In Conditions
Follow this topic
Bookmark
Record learning outcomes
Some customers may spend all day on their feet – much like the pharmacy team – whilst others could be sitting at their desks for hours on end. Both scenarios have implications for the legs and feet, sometimes leading to swelling, aches and pains.
For most people, this can be offset by regular breaks or some handy self-care tips like elevating the legs where possible, but some customers may be affected more seriously.
With the help of experts from the Royal College of Podiatry (RCP), we explore the various conditions customers may look to pharmacy teams for help with – including oedema.
What is oedema?
“Oedema is a build up of excess fluid in the tissues of the body, which causes visible swelling. It most often affects the feet, ankles and legs, but can occur in the hands, arms, face or abdomen,” says Patrick McGill, member of the vascular podiatry specialist advisory group of the RCP. “The affected area may look puffy or swollen; the skin can appear stretched or shiny, and pressing a finger into the skin may leave a temporary dent (pitting oedema). Oedema can be temporary or established as a chronic condition known as lymphoedema.”
Anyone can be affected by oedema as it is caused by common occurrences like insect bites or prolonged
standing or sitting. Patrick says, however, that certain things put people at higher risk of developing the condition:
- Being overweight or physically inactive
- Pregnancy
- Standing or sitting in the same position for long periods (e.g. on long shifts or journeys)
- Eating a lot of salty food, which can make the body retain fluid
- Having varicose veins or chronic venous insufficiency
- Those taking certain medicines, including some blood pressure medicines (e.g. calcium channel blockers), some hormones (such as HRT or some contraceptives), steroids and some antidepressants.
Oedema can also be a sign of a medical problem, such as:
- An injury like a sprain, strain or fracture
- Insect bites or stings
- Heart, kidney or liver problems that affect the body’s
fluid balance - A blood clot in the leg (deep vein thrombosis)
- Infections in the skin or soft tissues, such as cellulitis
- Thyroid problems (usually hypothyroidism)
- Lymphatic system changes.
Treatment options
While there can be many causes of oedema, there are an obvious set of symptoms pharmacy team members should look out for. One of the main symptoms is swelling in one or both feet, ankles or legs, or occasionally in the hands, arms, face or abdomen, says Patrick. Other symptoms may include a feeling of heaviness or tightness in the limbs; shoes feeling tighter; the skin looking stretched or shiny, and possible pitting (indentation) when pressed; possible aching and a reduced range of movement, and, “in more serious cases, breathlessness, chest discomfort or generalised swelling may be reported”.
If the oedema is benign – i.e. caused by things such as pregnancy, hot weather, standing all day or minor injury – Patrick advises pharmacy teams to share self-care tips and over-the-counter treatment where possible to ease discomfort. “Elevate the legs above hip level several times a day, and when resting. Avoid standing or sitting in one position for long periods and encourage regular movement and calf muscle ‘pumping’,” he says. “Avoid tight clothing or footwear around the thighs, calves or ankles, encourage a healthy weight and regular physical activity and reduced salt intake.”
Pharmacy teams can also recommend the RICE principles (rest, ice, compression elevation) where appropriate – for example, if the swelling is caused by a sprain or strain – and cool compresses to ease minor swelling.
If compression and supports are necessary, double check with the pharmacist before recommending properly fitted compression hosiery. This can help with mild, chronic venous oedema, varicose veins, or ‘heavy legs’, says Patrick, “but should be avoided if there is sudden, unexplained unilateral swelling, suspected deep vein thrombosis (DVT), severe peripheral arterial disease, skin infection or heart failure”.
As far as over-the-counter solutions go, Patrick advises simple analgesics such as paracetamol to help with discomfort. “Topical treatments – for example, soothing creams for insect bites – may help where there is an abrasion with no systemic features,” he adds.
Whether recommending lifestyle changes or an OTC treatment, Patrick says pharmacy teams must always check the duration of the swelling, whether it is one-sided or in both legs, if there is pain, redness, warmth, shortness of breath or chest pain, and if the customer has a long-term condition or is currently taking any other medication – including OTC products.

Compression hosiery can help to improve blood circulation and alleviate pain in the legs, ankles and feet by applying gentle pressure.
