Keeping women well
In Conditions
Follow this topic
Bookmark
Record learning outcomes
There are many common women’s health problems that can benefit from fast intervention, and pharmacy teams can help
Covid-19 is having a huge impact on women’s health and wellbeing, even among those who have not caught the virus themselves. A recent study by researchers at UCL claims women have found the pandemic more psychologically challenging than men, reporting higher levels of depression, anxiety and loneliness, and lower levels of life satisfaction and happiness.

Add to this the additional challenge of reduced access to many regular healthcare services such as GP surgeries, cancer screenings and others because of social-distancing measures, staff sickness or self-isolation, and it’s easy to see why so many women’s health issues are being unaddressed, undetected and left to deteriorate.
Thankfully, community pharmacies have remained open throughout the pandemic, with teams providing vital care, advice, support and signposting on the most common women’s health problems. Women are notorious for putting their own needs last, so encouraging them to address health problems quickly can be vital.
Offering this timely and supportive advice can make a huge difference to the outcomes for common women’s health issues, particularly during the current challenging times.
Thrush
Thrush is a yeast infection caused by an overgrowth of the Candida fungus, causing intense itching and soreness. It is often a result of taking antibiotics, as these kill other harmless bacteria allowing the fungus to thrive, but vaginal thrush can also be due to hormonal changes in pregnancy or menstruation, poorly controlled diabetes, scented bath products and wearing tight clothing.
Treatments usually contain an antifungal agent such as clotrimazole, econazole, miconazole or nystatin, which aim to reduce the level of Candida infection in the body. These are available as anti-fungal vaginal pessaries or intravaginal creams. Topical creams can also help to soothe itching, and oral tablets containing fluconazole, ketoconazole or itraconazole may be used.
Bacterial vaginosis
Bacterial vaginosis (BV) is actually the most common vaginal infection, but is often confused with thrush. BV is caused by a change in pH levels and symptoms include vaginal odour and a thin, white-grey discharge, whereas thrush symptoms are itching and a thick, white and odourless discharge.
Although BV is not usually serious, the NHS advises that it is treated with antibiotics, and stresses the importance of pregnant women seeking treatment as there’s a small chance it can cause complications with pregnancy.
Bacterial vaginosis (BV) is actually the most common vaginal infection, but is often confused with thrush
Cystitis
Cystitis is a urinary tract infection (UTI) caused either by a bacterium such as E. coli, or sometimes by non-bacterial agents, which results in inflammation of the bladder. Common symptoms include pain and frequency, urgency and difficulty in passing urine.
If not treated, a serious kidney infection may develop, so customers should see their GP if they have suffered for more than 24 hours, or be referred to a pharmacy-based UTI service, where appropriate and available. Pharmacy teams should also be alert to customers of any age who appear to be suffering from repeated or recurring UTIs that are not being resolved by treatment with antibiotics, and encourage them to go back to their GP to discuss other options or to ask for a referral to a specialist for further investigation.
Sensible steps to prevent cystitis include drinking plenty of fluid, passing water every three to four hours and avoiding the use of highly perfumed toiletries.
Bladder weakness
Urinary incontinence – known as bladder weakness or sometimes ‘leaking’ – can affect women of all ages, causing distress, embarrassment and inconvenience.
Continence charity the Bladder and Bowel Foundation (BBF) describes three main types of urinary incontinence:
- Overactive bladder (OAB) – a chronic condition defined as urgency, with or without urge incontinence, usually with frequency (needing to go to the toilet more than eight times a day) and nocturia (getting up to go to the toilet during the night)
- Stress urinary incontinence (SUI) – characterised by urine leaking in dribbles or spurts when coughing, sneezing, laughing, lifting and so on. This is usually due to weakness of the bladder or pelvic floor muscles, especially after childbirth or during menopause
- Mixed incontinence – a combination of OAB and SUI symptoms.
Most require investigation by a GP to determine the cause and help with management, but because women can be embarrassed to talk about incontinence, pharmacy staff should be alert to repeat purchases of incontinence products as a signal to start conversations and refer where appropriate.
