Save our soles
In Conditions
Follow this topic
Bookmark
Record learning outcomes
There’s a direct link between buying shoes without trying on first and the risk of developing issues with the feet, says research by the College of Podiatry. Find out how pharmacy can help with advice on preventing and treating common foot problems
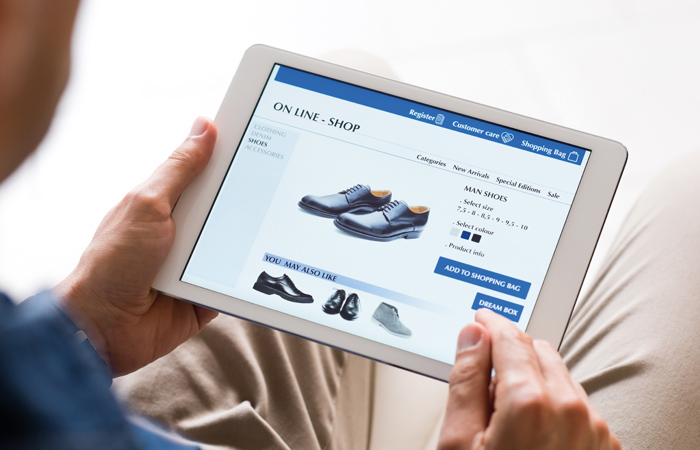
The growing trend for buying footwear online without trying on first is having an impact on the health of our feet, a survey by the College of Podiatry has revealed. Research found that 66 per cent of adults who don’t try on shoes before they buy experience foot problems, compared with 53 per cent of those who always do, and 56 per cent of respondents had bought shoes online in the past year. The research also found that 68 per cent of adults never get their feet measured, making them twice as likely to experience foot pain. In addition, those who skip trying on shoes are twice as likely to report ingrown toenails and corns.

“Ill-fitting footwear is responsible for a great many foot problems, including corns, calluses, blisters, bunions and hammer toes. By forcing your feet into tight shoes you can cause permanent changes to your foot structure,” explains Emma McConnachie, podiatrist and spokesperson for the College of Podiatry. “Our culture for fast fashion has changed our approach to shoes and expert fitting for adults is now not easily available. The rise in online shopping has also increased the number of people who are not trying shoes on before they buy them.”
Pharmacy staff can play a key role in advising customers about the potential problems caused by poorly fitting shoes, as well as recommending treatment for minor complaints. “Some people will need a simple OTC product as a first-line treatment, while others would be best directed to a podiatrist. This can greatly ease the strain being placed on GP practices by ensuring patients are directed to the most appropriately trained healthcare professional,” explains Emma.
Latest figures show that around half a million GP appointments a year are for foot health problems, many of which could be dealt with by pharmacy staff and podiatrists.
Familiar foot foes
While pharmacy teams can highlight the importance of buying properly-fitting shoes, getting the feet measured and helping to avoid related issues with the feet, they can also be on hand to offer information and advice on how to treat and prevent common foot problems, such as the following:
Plantar fasciitis
Meaning inflammation of the heel, plantar fasciitis affects around one in 10 people, most commonly those aged 40-60, and is more common in runners but can affect anyone. It’s caused by repeated small injuries to where the plantar fascia attaches to the heel bone. People are more likely to be affected if they spend a lot of time on their feet, have started exercising on a different type of surface, wear shoes with poor cushioning or are overweight.
Pain anywhere in the heel is the main symptom. It is usually worst first thing in the morning or after long periods of rest.
How is it treated?
Plantar fasciitis will normally improve over time. Resting the foot can help to ease the pain so avoiding running and excess walking and standing is a good idea. Gentle walking and stretching exercises can help. Well-cushioned shoes should be worn and walking barefoot avoided.
Heel pads and arch supports can help and work best if worn all the time. Anti-inflammatories can help ease the pain. If the pain is severe, steroid injections can be given to reduce inflammation.
