In Conditions
Follow this topic
Bookmark
Record learning outcomes
Slips, trips and falls are leading causes of home and workplace injuries, and community pharmacies are often the first port of call for first aid advice when a minor injury occurs.
Pharmacies stock a wide range of wound care products, from basic plasters and antiseptics to more advanced dressings, so it’s important that pharmacy teams know about different types of wounds and how to treat them effectively.
Open wounds
Most people will have an open wound from time to time. In many cases, minor cuts can be treated at home, but wounds that are large, deep or won’t stop bleeding usually need medical care, such as stitches. There are five types of open wound – abrasions, lacerations, incisions, punctures and avulsions:
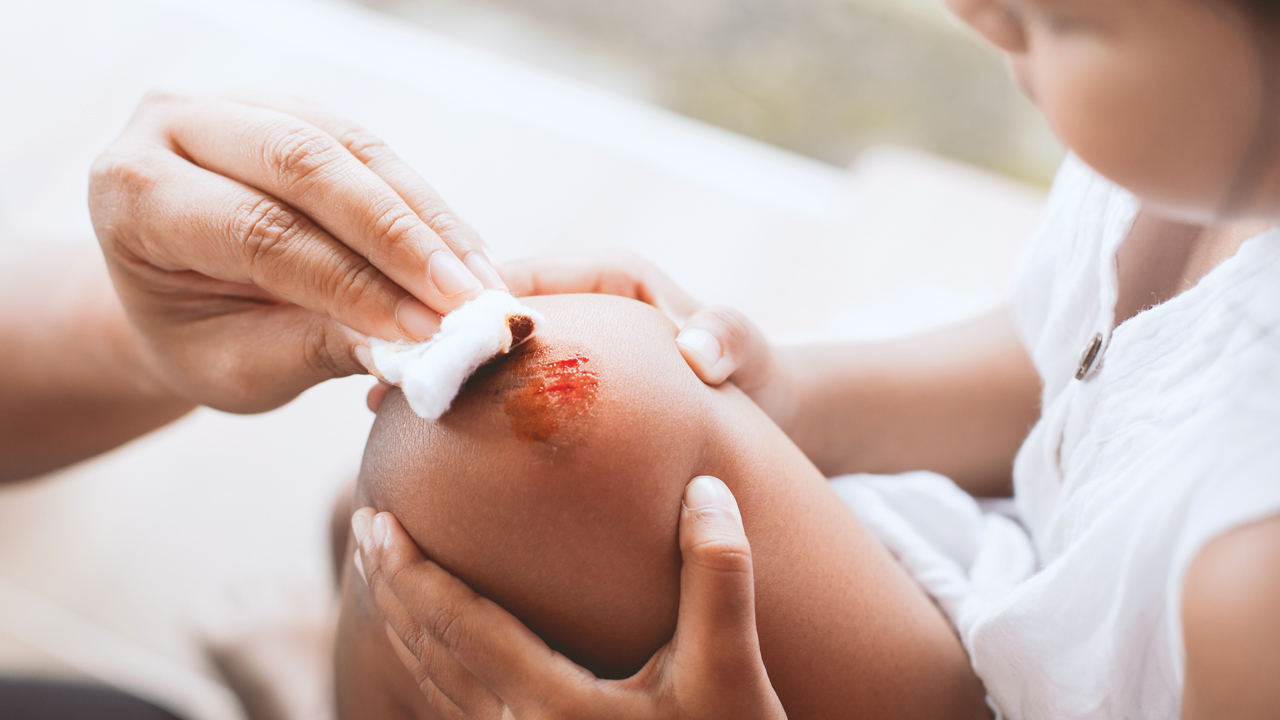
- Abrasions (grazes) happen when skin rubs or scrapes against a rough surface. These affect only the outer layer of the skin (epidermis), so there usually isn’t much bleeding, if any. Young children are particularly prone to grazing their knees or elbows. Most of the time, grazes are not serious, but they can still feel sore
- Lacerations are deep, messy tears in the skin, usually from a sharp object such as a knife or broken glass or even a paper cut. There may be significant bleeding, along with jagged wound edges that need stitching to prevent scarring. Lacerations often affect parts of the body that are close to the bone, such as the knees, elbows, shins and forehead
- Incisions are clean, straight cuts caused by a sharp tool or object. These can bleed heavily and damage underlying tissues, such as muscles and nerves. Common causes include kitchen knives, scissors, broken glass, and surgery. The edges of incision wounds are smooth, which means they usually heal more quickly and are less likely to cause scarring than laceration wounds
- Puncture wounds are small, often deep holes caused by a long, pointy object such as a nail, animal tooth, needle or – in extreme cases – a bullet. These wounds tend to close quickly because the external hole is small, which means they don’t always bleed much. However, they can be deep enough to damage internal tissues and may be prone to infections
- Avulsions are serious injuries that usually need immediate surgical treatment. The skin and tissue underneath are partly or completely torn away, and the wound bleeds heavily and quickly. This can happen during car crashes, animal attacks, explosions or shootings.
