Tackling oral health
In Conditions
Follow this topic
Bookmark
Record learning outcomes
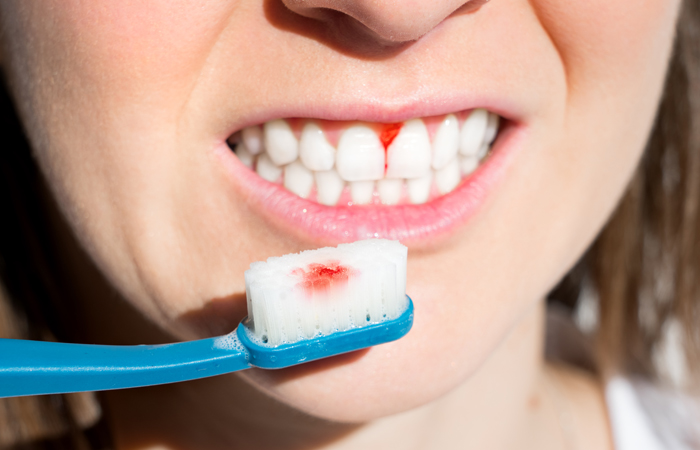
One of the first signs of gum disease is blood when brushing the teeth. With dental practices disrupted by the pandemic, many people are turning to community pharmacy for support with their oral health
Just as GP surgeries’ doors closed during lockdown, many dentists’ doors did too, leaving the UK population with a significantly reduced access to oral health care and support. But according to a new survey by the charity the Oral Health Foundation and oral care brand Colgate in January 2021, it wasn’t just this access that dwindled – people’s attitudes to oral health did too.

Some 55 per cent of British adults reported feeling that they had neglected their teeth during lockdown. More than one in three people reported toothache during the pandemic, with nearly one in 10 experiencing the pain for longer than two weeks. The Oral Health Foundation has voiced its fears that an increase in untreated tooth decay could lead to a sharp rise in the number of people having costly extractions in the future.
Dr Nigel Carter, chief executive of the Oral Health Foundation, says that healthcare professionals, including members of the pharmacy team, should be on hand to get people’s oral health back on track, especially as “the pharmacy may be their first port of call” when such problems arise. “It is imperative that community [pharmacies] don’t miss the opportunity to educate customers on good oral health practices,” he says.
Reassure and react
The research also shows that almost one in five people haven’t seen a dentist for over two years. Although dentists closed early on in the first lockdown, most dental practices are now back to relative normality. Yet one in four people have been searching online to fix their oral health problems at home rather than visiting a dentist. The reasons for this are unclear, but whether it’s not knowing that they’re open, or a concern about Covid-19, pharmacy teams can reassure customers that visiting their dentist is both safe and necessary.
This is particularly true for the one in five people who said they have been eating unhealthier foods and one in 10 who have been drinking more alcohol during the pandemic. Poor oral hygiene, diets high in carbohydrates and sugar, increased alcohol consumption and infrequent dental visits all increase a person’s risk of gum disease and tooth decay.
To promote healthy oral care habits, Dr Carter recommends that pharmacy teams and their customers get involved in oral health campaigns. “National Smile Month, which takes place between 17 May and 17 June this year, provides a great opportunity for pharmacy teams to help spread vital oral health messages,” says Dr Carter. “Later in the year, in November, we also run Mouth Cancer Action Month, which aims to raise awareness of mouth cancer and educate the public on the signs, symptoms and risk factors.”
Oral care routines
In the survey, around one in six people admitted to not brushing their teeth as much as before the pandemic, while almost one in five said they haven’t been brushing their teeth twice a day. According to the Oral Health Foundation, of those people who do brush regularly, many don’t clean between their teeth with an interdental brush or dental floss so they’re still not achieving the best standard of oral care.
“Knowing that fewer people are brushing twice a day is disastrous for oral health,” says Dr Carter. “Along with consuming less sugar, it is one of the best ways to prevent tooth decay. Brushing last thing at night and at one other time during the day with a fluoride toothpaste takes four minutes out of the day – an important and proactive step for self care and something to prioritise.”
