In Conditions
Follow this topic
Bookmark
Record learning outcomes
Our eyes are extremely complex, vital organs, but until they experience a problem with their sight, many people overlook their eye health. Getting regular check-ups can prevent and halt a number of eye health issues in their tracks, but there are plenty of things that the pharmacy team can spot – and advise on – to help customers prevent eyesight failure and other eye health problems.
The most common eye conditions that affect people in the UK are:
- Age-related macular degeneration (AMD) – this causes problems with the central vision which can become distorted or blurry, and is significantly affected by diet and smoking
- Glaucoma – a hereditary condition which causes optic nerve damage due to changes in the pressure in the eye. This can lead to loss of peripheral (side) vision and blindness if not managed with daily drops
- Diabetic retinopathy – the main cause of sight loss in the under-60s in the UK, this causes the central vision to become patchy making it difficult to read and drive
- Cataracts – a very common eye condition as we age, causing the lens inside the eye to change and become less transparent
- Retinitis pigmentosa – a group of inherited eye conditions that affect the retina at the back of the eye causing permanent changes to eye sight
- Lazy eye in children – also called amblyopia, this is when the vision in one eye does not develop properly, with treatment options including wearing glasses, using eye drops, or even surgery
- Light sensitivity (photophobia) – this causes discomfort or pain in response to normal levels of light or glare, which can then result in eye strain and headache/migraine.
Helping with eye health problems
Thankfully there is much that pharmacy teams can do to identify customers who may need help with eye problems. “Being aware of specific patient groups at increased risk of poor eye health is a great place to start,” says David Cartwright, optometrist and chair of the charity, Eye Health UK.
“For instance, smokers have a significantly greater risk of sight loss and higher propensity to suffer conditions such as dry eye or general eye irritation, so asking a patient who signs up for your pharmacy’s smoking cessation programme or purchases quit smoking products how their eye health is and whether they are up to date with routine eye tests could help benefit that patient. Most smokers know that their habit increases the risk of cancer or lung disease but fewer than one in 10 is aware of the link between smoking and sight loss.”
People with diabetes are another group who have increased risk of poor eye health. “Again, asking about a patient’s eye health when dispensing repeat prescriptions for diabetes medication can make a real difference to your patient’s wellbeing,” says David.
“Perhaps one of the most common small pieces of advice is for those patients who are on eye drops for glaucoma: after instillation, do they occlude the puncta [the small funnel-like drain hole found in the inner corner of the upper and lower eyelids] so the drop has more time to absorb?”
Other patient groups at increased risk of poor eye health include contact lens wearers, screen users and people who are obese. Some common medicines such as birth control pills, antidepressants, cardiovascular drugs or medication such as tamoxifen can also have eye health side-effects. David suggests that “it may be beneficial to include a notice about this on your pharmacy labels when dispensing these medicines”.
Spring allergies (hayfever) and winter respiratory infections also cause a spike in patients requiring OTC eye care products.
“Know the signs of conditions such as conjunctivitis or blepharitis so you can confidently assist in selecting appropriate OTC remedies”, says David, “and most importantly for any of the ‘at risk’ groups [over 60s, diabetics, smokers, etc.] advise that they have a regular sight test, every two years, which is vital to prevent avoidable sight loss”.
OTC products that may help
Many eye problems can be treated with over-the-counter (OTC) products and advice in the pharmacy, says Kenny Chan, Numark lead information services pharmacist.
For example:
- Vision – If a patient is struggling to read or see objects clearly, it could be a problem with their vision. In this case they may need glasses
- Infections – Conjunctivitis can cause discharge from the eye itself. Chloramphenicol eye drops or ointment can be used to treat the infection in patients over two years old.
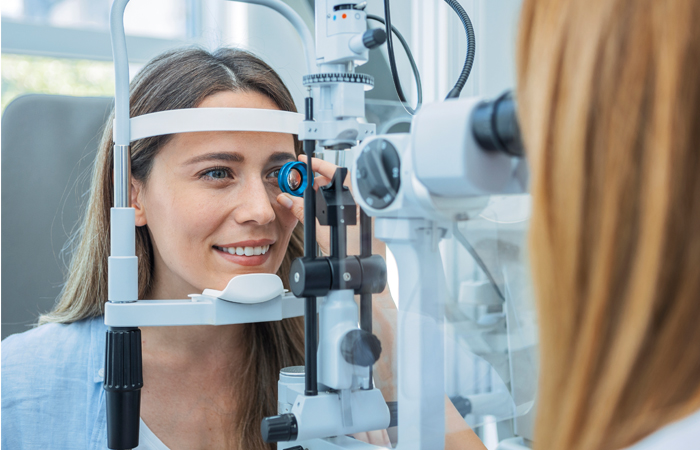
Customers should be encouraged to have a sight test, not just for their vision, but their eye health.
