First responder
In Conditions
Follow this topic
Bookmark
Record learning outcomes
With quick action crucial for dealing with many accidents and injuries, knowing what tips and advice to pass on to customers could mean the difference between life and death
Thousands of people die or are seriously injured in incidents every year in the UK. Yet, according to the NHS, many of these could have been prevented if first aid was given before the emergency services arrived. First aid is life-affirming, too. As the British Red Cross says: “If someone is injured or becomes suddenly ill at work, there is no greater act of human kindness than a person with the skills and confidence to step in and provide first aid support.”
If pharmacy teams are confronted by sudden injury or illness in the pharmacy, it is important to know what to do. Is there a dedicated first aider within the team? Does the pharmacy have a standard operating procedure (SOP) in place, and is everyone confident in their knowledge of it? If not, asking a colleague, pharmacist or manager for help is important.
If members of the pharmacy team haven’t been on a firstaid training course, it could be added to a to-do list for when lockdown relaxation allows it. Both St John’s Ambulance and the British Red Cross are hoping to resume their training courses from 4 July.
Of course, first aid isn’t always a matter of life or death. More often, it will involve giving care in a less serious situation. However, it is always important that customers know how to administer care safely, and pharmacy teams can help by recommending appropriate products and advising on their correct use for common conditions.
In the meantime, you could:
Download an app: The British Red Cross has produced First Aid and Baby and Child First Aid apps, while St John Ambulance offers apps on First Aid Advice and First Aid for Cyclists. All are available free from Google Play or the Apple Store
Test your knowledge: The British Red Cross has produced a handy PDF with tips on basic first aid techniques as well as a self-test quiz
Download resources: There are lots of resources available to download from the St John Ambulance website, including posters to display in the pharmacy or in the staff room and two free pocket-sized guides, Essential Baby First Aid and This Guide Saves Lives.
Cuts and grazes
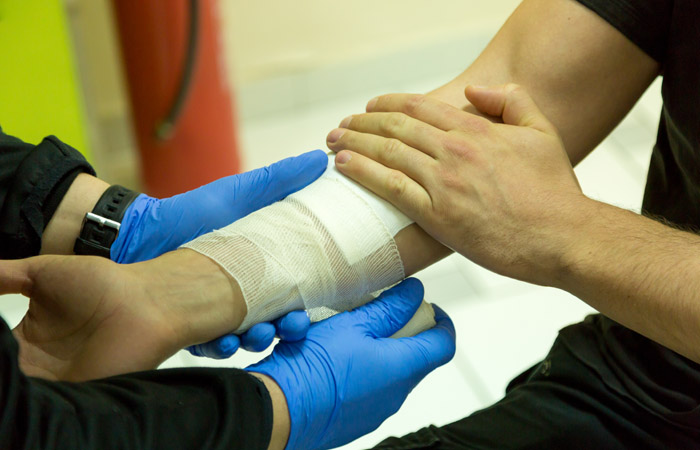
The first step in treating cuts or grazes is to stop the bleeding. This should be done by applying pressure to the area for several minutes. Ideally, a clean, absorbent bandage would be used, but any clean, non-fluffy material or even the person’s own hand will do.
When the bleeding has stopped, the wound should be cleaned under running water and patted dry with clean material. It can then be covered with a dressing or plaster to help prevent infection. The dressing should be changed as necessary and removed once the wound has closed itself. If pain relief is required after the injury, paracetamol or ibuprofen can be taken, as appropriate for the person.
Customers should call NHS 111 if:
- The wound looks like it is infected
- The wound was caused by an animal or human bite
- They feel generally unwell or develop a fever.
- They should go to A&E if:
- The bleeding won’t stop – note that pressure should be maintained on the wound at all times
- Bleeding is from an artery – the blood will pump in time with the heartbeat and be bright red and hard to control
- There is persistent loss of sensation or movement
- The wound is very large
- There is a large cut on the face, as hospital treatment may help to prevent scarring
- There is something embedded in the wound after cleaning
- A cut on the palm of the hand looks infected, as infections here can spread quickly.