The Oral Health Foundation recommends that adults use a small to medium-sized toothbrush head with soft to medium, multi-tufted, round-ended nylon filaments. The head should be small enough to reach into all parts of the mouth, especially the back, although a second brush could be used specifically for those hard-to-reach places. Pharmacy customers can buy specialised brushes, such as softer-bristled brushes for sensitive teeth, and toothbrushes with large handles and angled heads if they have reduced dexterity.
“Community pharmacy teams can encourage customers to look for the ‘Oral Health Foundation Approved’ logo on the oral health products they buy,” says Dr Carter. “This logo, which has been providing reassurance to consumers for nearly 30 years now, means that the claims made by the product in question have been scrutinised and evaluated by an independent panel of scientific experts. It means that a customer can buy the product in the knowledge that not only is it safe to use, it can also do what it claims to do.”
55 per cent of British adults feel they have neglected their teeth during lockdown
Water fluoridation plans

In February 2021, the secretary of state for health Matt Hancock confirmed plans to remove the barriers to water fluoridation schemes in the UK. If implemented, this will help to ease the process of water fluoridation for local communities and give the nation’s oral health a much-needed boost.
The addition of fluoride to water has been researched for over 75 years, and this process has been proven to reduce tooth decay by 35 per cent. Fluoride can greatly improve dental health by strengthening the tooth enamel and making it more resistant to tooth decay. Currently, only one in 10 households in England receive tap water containing the recommended level of fluoride. People living in areas with fluoridated water have been shown to have lower rates of tooth decay than those who don’t.
The Oral Health Foundation, which has been lobbying for water fluoridation to be extended for many years, has welcomed the plans. “In recent years, we have seen water fluoridation proposals repeatedly stall at local authority level due to high cost, competing demands and limited budgets,” says Dr Nigel Carter, chief executive of the Oral Health Foundation. “All the while, tooth decay continues to be the most common chronic disease in the country. Tooth extractions, most of which are caused by decay, remains the most common reason for hospital admissions of five- to nine-year-olds in the UK. Yet, this is a totally preventable disease. We believe that water fluoridation is the single most effective public health measure there is for reducing oral health inequalities and tooth decay rates, especially among children.”
Common oral health problems
From the teeth to the gums, there are many different conditions that can affect the mouth, and most can be managed through a good oral care routine.
Tooth decay
According to the Oral Health Foundation, new data shows more than 30 million adults in the UK have one or more fillings, showing just how widespread tooth decay is. In its early stages, tooth decay doesn’t cause any symptoms, but it can lead to sensitivity to sweet things, toothache, an unpleasant taste in the mouth and a dark spot on the surface of the tooth.
“When it comes to keeping tooth decay at bay, a customer’s greatest weapons are their toothbrush and a fluoride toothpaste,” says Dr Carter. “Adults and children over three years should use a toothpaste with 1350ppm to 1500ppm (parts per million) of fluoride. Everyone should brush twice a day for two minutes and should spit rather than rinse out the toothpaste once they are done.”
Early tooth decay can be treated with a fluoride varnish applied to the tooth, and a filling to repair the tooth. If the nerve in the middle of the tooth is damaged, the dentist may need to perform root canal treatment. If the tooth is very badly decayed, the tooth may have to be removed.
“If a patient is already suffering with tooth decay, it may be worth them using a high-fluoride toothpaste, upwards of 5000ppm fluoride,” says Dr Carter. “A high-fluoride toothpaste can help a customer get their oral health back on track and is especially useful for those who are more vulnerable to tooth decay. This includes the elderly, dry mouth sufferers or those on medications that cause dry mouth, people with diabetes and people with high-sugar diets. A high-fluoride toothpaste can only be purchased on prescription so if you believe a customer could benefit it from it, encourage them to book an appointment with their dentist.”
