Pharmacy flu fighters
In Conditions
Follow this topic
Bookmark
Record learning outcomes
Seasonal flu jabs have been around since the 1960s but have only taken off in pharmacies over the last few years. What do pharmacy teams need to know for the 2018/19 season?
In pharmacy, autumn is the season where it all starts to ramp up. Everyone is back into the old routine – staff, patients and customers – and life is busy but steady on both sides of the counter; a sense of harmony before the chaos that is the run up to Christmas. The last few years have seen flu jabs added to the hive of activity, particularly in England and Wales where pharmacies have been brought under the umbrella of the NHS service, but also elsewhere with many administering vaccines on a private basis.
A recent report from the International Longevity Centre shows just how important all this effort is. In the publication, the think tank – which looks at ways in which government and society can tackle the challenge of an ageing population – states that, in England, the vaccination programme prevents between 180,000 and 626,000 cases of flu and anything from 5,600 to 8,800 deaths each year. While the cost of the initiative is high, not just because of the price of vaccines but also in terms of the resources – human and otherwise – that go into getting people inoculated, the organisation indicates that it is worth it. However, it isn’t perfect and the report highlights two major issues: vaccine effectiveness and uptake.
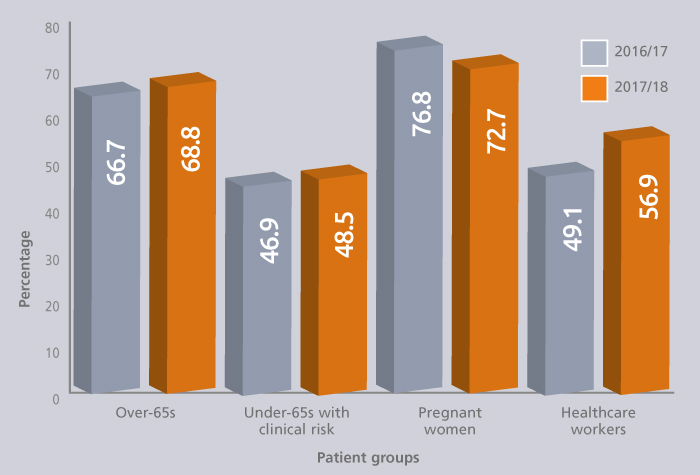
Coverage has been on an upwards trajectory year on year. Figures from GP surgeries in England show that 72.6 per cent of patients aged 65 years and over received the vaccine in 2017/18, compared to 70.5 per cent the previous year. The same trend is true of pregnant women (47.2 compared to 44.9 per cent), patients in clinical risk groups (48.9 compared to 48.6 per cent), three-year-olds (44.2 compared to 41.5 per cent) and two-year-olds (42.8 per cent compared to 44.9 per cent). More frontline healthcare workers received the jab last year too, at 68.7 per cent compared to 63.2 per cent, and in schools – which last year saw invitations extended to all children from Reception to Year 4 inclusive – the uptake was just under 60 per cent.
England
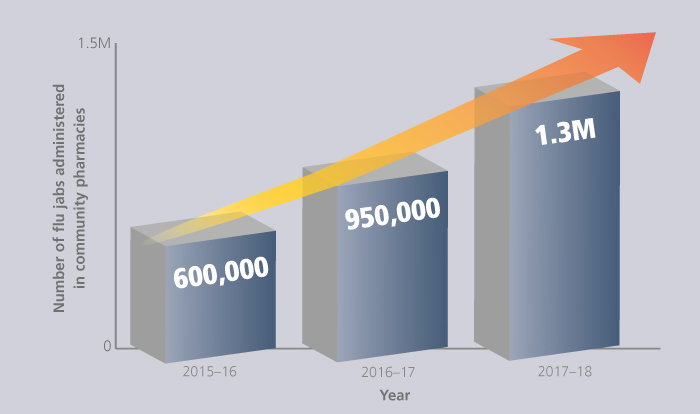
Vaccines administered
Challenges and solutions
While pharmacies becoming part of the seasonal flu prevention effort was viewed as a logical step within the sector, there has been dissent from some quarters outside the profession. Shilpa Shah, LloydsPharmacy area manager for North London, says: “In some places, GP practices have viewed it as a threat to their income – in one instance, a surgery put a notice on its door telling patients that the practice would lose money if they went elsewhere for their flu vaccination and this could lead to the surgery closing.” Ade Williams, pharmacy manager at Bedminster Pharmacy in Bristol, agrees: “Pharmacies can be viewed as being in competition with GPs – it’s a big flaw in the service, and a missed opportunity to improve collaboration between the two.”