For infections of the skin surrounding the eye, such as styes and blepharitis, use of warm compresses to unblock the gland and eye wipes to help clean the area should be recommended
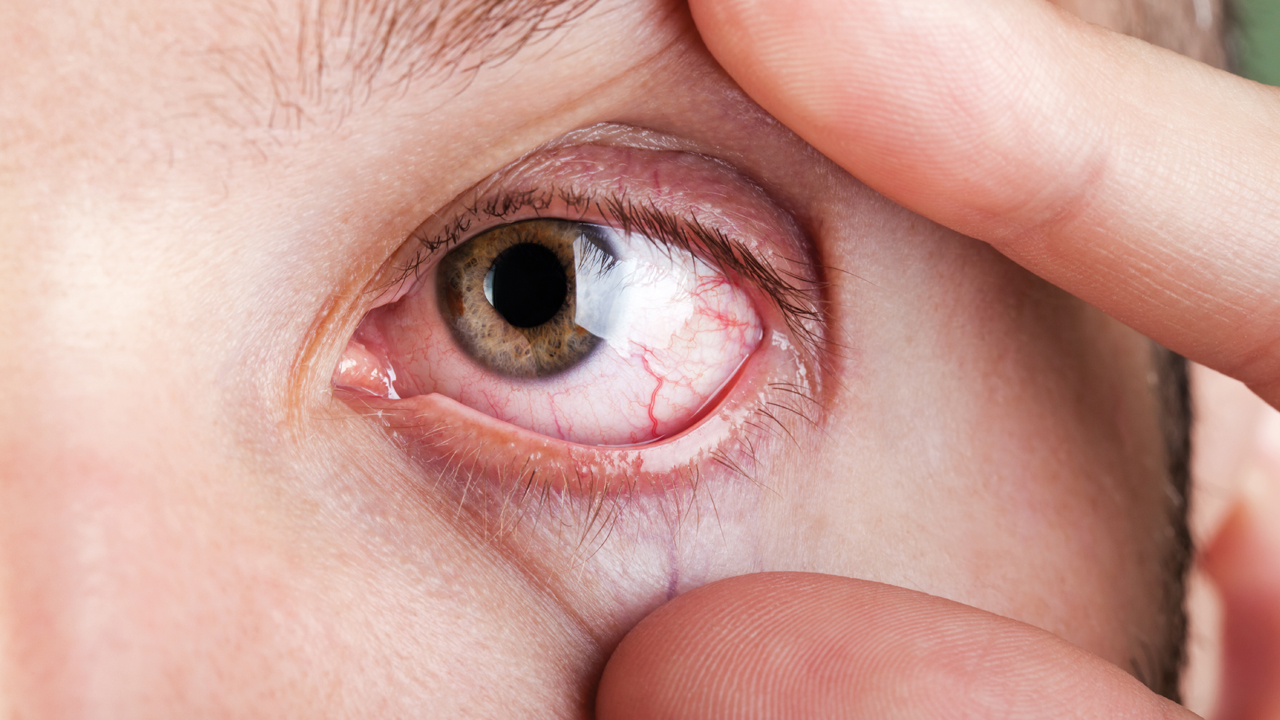
- Red eyes – Red eyes are very commonly presented in pharmacies, caused by burst vessels in the eye. Products containing naphazoline can reduce the size of blood vessels and can be used to treat bloodshot eyes
- Allergies – Often allergies such as hayfever can affect the eye, leading to watery, itchy eyes. Eye drops such as sodium cromoglicate can help relieve the symptoms
- Irritants – Irritants are something physical in the eye that is directly causing an irritation, such as hairs, pet fur, dust. An eye wash can be used to flush out any irritants.
When to refer to the pharmacist
Some common eye conditions do not have very many symptoms, if at all, in the early stages, so it is always important to encourage patients to attend regular sight tests as recommended by their optometrist.
However, where patients do present with eye or vision symptoms that are not easily distinguishable for a particular cause, they should be referred to the pharmacist who will be able to effectively triage and manage them, including referral where necessary.
“For some non-sight threatening eye conditions, treatment is available from pharmacies without prescription so provided the diagnosis is clear from symptoms, and management of these conditions are within their scope of practice – such as dry eye and bacterial or allergic conjunctivitis – then pharmacists should be able to provide advice and offer treatment where appropriate,” says College of Optometrists clinical adviser, Dr Paramdeep Bilkhu.
“Where there is doubt about an eye condition, then referral to the optometrist as first contact is recommended, as they have the relevant knowledge, skills, experience and access to equipment to accurately diagnose and manage eye conditions.”
When to refer to other eye care professionals
Although there is much the pharmacist can do to help, there will also be times when it is vital to know when to refer a patient on to other eye health professionals.
“It is crucial to find out if the person has had an eye examination already to establish the cause of the symptoms. If not, colleagues in optometry are perfectly placed to do that,” says Roshni Kanabar, clinical adviser at the Association of Optometrists.
Roshni advises that some red flag symptoms to look out for are pain, decreased vision and light sensitivity, and it’s important to remember that contact lens wearers are also more of a concern, as contact lens related eye infections can be sight threatening and treatment is time sensitive.
