Save Our Skin
In Conditions
Follow this topic
Bookmark
Record learning outcomes
Coming in from the wind and rain to a centrally heated house may feel blissful, but it can also wreak havoc on the skin. How can pharmacy teams answer customers' distress calls?

Winter is a challenging time for skin, when biting winds, freezing temperatures, hot central heating and a drier atmosphere all conspire to leave it dry, flaky, irritated and dull. But while we can't do much about the weather, there's plenty your customers can do to adapt their skincare routines to help prevent and control their skin worries and woes. Here, we look at some of the common winter skin scenarios that pharmacy teams are likely to encounter, and the advice that can be recommended to help solve them.
Scenario 1: chilblains
Samantha Seabourne, a slim and sprightly 65-year-old, calls in to the pharmacy. €You know I walk a lot, don't you?€ she says.
€Well, about a week or so ago I got caught in the rain and my feet got soaked because I wasn't wearing the right shoes. I took them off as soon as I got home and sat with a hot water bottle on my feet because they were freezing, but then I got some very itchy and sore spots. Take a look.€
Samantha slips her boot and sock off one foot and you see that an area of her heel and on her little toe is purple-red, slightly swollen and blistered, and she tells you that her other foot is almost identical.
Solution
 Samantha has chilblains on her feet as a result of the blood vessels near the surface of the skin becoming narrowed because of the cold and then suddenly wider again upon exposure to heat. This causes blood to leak into the surrounding tissue. The extremities of the body, such as the toes, fingers, ears and nose, are more likely to be affected by the condition, which is also known as perniosis and is more common in children, older people and women.
Samantha has chilblains on her feet as a result of the blood vessels near the surface of the skin becoming narrowed because of the cold and then suddenly wider again upon exposure to heat. This causes blood to leak into the surrounding tissue. The extremities of the body, such as the toes, fingers, ears and nose, are more likely to be affected by the condition, which is also known as perniosis and is more common in children, older people and women.
Other factors that can increase the risk of chilblains include poor circulation (e.g. because of a condition called Raynaud's syndrome), low body mass index and medication (e.g. beta blockers), which can cause cold extremities as a side effect.
Usually, chilblains get better on their own, taking around one to three weeks to do so. There is little that can be done to hasten the process, although some people feel that overthe- counter products that contain rubefacients can provide relief. It is important that Samantha doesn't scratch or rub her chilblains, as this will increase the risk of complications such as infection, ulceration and permanent scarring. If they have not got better in a few weeks, she should seek further healthcare advice.
There are also some measures that Samantha can take to reduce the chance of her experiencing chilblains in the future. For example, making sure she wears warm, well-fitting and waterproof footwear on her regular walks, which will boost her circulation and have a preventative effect. For a similar reason, she should quit smoking if she is currently a smoker.
In the future, if Samantha does feel that her feet have got too cold and that the chilblains may recur, she should warm them up gradually by putting on warm, dry socks rather than using a hot water bottle for a quick result.
Scenario 2: atopic eczema
Stay-at-home mum Charlotte Young is waiting for her son's prescription to be dispensed.
€I hate this time of year,€ she grumbles. €All the school runs and taking the kids to and from activities means I am constantly moving from inside to outside and back again, and my skin €“ which is dry at the best of times €“ just seems to give up! The amount I spend on creams for my face and body is ridiculous, but I figure that it's cheaper than moving to a warmer country, right?€
Solution
It sounds as though Charlotte may have atopic eczema, which can be triggered by the cold and damp weather that defines the great British winter. Most people with atopic eczema have very dry skin because it is unable to retain much moisture. This then means it doesn't take much to prompt an exacerbation, during which the skin becomes red and incredibly itchy.
In children, skin folds such as inside the elbows and the backs of the knees are most commonly affected, but in adults it is often the face that bears the brunt of the condition. Having said that, eczema can affect any part of the body. Rather than buying more cosmetic moisturisers, Charlotte would be better off stocking up on some emollient products.