Closed wounds
Closed wounds don’t break the skin’s surface, but underlying tissues and organs may still be damaged. These are usually caused by blunt trauma. There are various types of closed wounds:
- Contusions (bruises) are caused by damage to the small, shallow blood vessels under the skin. They cause tenderness and colour changes (typically red or purple at first, eventually fading to yellow or brown)
- Haematomas are pools of blood under the skin formed by damaged larger blood vessels. They tend to be deeper and larger than normal bruises and are often lumpy and painful. Most bruises are flat and clear up on their own, but a haematoma may not show up on the skin’s surface and may take several months to heal
- Blisters (small, fluid-filled pockets) are often caused by friction, burns and skin irritation. Blister fluid is usually clear, but it can sometimes contain blood or pus.
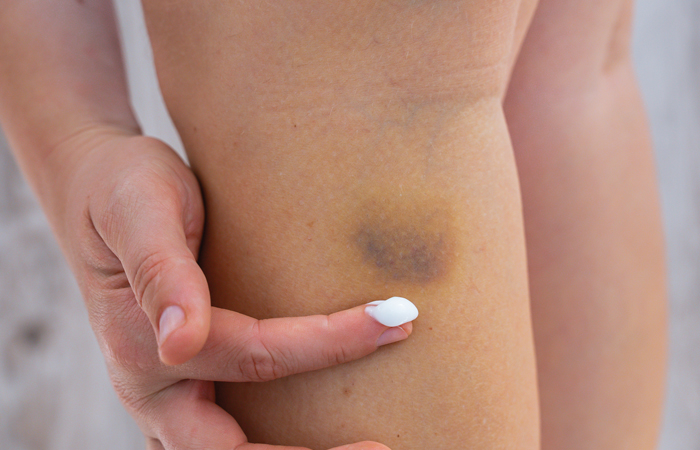
Bruises can take days to weeks to heal, depending on the severity.
Some over-the-counter creams can help with pain levels and healing times.
Looking after infected wounds
If a wound isn’t healing and has worsening pain, swelling and redness, it may be infected. The wound or surrounding skin may feel hot to the touch and leak discharge or pus.
Infected wounds take longer to heal and can be serious if the infection spreads.
Mild infections can usually be managed at home with regular care and monitoring. This involves bathing the wound with warm water and a clean cotton pad and applying an antiseptic cream and sterile dressings.
But if the wound is large or deep, the redness is spreading or the wound begins to ooze, patients should be referred to the pharmacist straight away.
More serious infections may need prescribed antibiotics (topical or oral). Generalised symptoms such as fever and aches and pains are signs of sepsis, which needs urgent medical care and intravenous antibiotics. If a wound contains soil, dirt or other debris, patients may need a tetanus vaccination.