“Patients should be referred to an optometrist if they are experiencing problems with their vision as they are able to prescribe glasses and contact lenses and detect signs of underlying general health conditions, such as diabetes, high cholesterol, and high blood pressure.”
Whatever interventions the pharmacy team makes – all the experts agree that the best way to help patients to keep their eyes healthy and protect their vision is to encourage them to always go for their regular sight tests every two years, or more often if recommended by an optometrist.
Dry eye
Dry eyes are a very common problem caused when not enough tears are produced to moisturise the eyes. “Dry eye is the most common cause of eye irritation in older people with as many as a third of over-65s suffering from the condition, while people with diabetes have a 50/50 chance of suffering with dry eye syndrome,” says David Cartwright, optometrist and chair of the charity Eye Health UK.
Symptoms of dry eye include: a sandy-gritty irritation that gets worse as the day goes on, dryness, a burning sensation, excessive watering – which some patients may be surprised to hear is a symptom – as well as itchy, red or tired eyes, or a feeling of dust in the eye.
“Some staff are proactive in going beyond the immediate problem in front of them, identifying potential changes in patients’ daily lives which might contribute to eye-related complications,” says Tania Cork, pharmacist and member of Théa UK’s EYE (Expert on Your Eyes). “For example, spending a long time looking at screens can cause problems like dry eye disease.
“Staff can also often extend their expertise when speaking with patients – for example, if someone is seeking to purchase contact lens solutions, they could also be suffering from dry eye disease, or if patients have comorbidities such as diabetes, pharmacy staff can check to see if they’ve had their eyes tested recently.”
A wide range of lubricants are available in pharmacies to help combat dry eyes, which come as eye drops, gels and sprays. However, David cautions: “For dry eye it is important to remember that there may be a number of reasons for this and there are different types of drops for dry eye to address the underlying cause so refer for a sight test to your optometrist, who may specialise in dry eye disease.”
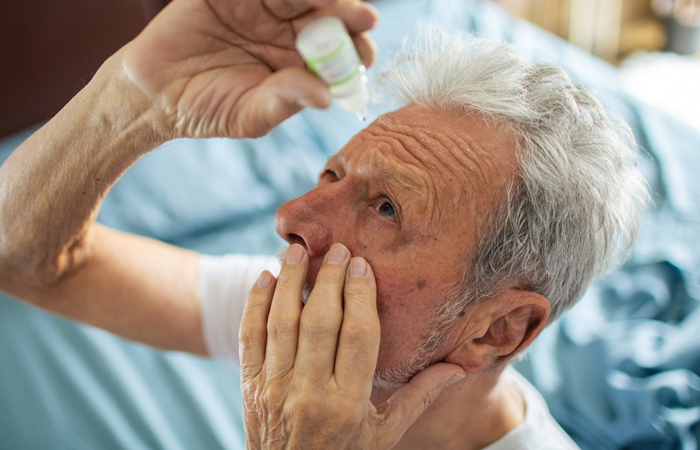
“Dry eye is the most common cause of eye irritation in older people”
Improving accessibility
Customers with vision challenges can find it hard to navigate around retail environments, so there is much to consider when it comes to making the pharmacy a welcoming and accessible space for people who are blind or have impaired vision.
“The concept of accessibility in pharmacy can be approached in two ways,” says Tania Cork, pharmacist and member of Théa UK’s EYE (Expert on Your Eyes). “The first involves considering the physical structure and layout of the building, a challenge in terms of adaptability to the diverse needs of patients; and the second perspective delves into the accessibility of medicines, exploring how easily patients can navigate the products and retain information.”
Many pharmacy staff already have good relationships with their customers, often recognising signs of blindness or visual impairment through frequent interactions, yet Tania says: “Distinguishing between varying degrees of visual impairment, especially compared to complete blindness, can be complex.”
In terms of physical structure and layout, Tania suggests pharmacies should consider having ramp access to the pharmacy and making sure aisles are wide enough and free from obstacles or ill-placed display units, so visually impaired people can find it easier to navigate around.
“Those who are severely visually impaired will have a white cane to support them when walking, to identify obstacles and as an indicator to others that they are visually impaired, so consider having high contrast edges for steps and shelf edges to help those detect objects easier,” she adds.
It is also important to ensure that all staff members are attuned and sensitive to the potential presence of patients with visual impairments – especially new customers. “Enhancing product accessibility can involve various tactics, including providing large-print labels, offering braille versions of informational leaflets, and reinforcing written information with verbal communication,” says Tania.
Patient medication records (PMR) also serve as vital repositories for information, allowing pharmacies to tailor their services to the unique needs of their customers, especially those with visual impairments. “The close relationships often nurtured between local pharmacies and patients with visual challenges facilitate a personalised approach to care,” adds Tania. “Which means staff members familiar with the specific requirements of these patients can better cater to their needs.”