“Fungal infections affect up to eight per cent of the population but are much more frequent in older adults”
Oedema alarm bells
Oedema can be serious, and sometimes requires further action. “For community pharmacy support staff, having a clear ‘refer to pharmacist/GP/999’ structure is useful,” says Patrick. Customers with the following symptoms should be referred for same-day GP or urgent care:
- Sudden onset of swelling in one leg, ankle or foot without an obvious minor injury
- Swelling that is painful, hot, red or tender, especially if one-sided (possible DVT, infection or inflammatory cause)
- Swelling that is severe, worsening quickly, or has appeared suddenly
- Swelling in a limb plus fever, feeling shivery, generally unwell or signs of spreading infection
- New or worsening swelling in someone with known heart, kidney or liver disease
- Swelling in several body areas without a clear explanation
- Oedema that has not improved after a few days of self-care or is recurring without explanation
- New oedema in someone who is pregnant, particularly in late pregnancy, especially if associated with headache, visual disturbance or abdominal pain (possible pre-eclampsia – local guidance may specify immediate assessment).
Oedema accompanied by any of the below will require a call to 999:
- Shortness of breath, difficulty breathing or breathing worse when lying flat
- Chest pain, tightness, heaviness or palpitations
- Coughing up blood
- Marked dizziness, faintness, confusion or feeling very unwell
- Sudden, severe one-sided leg swelling, particularly if it is painful, red and warm, in the absence of obvious minor injury (suspected DVT or pulmonary embolism)
- Rapidly expanding swelling after significant trauma.
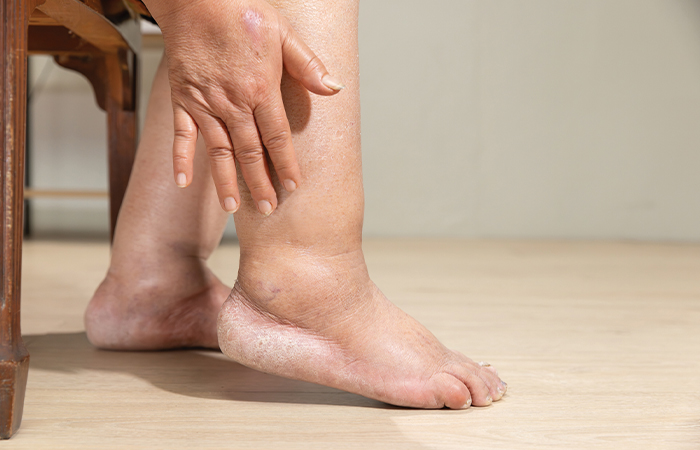
Oedema causes visible swelling and can be serious, depending on the cause.
The right shoes
Chief clinical advisor to the Royal College of Podiatry, Dr Helen Branthwaite, says the right shoes can make all the difference to foot health. Ideally, she says, shoes should fit the width of the foot across the widest part, have an adjustable method for the shoe to stay on, such as laces or Velcro, across the middle of the foot, and have a thumb nail’s length between the front of the shoe and the end of the longest toe. Shoes should also:
- Offer support around the arch and heel
- Be suitable for the activity the person is doing
- Have enough space at the front to accommodate the natural shape of the toes, both in width and depth. “Tapered, shallow and narrow fronted shoes are best avoided,” says Dr Branthwaite.
For general foot health, she advises washing the feet in warm, soapy water daily and drying between toes; changing socks daily – or more often if socks get damp; applying moisturising cream daily, taking care to avoid the area between the toes, and checking the feet regularly for changes. Anyone reporting any changes (e.g. discolouration, swelling, pain, skin changes or changes in sensation or temperature that last longer than a few days) should be referred to the pharmacist.
A guide to foot health
When it comes to conditions that can affect the feet, prevention is first prize.
It can be tricky for customers to spend time off their feet as people generally need to get from A to B, which makes the rest needed for recovery tricky to achieve. This quick guide to footcare will help you when advising customers on prevention and treatment options for some common problems.