Antimicrobial dressings containing silver, iodine or honey may be used for infected wounds or wounds at a high risk of infection, but these are not recommended for routine use.
Caring for wounds
Most minor open wounds, such as surface cuts and grazes, start to heal in a few days, whereas more serious wounds may need to be treated by a medical professional. If there is a risk of an infection, antibiotics or a tetanus booster jab may be recommended.
To stop the bleeding in a minor wound, pressure should be applied with a clean cloth or bandage, and the wounded area raised to reduce swelling.
If there is something stuck inside the wound, it should not be removed as this could cause more damage. Instead, it should be covered with a clean, moist cloth or bandage, pressing firmly around the object to push the edges of the wound together and control any bleeding.
It is important to clean cuts and grazes by rinsing them under running water or using a sterile wipe. The wound can then be gently patted dry with a gauze swab and the area around it cleaned with soap and water.
A sterile dressing or plaster can then be applied. Oral painkillers such as paracetamol or ibuprofen can ease associated pain, if required.
Bruises and shallow haematomas can usually be treated with ice, an ice pack or a cold compress for 15 to 20 minutes to reduce pain and swelling.
Advise customers that ice should not be placed directly onto the skin as this can cause an ice burn. Severe bruising or a haematoma may need further investigations to check for internal damage.
Dressings and plasters
Choosing the correct covering for wounds is important, as a dressing provides the optimal environment for healing. This can speed up the recovery time, reduce the risk of infections and prevent scarring.
- Washproof and waterproof plasters are suitable for everyday use and are less likely to come off in a bath or shower. Fabric plasters are more flexible and durable, making them ideal for joints, but they are not waterproof
- Fabric dressings can be cut down to suit different sizes of wounds, while shaped plasters (for fingertips or very small areas, for example) are also available
- Film dressings are ideal for minor cuts and grazes that are not bleeding very much or at all, but these are very sticky so are not suitable for fragile skin (e.g. in older people)
- Hydrocolloid dressings and plasters absorb wound fluid, so they are particularly useful for blisters, minor burns and shallow ulcers
- Hydrogel dressings contain a gel that hydrates wounds, making them ideal for dry burns.

Cuts and grazes should be cleaned with running water before applying a dressing.
“Around five million people in the UK have scars that cause physical or emotional distress”
Scars
According to the Scar Free Foundation, one in three people in the UK have a scar – that’s around 20 million people.
Wounds that take a long time to heal are more likely to leave a noticeable scar. Some scars fade over time, although this can take two or more years, whereas other scars don’t fade much or at all.
Everyone copes with scarring differently, and around five million people in the UK have scars that cause them physical or emotional distress.
Scars vary in how they look. They may be flat, sunken or raised, and coloured or white. They may look slightly different depending on the person’s skin tone, their location, the type of injury that caused them, and the person’s age and overall health. However, different types of scars have specific characteristics that make them easier to recognise.
- Fine line scars are common, often occurring after a minor injury or surgery. They may be slightly raised at first, but will eventually flatten and fade without any treatment. The scar may be itchy for the first few months
- Hypertrophic scars are raised and firm but will fade and flatten over time. These don’t usually grow any bigger than the original wound and are most common after a burn injury
- Keloid scars are raised, hard and smooth and tend to be red or darker than the surrounding skin. They are bigger than the original wound and don’t tend to flatten or fade without treatment. Keloid scars can form after a minor injury or an infected wound and are more common in people with darker skin
- Atrophic scars look like deep, small holes in the skin, or a sunken mark. They can form after acne or chickenpox and rarely disappear on their own
- Contracture scars feel tight and constricting, which can affect movement. These tend to be caused by burns and may look red and shiny until the scar heals.
Scar management
Scar management aims to make scars less noticeable, improve movement and support patients to cope with changes to their appearance. The sooner a scar is treated, the more effective the treatment will be.
The most suitable treatment will depend on the type of scar and its severity. First-line treatments include wearing prescribed pressure garments, using silicone gel sheets and massage.