Catching cancer early
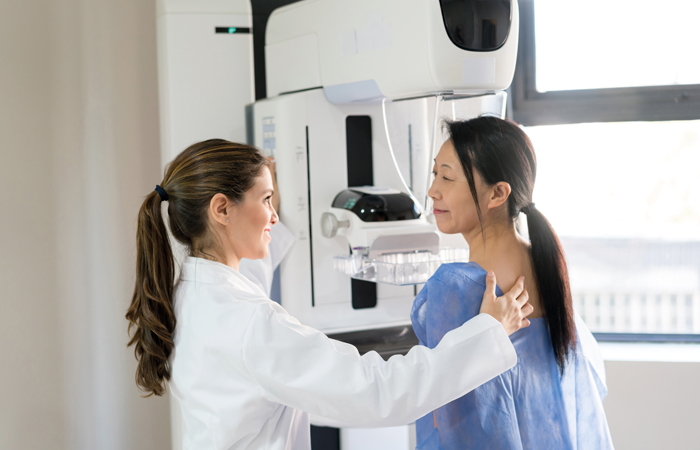
Cervical cancer remains the most common cancer in women under 35, claiming some 850 lives a year. Therefore, it is crucial that women continue to take up their invitation to cervical screening when they receive it, as well as telling their GP about any potential symptoms – such as bleeding between periods – that could indicate abnormal changes of the cervix before it could develop into cancer.
Eligible people in England are invited for cervical screening – also known as a smear test – every three years starting from up to six months before their 25th birthday to the age of 49, and every five years from ages 50-64. But with delays in screening caused by the Covid-19 pandemic, customers may be coming to pharmacy teams with their concerns, or reporting that they will put off going to screening appointments because of social-distancing worries.
It is vital that all staff, even if they have never had a cervical screen themselves, can talk confidently on the subject in order to reassure customers that screening is available, important and safe, and encourage them to take it up.
Pharmacy staff have a similar role to play when it comes to supporting customers with advice about being ‘breast aware’. Breast cancer is the most common cancer in the UK, but as breast changes are not usually accompanied by other physical symptoms, even if someone feels well it is still important that they see their GP and get any concerns checked out.
As with most cancers, the earlier breast cancer is diagnosed and treated, the better the chance of successful treatment. Making sure that customers know to check their breasts regularly for lumps and other changes can improve their chances of finding breast cancer at an early stage. Signs and symptoms to look out for include:
• A lump in the breast
• A change in the size or shape of the breast
• Puckering, dimpling of the skin or thickening of the breast tissue, like the skin of an orange
• A nipple that has inverted or changed position or shape
• Redness or a rash on the skin or around the nipple
• Discharge from the nipple
• Pain in the breast or armpit all or almost all of the time
• Swelling in the armpit or around the collarbone.
The breast cancer screening programme triggers an invite from the woman’s GP surgery every three years from the age of 50 until the age of 70, so pharmacy teams should remind women to make sure their GP has their correct contact details.
Period pain and heavy bleeding
Period pains (dysmenorrhoea) are caused by muscular contractions of the uterus as the body expels the lining of the womb during a period.
Pharmacy staff can recommend OTC pain relief options such as ibuprofen, as well as self-heating patches, microwaveable heat packs or hot water bottles to gently warm the areas of the body that are in pain. If that’s not working, customers can see their GPs for stronger prescription pain relief.
Heavy periods are also common and can have a debilitating effect on a woman’s everyday life. They do not always have an underlying cause, but as they can cause anaemia, or result from problems such as fibroids or endometriosis – which can go on to cause fertility problems – it’s important that women are encouraged to get their symptoms checked out.

Fertility problems
Many women imagine they can get pregnant when they want, but it’s not always that simple. Fertility rates drop naturally after the age of 30 and lifestyle factors such as poor nutrition, stress and anxiety are also significant.
