters.
“Customers can be recommended antifungal creams to use directly on the feet,” says Reshma Malde, pharmacist at John Bell & Croyden. “Antifungal powders as well as sprays can be used in shoes and socks and are useful for keeping feet dry and preventing reinfection from fungal spores in the shoes.”
Several antifungal ingredients are effective in treating athlete’s foot. “Imidazoles such as miconazole and clotrimazole work by killing the fungus,” Reshma explains. “They should be applied twice daily to the affected area until the skin looks normal again and treatment should continue for an additional two weeks to ensure all fungal spores are killed and to avoid the infection returning.”
If the condition doesn’t improve, or if there is severe pain, redness, or signs the infection has spread, Reshma advises consulting the pharmacist or GP, “especially for people who are diabetic or have a weakened immune system”.
Plantar fasciitis
Plantar fasciitis is a common cause of pain on the bottom of the heel and occurs when the plantar fascia ligament that supports the arch of the foot becomes irritated and inflamed.
Pain relief can be offered to manage symptoms. “Paracetamol and/or NSAIDs, either oral or topical such as ibuprofen, can be recommended for short-term relief of pain and inflammation,” says Reshma.
“Pharmacy teams may also recommend orthotic insoles, such as arch supports or heel cushions or gel cushion insoles, to relieve pressure on the plantar fascia. Stretching exercises targeting the calf and plantar fascia are particularly useful during the first four to six weeks, alongside using an ice pack wrapped in a towel on painful areas for 15-20 minutes at intervals through the day.”
For longer-term relief and prevention, self care is key. “Stop activities that could be causing the pain, such as long periods of standing, and reduce high-impact activities like running,” advises Reshma. She also recommends wearing comfortable cushioned shoes with good arch support and a small heel, such as laced trainers, rather than flat slip-ons and avoiding going barefoot.
Whether it’s recommending the right antifungal for athlete’s foot, providing self care tips for cracked heels, or identifying red flags that require medical referral, pharmacy teams are well equipped to support customers with their foot and leg health. By combining product knowledge with attentive questioning and tailored advice, staff can help prevent minor issues from escalating and keep customers confidently on their feet.
“By combining product knowledge with attentive questioning and tailored advice, staff can help prevent minor issues from escalating”
Diabetes care
People with diabetes have to take extra care of their feet because they are at risk of a decrease or lack of sensation in their lower limbs due to neuropathy. This means that unless they check their feet regularly, they can miss small wounds, blisters or the beginnings of foot infections, which can quickly worsen or turn into ulcers.
Charity Diabetes UK advises that people with diabetes should check their feet every day to spot the signs of any problems quickly and stop them from becoming serious complications:
- Take off shoes and socks
- Touch both feet and check their temperature – they should both feel the same and not be cold or hot
- Check feet for calluses, blisters or scabs, or any changes in the shape or colour
- Check in between toes for dry or flaky skin
- Ensure toenails are not too long and are not digging into the skin.
It is also important to advise any customers with diabetes to remember to keep their blood sugar under control, as elevated blood glucose reduces their body’s ability to fight infection and slows down wound healing.
If a customer is experiencing pain or a wound does not appear to be healing, they should be referred to their GP or a podiatrist.
A leg up
Pharmacy teams can be on hand to support customers with common leg concerns with OTC treatment and advice.
Deep vein thrombosis (DVT)
DVT is a type of blood clot most commonly formed in the leg, causing swelling, pain and discomfort. It is a serious condition which, if left untreated, can lead to fatal blood clots in the lungs – called pulmonary embolism (PE) – with 30-50 per cent of people who develop DVT going on to have long-term symptoms and disability.
While long distance travel is a risk factor for DVT, it doesn’t just affect people who have been on a flight. Sitting down for prolonged periods can lead to slow blood circulation, which increases the risk of developing a blood clot within a deep vein in the body.
The risk also increases if a person has pre-existing risk factors including a history of DVT or PE, blood clotting abnormalities, cancer, a recent surgery or injury, is pregnant, has varicose veins, mobility problems, or is living with obesity.
Preventative measures include moving around as much as possible, avoiding alcohol and keeping well hydrated. Anti-embolism stockings (AES) or graduated compression stockings (GCS) can also be useful, and pharmacy teams should ensure they know how to advise customers on how to buy the correct type and size of stocking and wear them correctly.
“30-50 per cent of people who develop DVT go on to have long-term symptoms”
Sciatica
Sciatica occurs when the sciatic nerve which runs from the lower back down to the feet becomes irritated or compressed. While the condition often improves within a few weeks to a few months, it can persist for longer in some cases and may recur.
Symptoms typically affect the lower back, buttocks, and the back of one leg, often extending to the foot and toes. Common signs include a sharp, burning pain running down the leg, tingling sensations similar to pins and needles, numbness, and muscle weakness.
Physiotherapist Sammy Margo from Deep Heat & Deep Freeze says self care for sciatica involves a combination of cold and hot therapy with the focus on cold therapy in the initial inflammatory and very painful stage.
“Cold application increases blood flow and decreases pain, and after the initial inflammatory phase, switching to heat can help relax muscles and soothe pain,” says Sammy. “In addition, it’s also important to stay active, so gentle exercises like walking, swimming, or yoga can help improve mobility and reduce pain.”
Pharmacist Mark Burdon, advisor to Combogesic, says over-the-counter pain killers can help reduce pain and inflammation. “Try a combination product containing paracetamol and ibuprofen for a faster onset of pain relief, than paracetamol or ibuprofen alone.”
Varicose veins
A varicose vein is one that has become swollen and twisted due to weakness in the vein wall and poor circulation associated with a sedentary lifestyle, overweight or pregnancy. Symptoms include tired, heavy legs; aching, painful legs; leg cramps and swollen ankles.
Conventional treatment options are support stockings and/or surgery to remove or collapse the veins. However, Ali Cullen, nutritional practitioner and educational manager at A.Vogel, says customers seeking an alternative may decide to try horse chestnut seed extract (HCSE). “It is thought to act to tone the veins and make the capillaries less permeable,” explains Ali.
“The tannins it contains may give it an astringent action on the vein wall, and it is also thought to reduce the activity of an enzyme involved in the breakdown of the vein wall. However, because HCSE contains constituents that may irritate the gastrointestinal tract, it is best taken in a gastro-resistant format (enterically coated to prevent it breaking down in the stomach) after food, to avoid irritating the stomach lining, and it is not suitable in pregnancy or breast-feeding, so gels can be smoothed onto the legs as an alternative to taking horse chestnut internally.”