Scratching the surface
In Conditions
Follow this topic
Bookmark
Record learning outcomes
With the majority of people self-treating skin conditions, pharmacy teams are well placed to offer advice and recommendations to help customers manage them and keep their skin clear and hydrated
Around 60 per cent of the population have experienced a skin condition at some point, according to the British Skin Foundation. Of these, around three-quarters will self treat, representing a huge opportunity for pharmacy staff to get more involved in offering advice on condition management and how customers can get the best from their treatments. So what are the most common conditions and what should be advised?

Psoriasis
Around 1.8 million people in the UK are affected by psoriasis, according to the Psoriasis Association. It can affect people at any age, but most commonly first appears from the late teens to thirties, or between the ages of 50 and 60. It is an immune condition that causes the skin renewal system to speed up, leading to an accumulation of skin cells.
- Causes
“A combination of genetic and environmental factors play a role in the development of psoriasis,” says Dr Anton Alexandroff, spokesperson for the British Association of Dermatologists (BAD). “There are several potential triggers [that] can cause flares, including infection, stress, damage to skin, intense sunlight and certain medications. Smoking, alcohol and obesity may result in poor response to treatment.” Psoriasis-causing changes in skin begin when T-cells are triggered and become overactive. The T-cells produce inflammatory chemicals, which then cause rapid growth of skin cells.
- Spot the signs
Psoriasis is characterised by raised red patches of skin – or plaques – often covered with silvery scales. They are most common on the scalp, trunk and limbs, but can appear anywhere on the body. The plaques can range in size from a few millimetres to several centimetres in diameter.
- Treatments
Regular use of emollients is essential to make skin more comfortable. Customers will need to see a GP or dermatologist for specialist treatments. These commonly include:
- Vitamin D derivatives
- Coal tar preparations
- Topical steroids
- Dithranol
- Vitamin A derivatives
- Calcineurin inhibitors
- Dermatologists can prescribe UV light therapy for resistant or severe cases.
There are several new prescription-only treatments that Dr Alexandroff says pharmacy staff should be aware of, including Enstilar foam, which contains the active ingredients calcipotriol and betathemasone and additional penetration components. It works twice as fast and is twice as effective as Dovobet gel, he says.
- Self care tips
Dr Alexandroff advises the following tips to pass on to customers:
- Adopting a healthy lifestyle which includes a balanced diet and exercising regularly
- Stopping smoking and reducing intake of alcohol
- Where possible, reduce stress
- Use emollients regularly.
Acne
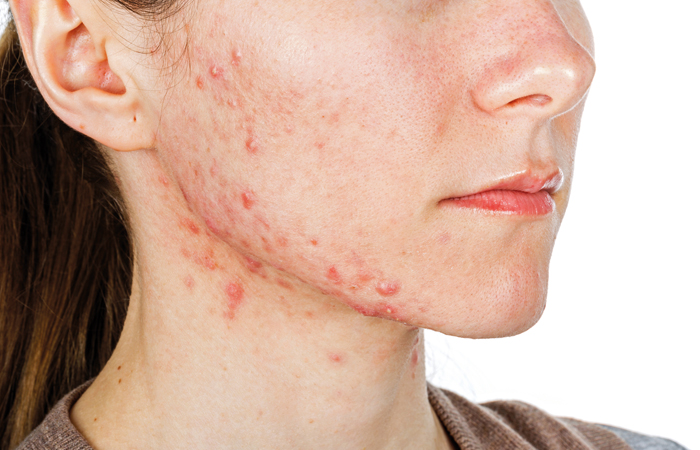
Acne is most common in young people, with 80 per cent of 11- to 30-year-olds affected to some degree. In addition, 19 per cent of adults over the age of 25 have reported acne, according to Acne Support – a new resource from the British Association of Dermatologists (BAD).
Acne is a poorly understood condition and can have a significant psychological effect on sufferers. Some 54 per cent of those who’ve experienced it said it affected their self-confidence and 22 per cent felt it affected their social lives, according to a recent survey by Acne Support.
The survey also found that when prompted with a list of treatments and remedies, 34 per cent of people didn’t know which were safe or effective acne treatments.