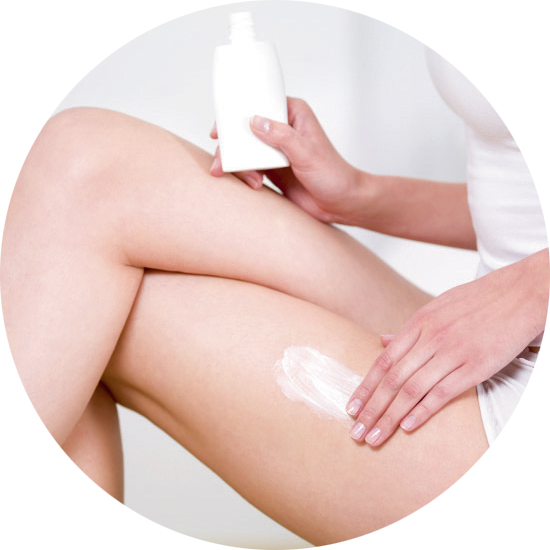 These will more effectively reduce water loss from the skin and protect it by providing a barrier. She may wish to take a multi-pronged approach to the problem, using one product as a soap substitute when washing, a cream or lotion on her face, and a greasier ointment on her body or on very dry patches of skin.
These will more effectively reduce water loss from the skin and protect it by providing a barrier. She may wish to take a multi-pronged approach to the problem, using one product as a soap substitute when washing, a cream or lotion on her face, and a greasier ointment on her body or on very dry patches of skin.
After bathing, a generous quantity of the emollient of choice should be smoothed onto the skin in the direction of hair growth, and then reapplied frequently €“ certainly at least once more during the day. This should be done all the time, even if the skin seems fine.
Given that changes in temperature seem to cause Charlotte's skin to worsen, she should try to keep her home environment cool, particularly her bedroom. She should keep her nails short and try to avoid scratching in order to lessen the chance of infection, instead rubbing the skin if the itchiness is overwhelming. If Charlotte experiences a flare up, she should return to the pharmacy for advice on topical corticosteroid and antihistamine use, although severe symptoms may warrant a visit to her GP.
Scenario 3: rosacea
€Please can you help me,€ pleads Claudia Craig, a regular customer who you estimate to be in her early 40s. €Every year at around this time, I get hot flushes, and it looks really unprofessional when I turn up to represent someone in court with a bright red face. I try my best with make-up, but it's tricky because my skin gets quite spotty as well, and I've noticed that some of the little blood vessels in my skin have become visible. I don't drink, but I swear my colleagues think I'm a winter alcoholic!€
Solution
 Claudia needs to visit her GP as her symptoms point towards rosacea, a chronic relapsing condition of the facial skin that is characterised by repeated episodes of flushing, persistent reddened skin and spots. Some sufferers report sensations of burning and stinging in the skin, and it isn't uncommon to experience eye symptoms. Fair-skinned women aged between 30 and 50 years are the most commonly affected, and symptoms can be triggered by extremes of weather, stressful situations, strenuous exercise, spicy food, alcohol and hot drinks.
Claudia needs to visit her GP as her symptoms point towards rosacea, a chronic relapsing condition of the facial skin that is characterised by repeated episodes of flushing, persistent reddened skin and spots. Some sufferers report sensations of burning and stinging in the skin, and it isn't uncommon to experience eye symptoms. Fair-skinned women aged between 30 and 50 years are the most commonly affected, and symptoms can be triggered by extremes of weather, stressful situations, strenuous exercise, spicy food, alcohol and hot drinks.
It is important to reassure Claudia that rosacea, while distressing, is not considered a serious condition. If the skin on her face is dry, she should use emollient creams and avoid topical corticosteroids and abrasive products such as facial scrubs. Claudia should try to avoid triggers as much as she can and be mindful to apply sunscreen if she is going to be exposed to sunlight, as this can also trigger symptoms.
As Claudia's rosacea appears to be relatively mild, a GP €“ once the diagnosis has been confirmed €“ is likely to prescribe topical metronidazole, which is thought to work as an anti-inflammatory and antioxidant rather than being used for its antibacterial properties. Oral antibiotics, most commonly tetracyclines, are used for more severe cases.
