In Conditions
Follow this topic
Bookmark
Record learning outcomes
A staggering one in five adults in the UK are deaf or have hearing loss or tinnitus and, according to a survey from the Royal National Institute for Deaf People (RNID) in 2022, even though 98 per cent of adults said that their hearing was important to them, only six per cent of adults without diagnosed hearing loss had taken a hearing test in the last 12 months.
Hearing loss can affect all aspects of daily life, including communication, relationships and employment, and can lead to mental health problems, such as depression. Looking after our ears properly can help to prevent many ear problems, including infections, a build-up of earwax, earache, and hearing loss. It may also prevent problems with balance, such as vertigo.
Earwax
Earwax is an oily substance in the ear canal. It usually falls out of the ear naturally over time but sometimes it builds up, leading to issues such as pain, tinnitus and hearing loss. Scratching or cleaning the ears, especially with cotton buds, can push the wax further into the ear. “Wax helps to protect our ears from infection and traps dust and debris from entering the ear canals,” says Hilary Harkin, acute advanced clinical nurse practitioner. “In the same way that some people sweat more than other people, some people can produce more wax.”
Excess earwax only needs to be removed if it’s causing problems, including hearing loss or affecting how well hearing aids work. It can often be softened at home using ear drops usually containing olive oil, almond oil or sodium bicarbonate from a pharmacy. “These drops can be used three to four times a day for three to five days,” says Richard McKearney, audiology adviser at RNID. “There are certain situations where medical advice needs to be sought to determine if using ear drops is safe, such as if someone has a perforated eardrum. National guidelines recommend that GPs offer earwax removal if the earwax build-up is causing problems.”
An estimated 2.3 million people in the UK require professional earwax removal every year. However, a report by the RNID in January 2024 revealed that fewer than half of Integrated Care Boards (ICB), the commissioners of most NHS services, are providing wax removal services in line with public health guidelines. Some parts of England don’t commission the service at all. Many people are either suffering in silence or paying for expensive private services, costing up to £100 for each appointment. “If customers decide to have wax removed this way, they should make sure the person they see is a suitably qualified professional, and check that they use a safe method of wax removal such as ear irrigation or microsuction,” adds Richard.
Dry, itchy ears
Many people get dry, itchy ears from time to time. This may be more common in people who already have eczema or seborrheic dermatitis. It’s also common during the menopause. “If you suffer with dry skin, use olive oil ear spray on a weekly basis and your usual skin care moisturising ointment around the outside of the ear if it feels dry,” says Hilary. “Often, it can be caused by shampoo and soap itching your ear. To keep ears dry when bathing, use a 50p-sized piece of cotton wool at the entrance to the ear canal and coat the outside of the cotton wool with petroleum jelly to repel water.”
Improving accessibility
Hearing loss can be very isolating. According to new research from the Royal National Institute for Deaf People (RNID), in May 2024, 22 per cent of people with hearing loss said that most people ignore them in public settings; this increases to 42 per cent for deaf people and 59 per cent for people who use British Sign Language (BSL). Richard McKearney, audiology adviser at RNID, recommends several ways to make community pharmacies more accessible for people with hearing loss:
- Have a separate consultation room or a quiet space away from the main pharmacy
- Ensure good lighting – some people with hearing loss rely on lip reading so need to be able to see the face of the speaker clearly
- Install a hearing loop to enable people with compatible hearing aids to hear what the pharmacist is saying directly through their hearing devices
- Train staff in deaf awareness through the RNID (rnid.org.uk)
- Learn BSL to aid communication
- Make sure customers can contact the pharmacy via email or text as well as phone. Some people with hearing loss use Relay UK, and Deaf British Sign Language users may wish to contact the pharmacy in BSL through video remote interpreting.

Pharmacy teams can provide more inclusive care to the hard of hearing community by learning sign language.
Middle ear infection
A middle ear infection (acute otitis media) is particularly common in young children, but anyone can be affected. Usually caused by a viral infection, it triggers inflammation and a build-up of fluid behind the eardrum. The main symptoms are earache, a fever, vomiting, a lack of energy, and slight hearing loss. Young children may rub or tug at their ear, not react to some sounds, not feed properly, and be irritable or restless. Middle ear infections can’t be prevented but several things can increase a child’s risk, including passive smoking, using dummies in children older than 12 months, and bottle feeding rather than breastfeeding.