- Causes
Acne is linked with changes in hormone levels. For boys during puberty, production of the male hormone testosterone increases and triggers a boost in sebum production, leading to oily skin. This also causes the lining of hair follicles to thicken, leading to blockages. The increased oiliness also triggers a reaction in the skin bacteria P. acnes, which causes inflamed skin.
In women – 80 per cent of adult acne is in women – hormone changes are also to blame, with pregnancy and menopause common acne triggers. Other factors include stress and diet.
- Spot the signs
Oily skin is a common sign of acne, especially on the face, neck, chest and back. There are several different types of acne spots pharmacy teams might see in customers: blackheads, whiteheads, papules (small red bumps), pustules (red bumps with white tip), nodules (hard lumps beneath skin) and cysts. In severe cases, large spots can leave scars, which occurs in a fifth of sufferers.
- Treatments
For mild acne, pharmacy teams can recommend an over-the-counter (OTC) cream or gel containing benzoyl peroxide, salicylic acid or nicotinamide. Benzoyl peroxide comes in 2.5% to 10% strengths. Dr Thivi Maruthappu, consultant dermatologist and British Skin Foundation spokesperson says: “Always recommend patients use the lowest strength possible to avoid irritation and redness.”
He advises against using too many potentially irritating products – such as exfoliating scrub, benzoyl peroxide and salicylic acid – at once, as it can worsen inflammation. The use of antibiotic monotherapy is discouraged due to the risk of antibiotic resistance, Dr Maruthappu adds.
- Self care tips
“Advise customers to cleanse [the skin] carefully – morning and evening – with a gentle cleanser and then apply topical acne products. Use non-comedogenic products and be cautious with use of oil-based hair products [that] can aggravate acne,” recommends Dr Maruthappu. “Advise customers against wearing make-up when exercising and to consider sweat-wicking gym wear.”
- Sensitive topic
Some customers may be embarrassed by their acne and reluctant to seek advice. “It is important to be empathic and non-judgmental as patients can feel that others believe them to be ‘unclean’ or eating a poor diet. Sharing with patients that acne can be a result of hormones, genetics or stress can be helpful,” says Dr Maruthappu. “Nodulcystic acne can lead to considerable scarring and should therefore be referred to the GP promptly. Some female patients may have underlying polycystic ovary syndrome (PCOS), which should also be referred.”
Eczema
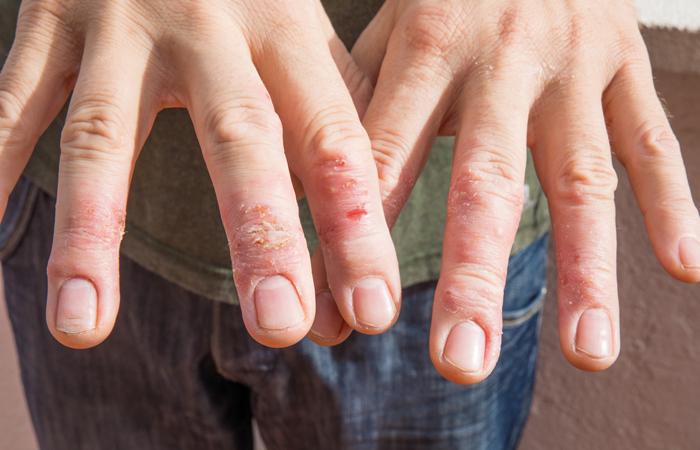
Eczema is the most common skin condition, with one in five children and one in 12 adults affected, according to the National Eczema Society.
- Causes
Genetics have a strong influence on the development of atopic eczema, present in 80 per cent of children where both parents are affected, and 60 per cent if one parent is affected. Environmental factors also play a role, with air pollution a key contributor, alongside food allergens and exposure to pollen, dust mites and pets. In addition, Dr Maruthappu says: “We now know that an impaired skin barrier is an important contributor to the development of atopic eczema.”
- Spot the signs
Atopic eczema is characterised by patches of red, dry, itchy and cracked skin. It most often affects the hands, insides of elbows, backs of knees and, in children, the face and scalp. Most sufferers have periods when eczema ‘flares up’ and times when it is less active. Itching is the trademark symptom of eczema.