“If heel pain has been present for more than three weeks it is best to have it assessed by a podiatrist to ensure it is plantar fasciitis as there are a variety of causes of heel pain,” says Emma.
Ingrown toenails
An ingrown toenail is where a piece of nail – usually on the big toe – pierces the skin and can be painful, inflamed and become infected. The shape of feet and toes can make people more prone to an ingrown toenail.
Excess sweating makes it more common in people who do regular sport or exercise. However, the most common cause is not cutting nails properly, including trimming too short or leaving a jagged edge of nail. Tight shoes can also push the nail into the surrounding skin.
Pain and inflammation of the surrounding skin are the main symptoms.
How is it treated?
To help prevent infection, customers can bathe the affected foot in a salty footbath and apply a sterile dressing. A podiatrist can remove the nail spike.
Prevention tips
- Use nail clippers to trim toenails
- Cut nails straight across, but not too short or down the sides
- Choose footwear and hosiery made of natural fibres to avoid sweaty feet.
Those who skip trying on shoes are twice as likely to report ingrown toenails and corns
Verrucas
These are warts on the soles of the feet, caused by the human papillomavirus (HPV). They are most common in those aged under 20. The virus thrives in moist, damp environments, such as communal changing room and around swimming pools. The small, rough lumps of skin often have a black dot in the centre. They can be painful and may develop in clusters.
How are they treated?
“Many verrucas will resolve themselves in six to 12 months, however if it is getting bigger, spreading to other areas or causing pain then treatment may be advised. However, as it is caused by a virus, there is no guaranteed treatment that will get rid of it,” says Emma.
Salicylic acid in the form of lotion, paint or plasters work by burning off the top layer of the verruca. It needs to be applied daily for up to three months. The surrounding skin can be protected by applying petroleum jelly before treating. Freeze treatments are also available which work by destroying the verruca tissue.
Prevention tips
- Wear a waterproof plaster when swimming to prevent spreading
- Wear flip-flops when using communal changing rooms and showers to prevent infection.
Corns and calluses
These are thickened, often painful, areas of skin caused by pressure or friction from shoes. Hard corns occur on the top of smaller toes or outer edge of the little toe. Soft corns form between the toes. Calluses form on the sole of the foot, usually just underneath the toes and are caused by repeated friction from walking and running.
How are they treated?
Salicylic acid treatment works by dissolving the keratin that makes up the dead layers of skin in corns and calluses. They come in the form of plasters, pads and drops. They should not be used by people with diabetes or poor circulation. A cushioning pad or shoe insole may help to protect the skin and allow the corn or callus to heal.
Prevention tips
- Gently rubbing hard areas of skin with a foot file and then applying a foot moisturising cream can help
- Make sure shoes fit properly and are not too tight.
Cracked heels

“Cracked heels are caused by a decrease in the moisture level in the skin around the heels. Wearing backless shoes increase the friction to the area which increases the risk of cracks,” says Emma.
How are they treated?
“If there is a thick yellowish layer of skin over the heels, see a podiatrist to have this removed, which will help improve
the condition of the skin.” A high level urea cream (25% plus) applied daily will help to repair the skin and heal cracks.
Prevention tips
- Keep the skin hydrated with a foot cream
- Avoid backless shoes.
Choose footwear and hosiery made of natural fibres to avoid sweaty feet
Athlete’s foot
This common skin infection is caused by a fungus and affects up to one in four people at one time. It is more common in people who sweat more, or wear shoes and socks that make their feet sweaty. It can be passed on in communal showers and around swimming pools. Signs are an itchy, scaly rash between the little toes. Skin may become cracked and sore with splits in the skin, which may be painful.
How is it treated?
Topical antifungal treatments will treat the infection. These include terbinafine, clotrimazole, econazole, ketoconazole and miconazole. These come as sprays, liquids or powders. They should normally be continued for one to two weeks after the infection has disappeared to clear the fungus completely.