Not everyone with a middle ear infection needs to see their GP as the symptoms often get better on their own after three to five days. Paracetamol or ibuprofen can treat pain and fever. Placing a warm cloth over the ear may help too. Using an ear drop containing an anaesthetic and an analgesic may ease the pain – this can be prescribed by a pharmacist as part of the Pharmacy First scheme.
If the infection isn’t clearing up, or there’s a lot of pain or discharge, customers should speak to their GP, as they may need antibiotics. “Red flags include severe ear pain, sudden hearing loss, discharge from the ear accompanied by fever, dizziness or balance problems, persistent or recurrent ear infections, or any other concerning symptoms that don’t improve with self care measures,” says George Sandhu, deputy pharmacy superintendent at Well Pharmacy.
Outer ear infection
Outer ear infections (otitis externa) are caused by inflammation of the external ear canal. This may be due to a bacterial or fungal infection, an allergy or irritation, such as getting water into the ear when swimming. Damage to the ear canal (e.g. from a finger or cotton bud), wearing hearing aids or having eczema can increase the risk.
The symptoms include pain, itching, discharge, reduced hearing, pain in the jaw, and a full feeling in the ears. Acetic acid drops or sprays can be bought over-the-counter to treat mild symptoms in adults. More severe symptoms may need prescribed antibiotic drops or spray with or without a corticosteroid.
“Many people are either suffering in silence or paying for expensive private services”
Market monitor
Otinova® is a fast-acting ear spray that helps relieve symptoms of otitis externa or swimmer’s ear, explains manufacturer Kestrel Medical LTD. Containing aluminium acetate, which has an astringent effect, the spray acts quickly and covers a range of pathogens known to cause ear inflammation, adds the company. Free of antibiotics and steroids, Otinova has an antibacterial and antifungal effect and is recommended for those aged five years and over presenting with symptoms of ear canal inflammation, particularly those exposed to water regularly, explains the company.
Kestrel Medical LTD: otinova.co.uk
Glue ear
Glue ear (otitis media with effusion) is caused by a build-up of fluid in the middle ear with no signs of inflammation or an infection. It’s particularly common in young children, and is a common cause of ear discomfort, tinnitus and hearing loss. Glue ear often gets better on its own without any treatment, however, it can affect children’s behaviour, concentration levels, language development and day-to-day life. According to the National Institute for Health and Care Excellence (NICE) guidance published in August 2023, there’s no evidence that corticosteroids, antihistamines or decongestants can be used to treat glue ear. Antibiotics are also not effective. “Nasal hygiene is important, so encourage the parent or carer to teach their child how to blow their nose,” says Hilary. “Smoking in the house increases the likelihood of glue ear so give smoking cessation advice if necessary.”
A GP may suggest autoinflation, which helps to open the Eustachian tube so that fluid can drain out. This involves blowing up a balloon using a nosepiece attached to one nostril, while closing the mouth and other nostril. Older children may be able to do this without using the balloon.
If glue ear is causing hearing loss, hearing aids or grommets may be recommended. Grommets are small plastic tubes that sit in a hole in the eardrum, and let air get in and out of the ear more easily.
“Wax on top of the ear drum has been known to cause balance concerns”
Dealing with earwax safely
- DO remove earwax with over-the-counter olive oil eardrops or sprays
- DO seek medical advice if the wax isn’t clearing up at home or is causing severe symptoms
- DO contact the GP surgery to see if there is a local NHS ear removal service (or find a local qualified practitioner)
- DON’T insert anything into the ear – no fingers, cotton buds or tissues – as this may push ear wax further in
- DON’T use ear candling to remove wax, as this can cause burns.