Dry skin
One of the areas customers may overlook when it comes to footcare is their skin, which plays an important role in protecting the feet from injury, allowing comfortable movement and regulating temperature. “The skin on the sole of the foot differs from the rest of the body as it does not have sebaceous glands. This makes it naturally drier,” says Dr Ivan Bristow of the Royal College of Podiatry’s dermatology in podiatry specialist advisory group. “The skin is also thicker to help accommodate the forces and activities our feet are designed to do. This means the skin on your feet needs a bit more TLC than you might think.”
Customers dealing with dry skin or cracked heels should use a moisturising cream. “Creams which contain five to 10 per cent urea can help to both prevent and treat dry and cracked skin. Using these liberally overnight under socks can improve their effectiveness,” says Dr Bristow.
“There are other underlying reasons that skin on the feet can become dry and cracked,” he adds. “Wearing backless shoes and sandals can increase the incidence of heel fissures. Medical conditions such as diabetes and obesity and drugs such as statins can all have an effect, as can some other medications and treatments. Dermatological conditions such as eczema and psoriasis can present on the feet and can be easily confused with dry skin.”
Dry skin should start to improve within a couple of weeks of using a urea cream daily. If this is not the case, the customer should be referred to the pharmacist or advised to seek professional advice from a Health & Care Professions Council (HCPC) registered podiatrist.
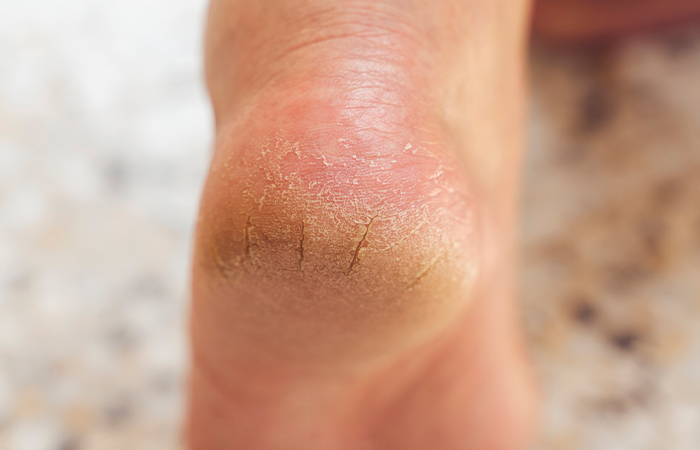
consistent moisturising to get rid of.
Fungal nail infection
Knowing the signs of an infected toenail can help customers to avoid serious discomfort.
“Fungal infections (onychomycosis) affect up to eight per cent of the population but are much more frequent in older adults. They usually start in the skin as athlete’s foot and then spread to cause thickening and discolouration of one or many toenails,” says Dr Bristow. Fungal infections can also be caused by an ingrown toenail. Symptoms include:
- White, chalky patches on the nail
- Yellow, brown or orange discoloration under the nail
- A flaky, discoloured nail
- Thickened and discoloured nails that are not uniform in colour.
It is not unusual for toenails to change in thickness and colour as people age, which means many customers may not realise when an infection has occurred, so they may advance and be harder to treat.
“Where the infection is present in only the middle to the tip of the nail, over-the-counter preparations containing 5% amorolfine may be effective, used twice a week, but can take up to 18 months to work,” says Dr Bristow.
“There are many other products available for discoloured and fungal nails. However, these are not medicines and are less likely to resolve the fungal nail infection. Often, they will have a ‘bleaching’ or acidifying effect, providing a temporary improvement.”
Dr Bristow cautions that any customers with an infection that has spread to the lunula (half-moon) of the nail should be referred to the pharmacist or an HCPC registered podiatrist.
Ingrown toenails
Customers may complain of toe pain caused by an ingrown toenail, which is when the nail grows into the toe. The toe may be red, painful and swollen. The NHS recommends soaking the affected foot in warm, salty water to help soften the skin and reduce the chances of infection, and then to keep the foot dry for the rest of the day. Paracetamol or ibuprofen can be taken for pain. It is very important that customers do not cut the toenail, or pick at it. Wearing wide, comfortable shoes that do not squish the toe is also important. Customers should also be advised not cut their toenails too short, and to cut straight across the nail, rather than down the edges.
Anyone with a troublesome ingrown toenail should be referred to the pharmacist in case antibiotics or further referral are required. In some cases, a podiatrist may cut away part of the nail or remove the whole nail.