- Treatments
Emollients are the mainstay of eczema treatment. “Patients should apply emollients liberally at least once a day, twice if possible. They should be applied plentifully – for adults with dry skin all over their body, we recommend 500-1000g per week. If using emollient from a tub, advise customers to use a clean spoon or spatula to apply the product to avoid contamination,” says Dr Maruthappu. Customers should be encouraged to try different emollients until they find one that suits their skin.
For additional treatment, Dr Maruthappu advises that OTC antihistamines can help with itching and topical steroids can be applied to affected areas. “Used carefully, topical corticosteroids are valuable in the management of atopic eczema. One fingertip unit is enough to treat an area the size of the front and back of a patient’s hand,” he says. It should normally be used just once daily and continued until 48 hours after a flare up has cleared. Customers should leave 30 to 60 minutes between emollients and corticosteroids. If there is any sign of infection, see the GP, Dr Maruthappu adds.
The National Institute for Health and Care Excellence (NICE) has recently approved use of a new injectable biological therapy for moderate-severe eczema. Dupilumab is available to patients who have not responded to or can’t use Ciclosporin.
- Self care tips
Customers can be advised to:
- Use a soap substitute
- Apply emollients regularly and liberally
- Treat flare ups promptly
- Wash clothes with non-biological powder
- Seek a dermatological referral if they are not responding to treatment.
Rosacea
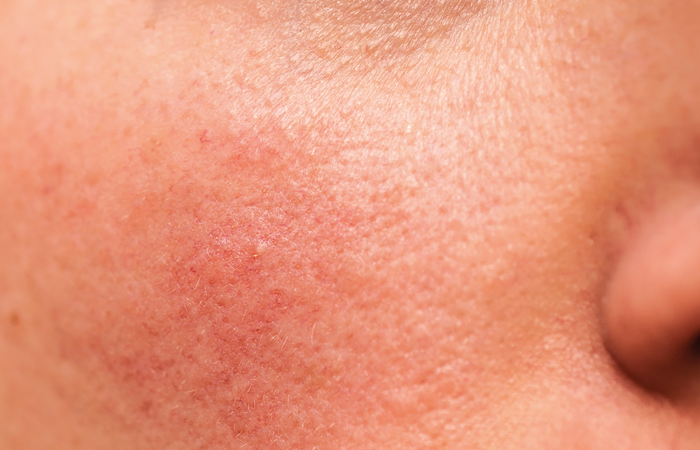
This affects one in 10 people in the UK, mainly fair skinned people aged 40-60 years. It’s often confused with acne but responds to different treatment so it’s important that customers see their GP for a diagnosis.
- Causes
“The exact cause of rosacea is unknown, but underlying trigger factors cause both inflammation and an undue readiness of the blood vessels of the face to dilate.” says Dr Alexandroff.
Common triggers include alcohol, exercise, high and low temperatures, hot drinks, spicy foods, sunlight and stress.
- Spot the signs
Signs to watch for include frequent flushing, thickening of affected skin, redness on parts of the face – similar to the appearance of sunburn – small lumpy red spots, small cysts and tiny blood vessels visible on the face.
The eyes can be affected too, causing dryness, itching and sensitivity to light. Inflammation and infection of the cornea is a serious complication, which can affect vision. Patients should be advised to seek medical help for eye pain or visual symptoms associated with rosacea.
- Self care tips
“It’s important for customers to not rub or scrub their face. Clean the skin using a gentle, non-abrasive cleanser. Advise use of a soap substitute and a perfume-free moisturiser. The use of steroid creams should only be adopted if instructed by a GP or dermatologist as they can worsen symptoms,” says Dr Alexandroff.
- Treating rosacea
Antibiotics are the usual treatment. For mild-to-moderate rosacea, topical antibiotics include metronidazole and ivermectin. For more severe cases, oral antibiotics are recommended, such as tetracycline or erythromycin.
Topical azelaic acid is an alternative to antibiotics to treat mild-to-moderate rosacea.
To reduce redness, brimonidine is helpful. Laser and light therapy may be used for extreme redness and dilated blood vessels.