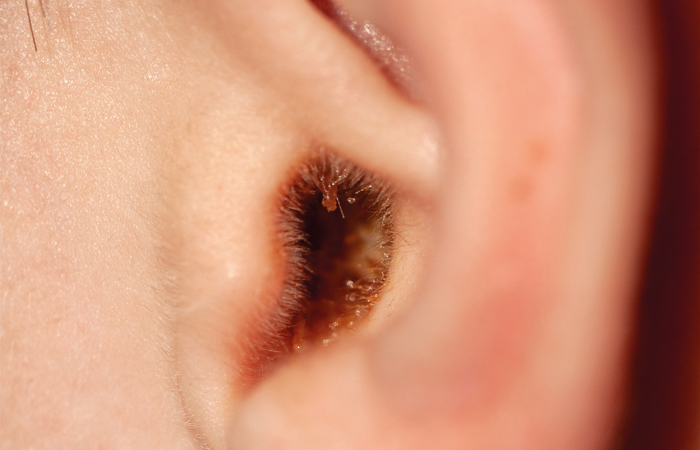
A build up of earwax can cause issues such as hearing loss and tinnitus.
Tinnitus
Tinnitus (hearing sounds inside one or both ears) usually comes and goes. The sounds vary from person to person, from ringing and buzzing to humming and hissing. The causes of tinnitus aren’t fully understood, but it may be triggered or worsened by stress or excess earwax. “Around one in seven adults have tinnitus all the time or regularly,” says Richard. “Most often, it’s linked to hearing loss or other ear conditions. It’s rarely a sign of a serious condition. The NHS website advises people to see their GP if they have tinnitus which is regular or constant, if their tinnitus is getting worse, or it is bothering them – for example affecting their sleep and concentration.”
Tinnitus often improves over time. Customers can try relaxation techniques and mindfulness, regular exercise, a better sleep routine, cutting down on caffeine, and cognitive behavioural therapy (CBT) or counselling. Many people find that distraction helps, such as listening to soft music or background sounds. Tinnitus re-training therapy may be available on the NHS for severe or persistent symptoms. This uses sound therapy to re-train the brain to tune out the tinnitus. If there’s any hearing loss, hearing aids may be recommended. Customers can also be directed to a local or national tinnitus support group. “It’s very important to listen to people describe and talk about their tinnitus as it can be very distressing,” says Hilary. “Point them to support centres and tinnitus counsellors, who are available on the NHS – the GP can refer them.”
Children will often tug and itch their ear if they are having issues.
Dizziness and vertigo
Vertigo feels like you or everything around you is spinning or moving. It’s more than just feeling dizzy, which is an umbrella term for feeling lightheaded, unsteady or woozy. An attack of vertigo can last for a few seconds to several hours. In severe cases, it can last for days or even months. “Sometimes balance can be affected as you get older, but it can also be related to an ear problem,” explains Hilary. “Wax on top of the ear drum has been known to cause balance concerns, so removal can help.” Vertigo is usually due to a problem with the inner ear, caused by an infection (labyrinthitis), migraine or some medicines. With benign paroxysmal positional vertigo (BPPV), specific head movements cause vertigo. Ménière’s disease is a rare inner ear condition that can cause vertigo, tinnitus and a loss of hearing.
Vertigo often gets better without treatment but it’s important to see a GP if it keeps coming back or is affecting daily life. During a vertigo attack, lie still in a quiet, dark room to reduce the spinning feeling, move your head carefully and slowly during daily activities, and sit down straight away when you feel dizzy. A GP might prescribe antibiotics if vertigo is caused by an infection, or prochlorperazine or antihistamines to aid balance. Specific exercises may help to improve balance in BPPV.
Pharmacy First for earache
As part of the Pharmacy First service, community pharmacies can assess and examine children aged one to 17 with earache, to check for signs of a middle ear infection. Pharmacists taking part in the scheme can look inside a child’s ears using an otoscope. “We can offer guidance on self care measures, such as using over-the-counter pain relievers (ibuprofen or paracetamol) and applying warm compresses to the affected ear,” says George Sandhu, deputy pharmacy superintendent at Well Pharmacy. “A pharmacist can also offer ear drops and oral antibiotics if patients require and meet the eligibility criteria. If necessary, customers should visit their GP for further evaluation and treatment.”