Burns and scalds
Burns and scalds both damage the skin by heat. The difference between them is that a burn is caused by dry heat (e.g. from an oven or a fire), while a scald is caused by something wet, such as hot water or steam. Strangely, the level of pain a person feels after such an injury doesn’t always indicate how serious it is. First aid for burns involves the following steps:
- Immediately remove the heat source
- Take heat out of the injured area by running cool water over it for at least 10 minutes. Ice, iced water, creams or greasy substance like butter should not be used, but if there is no water, any cool liquid can be used – juice, milk or even beer – until there is access to water
- Remove clothing or jewellery from the injured area – but do not remove if it is stuck to the skin
- Cover the affected area loosely with cling film or a clean plastic bag
- If appropriate, take painkillers such as ibuprofen or paracetamol
- If the face or eyes are injured, the person should sit up if possible, rather than lying down, as this helps to reduce swelling.
Minor burns should heal on their own if they are kept clean and the person resists bursting any blisters that have appeared. However, a visit to A&E is required if the injury:
- Was caused by electricity or a chemical
- Is large or deep
- Causes white or charred skin of any size
- Is on the face, hands, arms, feet, legs or genitals and has caused blisters.
If the person has breathed in smoke or fumes, they should also be advised to seek medical attention.
A burn is caused by dry heat, while a scald is caused by something wet
First aid for minds
The events of this year have placed particular stress on most people’s mental wellbeing. And although there is no visible injury, first aid still applies when stress is becoming harmful to health.
The most important first step is to talk to someone. Visit Help for employees on stress at work for more information on how to do this, as well as the signs and symptoms to look out for, and links to useful resources.
Employers have a legal duty to protect employees from stress at work by doing a risk assessment and acting on it. So, if something at work is bothering you, speak to your manager. If the problem is being caused by your manager, find out what policies are in place to deal with this. If there are none, you talk to your HR department, if you have one, or your GP if you don’t. The HSE website also has valuable advice about this.
Insect bites and stings
Insect bites and stings can cause a red, swollen lump on the skin that might be painful or itchy, and in some people they may trigger an allergic reaction (see below).
If there is no allergic reaction, symptoms usually pass within a few hours or days, bearing in mind the following first aid steps:
- Remove any insect parts still in the skin
- Wash the area with soap and water
- Apply a cold compress or ice pack for at least 10 minutes
- Raise the affected area if possible to minimise swelling
- Avoid scratching the area (to prevent infection).
Painkillers such as paracetamol or ibuprofen can help with pain, as appropriate. Customers should call NHS 111 if they are worried about a bite or sting, or:
- If symptoms don’t start to improve within a few days, or get worse
- The mouth, throat or eyes are affected
- A large area (10cm or more) around the site becomes red and swollen
- The area looks infected
- They develop signs of an infection, such as a fever, swollen glands or other flu-like symptoms.
Allergic reactions
Most allergic reactions are mild enough to cause nothing more than irritating symptoms like itchiness, a runny or blocked nose, dry skin, a rash or an upset stomach. In these cases, over-the-counter treatments like antihistamines or emollients should suffice. Refer to the pharmacist for advice on an individual basis and to check whether a GP referral is necessary.
Some reactions, however, are more serious and require urgent medical attention. If not treated fast, an allergic reaction called anaphylactic shock can be fatal.
Signs of anaphylactic shock include:
- Feeling lightheaded, faint, confused or anxious
- Breathing difficulties, such as fast, shallow breathing
- Wheezing
- A fast heartbeat
- Clammy skin
- Swelling of the tongue and throat
- Loss of consciousness.
There may also be other allergy symptoms, such as an itchy, raised rash (hives) or stomach pain.
If someone is having a severe allergic reaction, they may have medication, such as a pre-filled injection device containing adrenaline, with them. If they do, help them to use it or follow the instructions yourself. Then call 999.
If something visible (e.g. an insect sting) has triggered the reaction, remove it if possible. Help the person to get comfortable and monitor their breathing and responsiveness while you wait for paramedics to arrive. Repeated doses of adrenaline can be given at five-minute intervals if there is no improvement or the symptoms return.
Stroke of genius
The NHS is starting to use artificial intelligence (AI) to help doctors treat people who have had a stroke.
The chances of surviving this life-threatening condition are higher if 999 is called as soon as a stroke is suspected. Unfortunately, fears about Covid-19 are stopping people from seeking treatment. The NHS is keen to let people know, however, that services have been restructured to reduce the risk of patients being exposed to, or passing on, the infection. Some hospitals are even using a new AI tool that allows staff to share patient scans with stroke physicians quickly and remotely, rather than having to see them in person.
The FAST acronym can help to identify a possible stroke:
• Face – has their face fallen on one side? Can they smile?
• Arms – can they raise both arms and keep them there?
• Speech – is their speech slurred?
• Time to call 999.