According to the National Diet and Nutrition Survey (NDNS) rolling programme, which charts nutrient intake in the population on an ongoing basis, women of childbearing age over the last 20 years have shown a downturn in the intake of micronutrients such as folate, which are key to successful conception, pregnancy and birth. And figures from a new report from the makers of the Alive! range of multivitamins, entitled ‘Nutrient starved’, says the number of women failing to achieve even the lower reference nutrient intake (LRNI) for folate has risen from three per cent to six per cent.
“These are worrying figures”, says Dr David Edwards, GP and an advisor to Alive!. “Folate is crucial pre- and post-conception for a healthy pregnancy, with low intakes during pregnancy increasing the risk of neural tube defects (NTDs) such as spina bifida in the unborn baby.”
Eating a healthy, varied diet in pregnancy will help expectant mothers get most of the vitamins and minerals they need, but Government advice is to take 400 micrograms (mcg) of folic acid each day from before conception until 12 weeks pregnant. The Department of Health and Social Care also advises all adults, including pregnant and breastfeeding women, to take 10mcg of vitamin D a day, and should consider taking a supplement containing this amount to keep bones, teeth and muscles healthy.
Women are notorious for putting their own needs last, so encouraging them to address health problems quickly can be vital
Emergency contraception
Community pharmacy is often the first port of call for emergency hormonal contraception (EHC), and while these inquiries will require pharmacist intervention, the whole pharmacy team should know how to handle them, as counter staff are often the first people the customer will speak to.
GPhC guidance requires all pharmacy professionals to be sensitive in the way they communicate with people asking about EHC and “not imply or express disapproval or judgement”. With this in mind, each member of the team should ensure they are trained to treat patients with respect and sensitivity.

Menopause and hot flushes
Menopause is defined as the point in a woman’s life when she has not had a period for a whole year. In the months and years leading up to this, women can experience a range of symptoms that vary tremendously. Some women only experience symptoms for a few months, whereas others can suffer for years, even after their last period.
The most common symptoms are:
- Hot flushes – 75 per cent of menopausal women have these
- Night sweats
- Mood swings
- Tiredness and insomnia
- Reduced or absent libido (sex drive)
- Vaginal dryness
- Poor concentration and ‘brain fog’.
Hot flushes can be eased by wearing light clothing in layers, drinking plenty of water and limiting hot drinks, alcohol and spicy foods. Pharmacist Norma Goldman, founder of The Menopause Exchange, says: “There are also non-hormonal prescribed treatments for menopausal hot flushes and night sweats which can help.”
It can be common for doctors to miss the symptoms of menopause, and many women are prescribed antidepressants for menopausal symptoms such as anxiety, depression and insomnia, when in fact hormone replacement therapy (HRT) would be more appropriate if menopause is the cause. Some women may choose to try alternative or complementary products instead, but Norma stresses that these “may not be suitable for women who have a history of breast cancer, other medical conditions or are taking medication or over-the-counter medicines”.
An unexpected downside of obesity
Being obese can have dire health consequences such as an increased risk of developing many potentially serious health conditions including type 2 diabetes, coronary heart disease and stroke. The Covid-19 pandemic has also shown that people living with severe obesity are more vulnerable to the virus and experience higher death rates. But there are other, more unexpected, downsides to being obese too.
Research from the Institute for Employment Studies (IES) claims that women who are obese are paid up to 13 per cent less than those who are not. They also experience reduced wellbeing at work and increased stress. The IES’s new report entitled ‘Obesity Stigma at Work: Improving Inclusion and Productivity’, found that weight-based stigma is rife in employment, as a result of employers not understanding the causes of obesity or holding the stereotypical belief that those living with obesity are lazy, less conscientious and incompetent.
Avideh Nazeri, director of clinical, medical and regulatory affairs at Novo Nordisk UK, which sponsored the report, says: “Obesity is a complex, chronic condition influenced by a range of factors including genetics, physiology and environment. Better understanding of the science of weight gain and loss is urgently needed to improve employment outcomes for people with obesity, and could play a key role in unlocking the full potential of the workforce as we recover from the economic impact of Covid-19.”