Top tips for healthy skin
Suggest customers follow these top tips for healthy skin throughout the winter months:
- Don't forget to protect hands in the winter, as they're often the first area of the body to dry out because they're constantly exposed to the elements. Use an SPF15 protective hand cream to prevent age spots as well as dryness. Wearing gloves in cold weather will also help
- Use a night cream to help prevent skin drying out
- Choose a creamier or more gentle cleanser during the winter months as harsh cleansers cause dryness
- Treat skin to a moisturising face mask every week during the winter months to leave it glowing and hydrated. Apply after exfoliating and leave on for 10-15 minutes before removing
- Choose a lip balm with SPF15 to help prevent cold sores and chapped lips
- Exfoliate skin once a week to remove the build-up of dead skin cells that can lead to flakiness and a dull complexion. Apply the product to damp skin and massage in gently, using circular motions, and rinse thoroughly
- Avoid harsh bubble bath and shower gel products and choose formulations that are creamy or oil-based, and always look for 'soap-free' products that don't dry the skin out.
Scenario 4: cold sores
William Bailey is picking up his prescription for his cholesterol-lowering medication. €Glad I managed to sort this out in time,€ he says. €I suddenly realised I was on my last few tablets and I'm flying to Austria tomorrow for a work conference.€ As he turns to leave, you notice he scratches the side of his mouth and he says: €I think I'm getting a cold sore. The sunshine out in Innsbruck will cure it, won't it?€
Solution
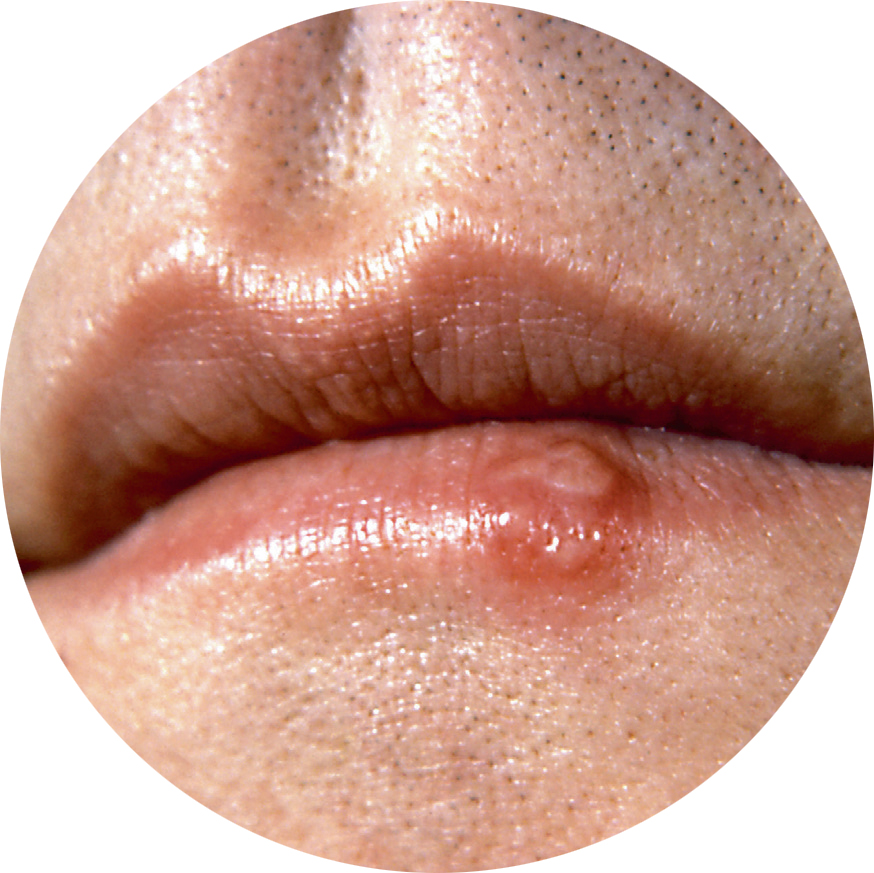 Cold sores are caused by the Herpes simplex virus, which usually lies dormant in the body but is occasionally reactivated by triggers such as having a fever or infection, tiredness, stress, hormonal changes and sunlight. So the sun may actually make William's symptoms worse rather than better.