Shilpa goes on to say: “The places where it works best are those where the pharmacy and GP practice have worked together. In one branch, the GP practice had no capacity so turned over its list to the pharmacy and signposted all patients who could have it done outside the surgery. The best thing pharmacies can do is explain to local GPs that they are there to help, and can catch individuals who wouldn’t necessarily be picked up otherwise. For example, the man with diabetes who is so stable that he barely goes into his surgery, instead ordering his prescriptions online or over the phone, but still falls into the clinical ‘at risk’ category; and the woman who pops in to buy some make-up after she’s done the school run but before she goes to look after her elderly parents.”
Ade’s thoughts run along the same lines: “Carers are a low priority for surgeries, but pharmacy has a real opportunity to identify them, tell them about the flu jab, and do it there and then. For this to happen, you have to have someone trained to provide the service during all the pharmacy’s opening hours. It doesn’t just provide consistency, it makes financial sense too; once you’ve added up the time it takes to manage an appointments system and remind people to come in, you may as well have got all your pharmacists to do the training to administer the injections.” He adds a note of warning, however: “Pharmacy needs to make sure they show patients professional courtesy by not putting on them to tell the GP surgery that they have had the jab elsewhere – we can and should do that for them.”
Ade continues: “We also contact the midwife team to let them know that we are providing the service as commissioned by NHS England, and highlight that we can vaccinate for longer than GP surgeries – up until the end of March. We get a lot of pregnant women from ethnic minorities in this way because they find it easier to communicate with us what they have come in for instead of trying to explain at the GP’s – they can simply say they have come in for an injection and we know what they mean as it’s the only one we do.”
Wales
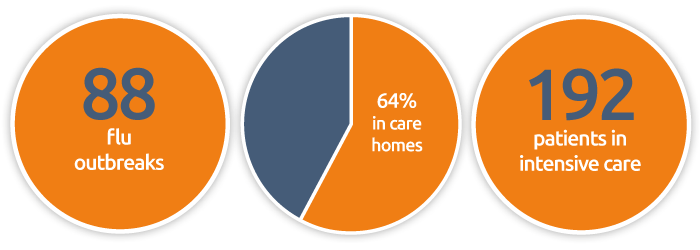
Flu outbreaks reported
Vaccine uptake
2018/19
This winter sees pharmacies continuing in their role as part of the NHS seasonal flu vaccination scheme, with an emphasis on targeting care home staff. All primary school children are included in the 2018-19 effort.
Harnessing staff power
While pharmacists are the ones doing the jabs, staff members have a vital role to play. Shilpa says: “They are the ones who come into contact with customers first, so it’s about making every contact count.” Bedminster Pharmacy’s healthy living champion June Cambridge-Rose says that approach works whether the individual has come in for a prescription, an OTC product, or for any other reason: “We spot people who are eligible for the free NHS flu jabs through their prescriptions when we are dispensing, or when we are chatting to them as they wait for their medicines or pay for items at the till.”
Pharmacy team members can also raise awareness of flu vaccination by putting up posters and displays, using bag stuffers and stickers, and drawing attention to leaflets on the topic; these should be provided in a variety of languages as appropriate to the customer base. Ade says that delivery driver Shirley Jamieson is invaluable at reaching individuals who otherwise wouldn’t find out, yet are among the most vulnerable, stating: “Nearly a third of the vaccinations that we do are for people who have come in because Shirley has seen them on her rounds.”
The benefits of flu jabs extend beyond those who have been vaccinated: herd immunity – protection for people who haven’t had the injection because circulating virus levels are lower; this is particularly important for individuals who can’t be immunised, perhaps because of an illness or an allergy to one of the vaccine ingredients – and greater understanding that pharmacy is about more than just dispensing and selling medicines. It is also about demonstrating how pharmacy is a key part of the NHS and healthcare in general, says Shilpa: “At the end of the day, we all just want to do the best for our patients and the public, and this is another way in which we can do it.”