Pressure garments
Pressure garments are designed to provide a precise amount of constant pressure over a wound to limit the growth of scar tissue. These tight, made-to-measure, lycra-containing garments may be prescribed for people with severe burns to reduce the risk of hypertrophic scarring.
Pressure garments are worn day and night and only removed to treat the scar with massage or silicone. They may need to be worn for up to two years.
Scar massage
Massaging a scar several times a day with a moisturising cream, oil or lotion may help to reduce itching. Massaging in circles along the scar with the tips of the fingers helps to boost blood circulation, which can soften the scar and improve the absorption of moisturising products.
Scars should only be massaged once the wound is fully healed, and it can take at least three months of massage to see any benefits.
Silicone products
Silicone products can help to moisturise healed scars and improve their appearance, as well as relieving itching and discomfort. Silicone gel is a clear, self-drying gel that can be applied to the affected area.
Silicone is also available in gel sheets – soft and flexible wound dressings that can be placed onto the skin for several hours at a time.
Camouflage products
Some people may want to make their scars less noticeable, in which case skin camouflage products may be suitable. These are highly pigmented creams and powders designed to match the surrounding skin.
They are waterproof, suitable for the face or body, and can stay in place for two or three days at a time. However, they cannot change the texture of the skin, alter raised or indented skin or be applied to infected, inflamed or broken skin. Some people may be able to obtain these products on prescription.
Specialist treatments
Specialist scar treatments don’t guarantee the complete removal of scars, but they aim to make them less visible. They may be suitable for severe scarring or scarring that is causing physical or emotional symptoms but are not always available on the NHS.
Options include steroid injections to reduce swelling and flatten the scar, and laser or light therapy to reduce redness or remove the top layers of a thickened or pitted scar. Other treatments include cryotherapy to freeze keloid scars, dermal fillers for pitted scars, and microneedling.
Surgery is an option for more serious scars, especially those caused by burns.
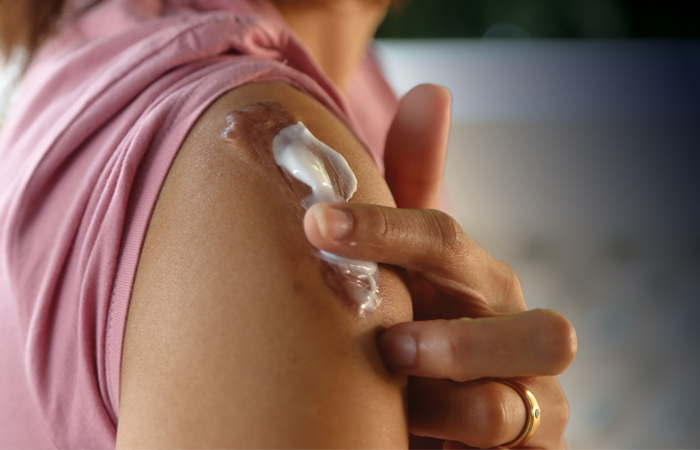
Customers can massage a scar several times a day with a lotion, oil or gel, but this should only be done once it is fully healed.
Living with a scar
Scars can have a significant impact on a person’s daily life. They can be very itchy due to nerve damage, and may also be painful and uncomfortable since scar tissue does not stretch or grow.
People with more substantial scarring may find it difficult to stay cool because scar tissue does not have any sweat glands either, and their skin may be dry if oil-producing glands have been damaged.
It may be painful to move around if scar tissue forms over a joint. However, exercise is important as it can prevent the skin from contracting and tightening.
Sun exposure should be avoided as scar tissue burns easily; using a sun block is essential.
Scars can have a significant impact on self-esteem, and around one in three people with visible scars experience depression or anxiety.
Specialised counselling is available through organisations including the Scar Free Foundation (scarfree.org.uk), Changing Faces (changingfaces.org.uk) and the Katie Piper Foundation (katiepiperfoundation.org.uk).