Cold sores are caused by the Herpes simplex virus, which usually lies dormant in the body but is occasionally reactivated by triggers such as having a fever or infection, tiredness, stress, hormonal changes and sunlight. So the sun may actually make William's symptoms worse rather than better.
The first sign of a cold sore is usually a tingling or itching sensation around the mouth that can last between six and 48 hours, followed by the development of small, fluidfilled sores that are at their most painful for the first 24 hours but get better over five to seven days. Although the evidence base supporting the use of topical antivirals for the management of cold sores is small, such products are popular. Given that William is at the prodromal stage of infection €“ i.e. the lesions have yet to appear €“ he is at the right time to start using topical aciclovir or penciclovir, should he wish to, which may reduce the duration of his symptoms if he follows the application instructions carefully.
Given that William recognises the signs that he is getting a cold sore, it is safe to assume that he may suffer a recurrence in the future and could benefit from some advice on prevention. The most important thing he needs to do is to minimise the impact of trigger factors, including using sunblock lip balm to help reduce outbreaks caused by sun exposure. William may also want to keep a tube of antiviral cream at home so he is able to start treatment at the first sign of an attack.
Sun care in winter
Customers who are going on skiing trips need to take extra care of their skin, as higher altitudes mean that damaging UV rays can filter through the atmosphere so that more of them reach the skin. €These rays bounce back off snow, intensifying their effects,€ explains Dr Nick Lowe, consultant dermatologist at London's Cranley Clinic. €Ensure you use a broad spectrum sunscreen that contains proven levels of UVB and UVA protection and reapply regularly,€ he adds.
Dr Lowe also advises choosing a waterproof formulation and applying it before heading out to the slopes. Ensure customers don't forget sunscreen for lips too as they burn quickly. Recommend a stick formula that's easy to keep reapplying on the go. €Wear ski goggles or sunglasses to protect eyes from harsh sunlight on the ski slopes,€ says Candice Gardner, education curriculum manager at Dermalogica.
Even if a customer is not skiing, it's still important to protect skin from UV rays all year round. €Although the angle of the earth in relation to the sun means UVB, which causes burning, is not as concentrated, the UVA rays which penetrate deeper and cause damage to the dermis are consistent all year round. This means that it's vital to still protect skin from UV rays during the winter months,€ says Candice.
Scenario 5: psoriasis
Josie Bartlett is a student at the local sixth form college who works at the pharmacy on Saturdays. After she finishes her shift one weekend, she asks for a quiet word. Once in the consultation room, she says that her scalp has been bothering her, and lifts her hair from her neck to reveal several red patches of skin covered in thick, silvery-white scales.
She says that she has had similar patches in the past, but since the start of the cold weather a few weeks ago, it seems to have worsened. While it isn't particularly itchy or uncomfortable, she says she is starting to feel self-conscious about it.