Prevention tips
“Advise customers to wash feet regularly and dry between toes. Also avoid walking barefoot in communal areas and trying on shoes barefoot when shopping,” says Emma. In addition:
- Don’t share towels
- Use anti-fungal foot sprays to prevent recurrence
- Alternate shoes every two to three days
- Change socks or tights daily.
Blisters
Blisters can be caused by ill-fitting footwear, socks rubbing against skin or feet getting very wet or sweaty. In people with diabetes they can become more serious as they may not heal easily.
How should they be treated?
Blisters should not be burst as this can result in infection. Instead, place a circular piece of foam or felt over the blister with a hole through the middle and tape in place. This prevents further friction on the skin. Alternatively, apply a hydrocolloid blister plaster, which forms a second skin over the blister to protect it and allow it to heal.
Prevention tips
- Wear well-fitting footwear and ensure socks are the right thickness for the shoes
- Keep feet dry – for sweaty feet, use a spray to control moisture
- When exercising, choose socks that help to draw sweat away from the skin.
Footcare and diabetes

Diabetes leads to 169 amputations every week, according to Diabetes UK, and the number of lower limb amputations is increasing. “Having diabetes increases people’s risk of developing serious problems with their feet. It can damage the sensation in the feet, and this loss of feeling can mean people with diabetes do not notice injuries,” says Dan Howarth, head of care at Diabetes UK. “Not noticing wounds – and not getting them treated – can lead to foot ulcers, infections, and at worst, amputations. Unhealed ulcers and foot infections are the leading cause of diabetes-related amputations, with diabetic foot ulcers preceding more than 80 per cent of amputations.”
Diabetes can cause reduced sensation in the feet as the nerves don’t work as well due to nerve damage from raised glucose levels (diabetic neuropathy). People with diabetes also have increased risk of peripheral arterial disease, with the legs and feet commonly affected. Skin with poor blood supply won’t heal as well as normal.
Poorly-fitting footwear can put pressure on feet, resulting in blisters, corns and calluses, which increase risk of foot ulcers.
“We recommend that diabetics check their feet every day to ensure there are no breaks in the skin or emerging problems. Any open wound, especially with neuropathy, should be professionally assessed and treated as soon as possible,” says Emma McConnachie, podiatrist and spokesperson for the College of Podiatry.
Everyone with diabetes is entitled to a free annual foot health check, usually as part of their annual diabetes check at the patient’s GP practice. However, there are signs that customers should watch out for and consult their GP if they notice any, says Dan, such as:
- Tingling feeling in the feet
- Pain
- Dull ache
- Shiny, smooth skin on legs and/or feet
- Loss of sensation
- Swollen feet
- Feet not sweating
- Wounds or sores not healing
- Cramp in legs when resting or walking.
“If any of the above are noticed, it’s really important that customers take the weight off their foot, contact their GP or foot protection team immediately, or go to their nearest out-of-hours healthcare service if these aren’t available,” says Dan.
Diabetes UK has produced a video you can pass on to customers on how to check their feet daily.
Red flags which warrant immediate medical attention include:
- Change in colour or shape of feet
- Cold or hot feet
- Blisters or cuts that can be seen but not felt
- Foul smell from an open wound.
Customers with diabetes can do a sensitivity test at home to check for loss of sensation in their feet using this video and instructions.
Top tips
Diabetes UK has the following advice for pharmacy teams to pass on to customers with diabetes to help prevent foot problems:
- Get help to quit smoking, as this increases risk of narrowed blood vessels
- Control blood sugars, cholesterol and blood pressure
- Check feet daily for any changes
- Eat a balanced diet and stay active
- Take care when cutting toenails, file off sharp edges and avoid piercing the skin
- Make sure footwear fits comfortably and that socks and tights don’t rub
- Use a moisturising cream every day to stop skin drying out, but pick one that’s fragrance-free to avoid irritating skin
- Don’t use blades or corn removal plasters as these can damage skin.