Gum disease
Around 90 per cent of UK adults have some form of gum disease, which causes red, swollen gums and can affect their overall health. “In recent years, severe gum disease has been linked to an increasing risk of diabetes, dementia and strokes,” Dr Carter says. “And just last month [February 2021] a study came out linking it to Covid-19 complications. The first sign of gum disease is blood on your toothbrush or in the toothpaste you spit out after brushing. Your gums may also bleed when you are eating, leaving a bad taste in your mouth and your breath may also become unpleasant.”
If a pharmacy customer is experiencing symptoms of gum disease, they need to take steps to treat it. “Regular and effective brushing, as well as daily interdental cleaning with interdental brushes or floss, is usually enough to nip it in the bud,” says Dr Carter. “It may also be worth investing in an electric toothbrush, which studies have shown to be more effective than manual brushes when it comes to removing plaque from your teeth and gums. However, if problems persist, customers should be encouraged to book an appointment with their dentist.”
Bad breath
Many people don’t realise they have bad breath, but the Oral Health Foundation has a simple test they can try. Just lick the inside of the wrist and sniff – if it smells bad, then it’s likely their breath does too.
Bad breath is often caused by a build-up of bacteria on the teeth, or bits of foods getting stuck between the teeth. Using a mouthwash containing antibacterial agents or chewing sugar-free gum may help. But customers shouldn’t use a mouthwash to disguise their bad breath, as they need to sort out the underlying cause. Persistent bad breath has lots of causes, including smoking, a dry mouth, acid reflux or even crash dieting.
“If a customer complains of bad breath, the first questions to ask are about their oral health routine,” says Dr Carter. “Are they brushing twice a day for two minutes with a fluoride toothpaste? Are they cleaning in between their teeth? Often, an effective oral health routine will eliminate bad breath. However, if they have tried to address the issues at home and the bad breath persists, they should be encouraged to contact their dentist. It could be sign of a more serious oral health problem, such as gum disease or even mouth cancer.”
Sensitive teeth
According to the Oral Health Foundation, most people suffer from some tooth sensitivity, but the problem is more common in people aged 20-40. Sensitivity may be caused by brushing too hard, receding gums, gum disease or tooth grinding. Most people with sensitive teeth get the pain when drinking or eating something cold, but occasionally also experience this with hot, sweet or acidic foods.
“Having sensitive teeth can mean anything from getting a mild twinge to having severe discomfort that can continue for several hours,” says Dr Carter. “It can also be an early warning sign of more serious dental problems so it’s important it is addressed. Several brands of toothpaste on the market that aim to ease sensitive teeth may help. If the sensitivity doesn’t clear up, encourage the customer to book an appointment with their dentist.”
Dental erosion from eating sugary or acidic foods regularly is another common cause of sensitivity. Pharmacy customers should be advised to have acidic food and drinks, including fizzy drinks, just at mealtimes. Finishing a meal with cheese or milk, or chewing sugar-free gum, may help to cancel out the acid.
Mouth cancer
In 2019, more than 8,700 British adults were given the news that they had mouth cancer. According to the Oral Health Foundation, cases of mouth cancer in the UK have nearly doubled in the last 20 years, yet seven in every 10 people are unable to identify the early warning signs and symptoms and 83 per cent of people don’t feel confident enough to do a mouth cancer check at home.
Mouth cancer is most common in the over-40s. Most cases are linked to smoking and alcohol, but recent reports have also linked it to the human papillomavirus (HPV). Each year in the UK, more than 2,300 people die from mouth cancer, with many of these deaths being preventable. Many people are unaware that lumps or swellings in the mouth, head or neck are potential signs of mouth cancer, and persistent hoarseness may also be a link.
Dr Nigel Carter, chief executive of the Oral Health Foundation, says it’s important for everyone to know how to spot the early signs of mouth cancer. “Look for mouth ulcers that don’t heal within three weeks, red or white patches in the mouth and unusual lumps or swellings in the mouth or head and neck,” he says. “Most mouth cancers appear on the tongue – around a third of all cases – but it can also strike on the tonsils, gums and lips. It can also be found on the roof or floor of the mouth, as well as the throat.”