Solution
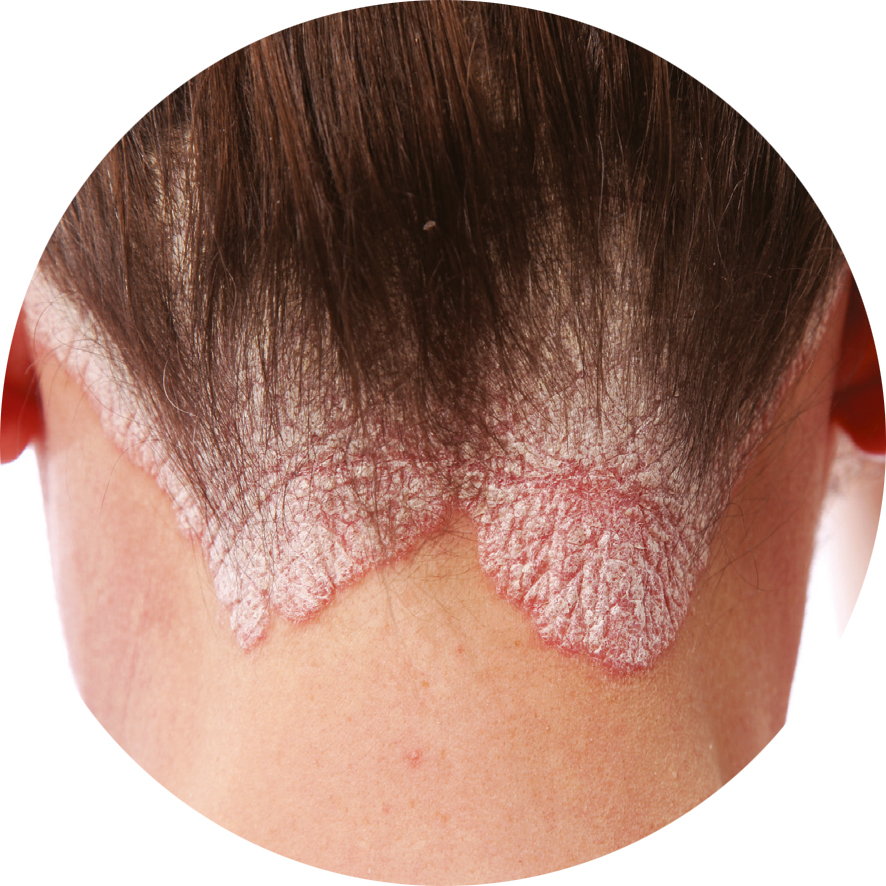 Josie appears to have psoriasis, a condition in which skin cell turnover is accelerated, causing immature cells to accumulate on the surface of the skin. In most cases, symptoms become worse as the result of a trigger, which may be a change in the weather €“ as seems to be the case for Josie €“ or hormone levels, stress, smoking, excessive alcohol consumption, trauma to the skin, certain medicines, and certain immune disorders.
Josie appears to have psoriasis, a condition in which skin cell turnover is accelerated, causing immature cells to accumulate on the surface of the skin. In most cases, symptoms become worse as the result of a trigger, which may be a change in the weather €“ as seems to be the case for Josie €“ or hormone levels, stress, smoking, excessive alcohol consumption, trauma to the skin, certain medicines, and certain immune disorders.
Psoriasis is a condition that needs to be diagnosed by a GP, and managed using prescription products. For mild to moderate cases, the application of a vitamin D product such as calcipotriol, calcitriol or tacalcitol once a day may be sufficient. Assuming Josie is prescribed such a treatment, she needs to give it around four weeks, and then, if her response is good, continue using the product until her skin is clear. Emollients should be regularly applied thereafter to protect the skin and reduce moisture loss, and can also be used to soften and loosen scales before applying vitamin D products.
Other drugs that may be used include topical corticosteroids, calcineurin inhibitors such as tacrolimus and pimecrolimus and coal tar products. Alternative options that may be used in severe cases include phototherapy or systemic medication, which may be oral (e.g. methotrexate, ciclosporin and acitretin) or injectable (e.g. etanercept or adalimumab). The effect that psoriasis can have on appearance means that people with the disease are more likely to suffer from emotional problems such as depression and anxiety.
As Josie will be under the care of her GP for her psoriasis, she will be undergoing regular reviews, but as her work colleague, it is worth bearing this in mind if her mood seems low in the future. She should also make sure she takes good care of herself by eating a healthy diet and taking regular exercise, as psoriasis sufferers are at increased risk of developing diabetes and cardiovascular disease in later life.
Signposting
- The College of Podiatry
- National Eczema Society
- The British Association of Dermatologists
- The National Rosacea Society
- Herpes Viruses Association
- The Psoriasis Association.
A generous quantity of the emollient of choice should be smoothed onto the skin in the direction of hair growth