Northern Ireland
Flu outbreaks reported
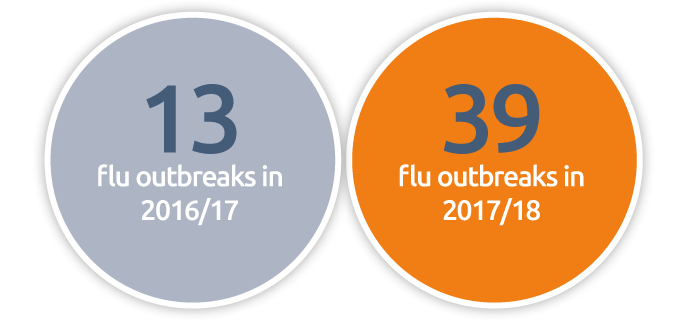
Vaccine uptake
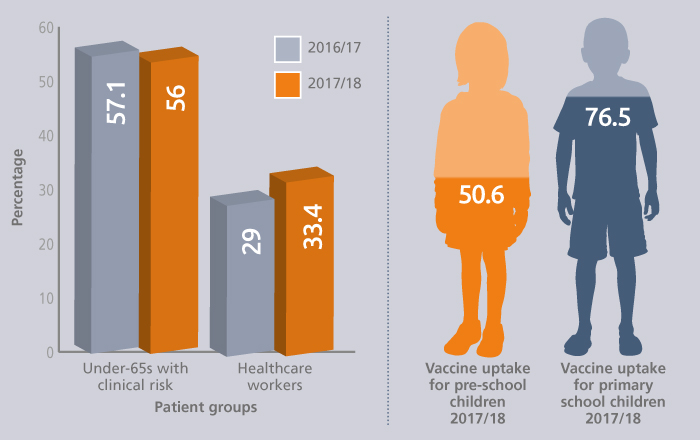
2018/19
This winter, Northern Ireland will adopt the same approach as England, but with GP practices and schools administering vaccines from the beginning of October until the end of March.
What is in the vaccine, and why?
Each year, the World Health Organization analyses surveillance data from around the world to decide which flu strains should be included in the annual vaccine. This year’s jab for the Northern Hemisphere contains two strains each of influenza A (Michigan and Singapore) and B (Colorado and Phuket), making four in total: this is known as a quadrivalent influenza vaccine (QIV), e.g. Fluarix Tetra, and is generally used for adults considered at increased risk of flu and its complications. The intranasal version, mainly used for children, is also quadrivalent, but is referred to in official documentation as the live attenuated influenza vaccine (LAIV). The brand name of this product is Fluenz Tetra. There is also a jab that doesn’t contain the Phuket B strain, known as a trivalent influenza vaccine (TIV), e.g. Influvac. Some also contain an adjuvant, a substance that boosts the immune response, and are referred to as adjuvanted trivalent influenza vaccines (aTIV), e.g. Fluad. Trivalent vaccines tend to be used in the over-65s, who are less likely to catch the additional influenza B strain that is in the quadrivalent product.
The effectiveness of the seasonal flu vaccination varies year to year. This is because the virus mutates, and these changes are difficult to predict. According to Public Health England, last year’s jab was 15 per cent effective overall. This sounds poor, but importantly efficacy was higher in one of the most vulnerable groups – under-18s – at nearly 27 per cent, with over 90 per cent protection conferred against the H1N1 A strain (which caused the swine flu pandemic of 2009) and over 60 per cent against B strains which tend to be more common in children.
Vaccine supplies can and do vary, and this year is expected to be no different, particularly because of the different forms of vaccines that are recommended for different groups of patients. The advice is to start vaccinating each group as the appropriate vaccine becomes available, ideally before December. However, it is worth remembering that it is OK to continue to offer jabs to eligible patients at any point in the season; this is particularly relevant if the flu season is later than expected and for patients who move into the at-risk groups such as newly pregnant women.
Scotland
Vaccine uptake
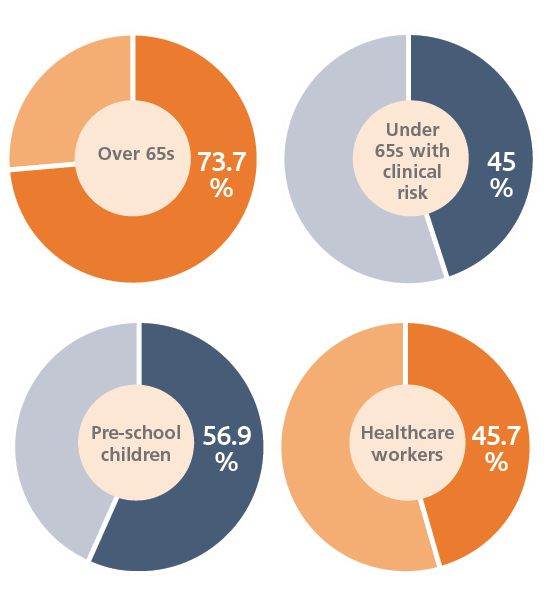
Hitting targets
The flu vaccination scheme in Scotland is delivered through GP practices. Health officials in Scotland have met the World Health Organization target for 75 per cent of over 65s to be vaccinated against seasonal flu five out of the last eight years.
Further information
- The ILC report
- England’s seasonal flu programme
- PSNC’s information on England’s pharmacy flu jab service.
Nearly 9,000 pharmacies in England delivered over 1.3 million NHS flu jabs last season
