Back to basics
In In-depth
Follow this topic
Bookmark
Record learning outcomes
Deaths related to asthma attacks have increased in recent years, raising the question of whether enough is being done for the basic care of this common lung condition. But pharmacy teams can help
For a health condition with no cure, the treatment options available for people with asthma make this common lung condition manageable. But recently questions have been raised about whether enough people have access to basic asthma care and Asthma UK says more needs to be done.
The charity highlights that deaths from asthma attacks are currently the highest they have been in the last decade, increasing by over 33 per cent during that period. In 2018, over 1,400 people died from an asthma attack, which is an eight per cent increase from 2017. The data also reveals that there has been an increase in men dying from asthma attacks, as well as a 42 per cent increase in deaths in people aged between 33 and 44 years over the same period.
The National Review of Asthma Deaths (NRAD), commissioned by the NHS and Department of Health five years ago, also found that two-thirds of asthma deaths could have been prevented by better basic care.
Asthma UK also estimates that 60 per cent of people with asthma in England and Wales – 2.9 million people – are not receiving basic care as recommended by national guidelines. Of the 19 recommendations to improve care made by NRAD, only one has been partially implemented, according to Asthma UK.
“It is completely unacceptable that thousands of people with asthma in England and Wales have died needlessly from asthma attacks,” says Kay Boycott, chief executive of Asthma UK. “It’s been five years since the National Review of Asthma Deaths found that two-thirds of deaths from asthma attacks could have been prevented with basic care, yet we are still seeing tragic cases of lives being cut short”.
She adds: “The same mistakes are being made again and again because essential recommendations have not been implemented. This lack of action is costing lives and devastating families and communities.”
In 2018, over 1,400 people died from an asthma attack, which is an eight per cent increase from 2017

Call for change
Asthma UK has urged the NHS to take action to enable more people to have access to basic asthma care. Asthma currently costs the NHS an estimated £3 billion annually, according to the NHS.
“The NHS must act now to ensure that everyone with asthma in England and Wales gets basic asthma care which includes a yearly review with their GP or asthma nurse, a check to ensure they are using their inhaler properly and a written asthma action plan,” says Kay. “The NHS needs to ensure that all healthcare professionals are providing this care to patients.”
As part of the NHS Long Term Plan, more than three million people are expected to benefit from improved respiratory, stroke and cardiac services over the next decade. NHS England says it will be working alongside a range of clinicians, commissioners and voluntary sector organisations including the British Lung Foundation and Asthma UK to deliver the new programme.
NHS England has also developed an asthma toolkit and national standards, as well as creating a set of ambitions for healthcare professionals, commissioners, schools, parents, carers and young people that outline effective asthma care plans, standards and improved asthma care delivery.
Commenting on the way forward for asthma care, Mike Morgan, national clinical director for respiratory at NHS England, says: “Asthma UK worked closely with the NHS to develop proposals in our Long Term Plan, which sets out measures including better diagnosis of the condition, improved medicine reviews and stronger guidance for local health services to better support families living with asthma, all of which will contribute to more than three million people benefitting from improved respiratory, stroke and cardiac services over the next decade, but as we’ve seen this week, with confirmation that one third of childhood asthma cases are linked to air pollution, it’s clear that a big part of this challenge cannot be met by the NHS alone.”
If what has been promised in the proposed programme is delivered then there is hope that the number of deaths due to asthma attacks will stop increasing. Pharmacy teams can help, not only in delivering the aims of the new programme, but also make a significant contribution to people having better access to basic asthma care and information.
Asthma triggers
Asthma is caused by the swelling of the breathing tubes that carry air in and out of the lungs, making the tubes highly sensitive and temporarily narrow. This can occur randomly or after exposure to a trigger.
Common asthma triggers include:
- Allergies, including pollen, animal fur and dust
- Cold air, smoke and pollution
- Exercise
- Infections including colds or flu.
Pharmacy teams can help customers identify triggers and try to avoid them, or have their personalised action plan ready, just in case.
What is basic care?
Approximately 5.4 million people are being treated for asthma in the UK including 1.1 million children and 4.3 million adults – that’s one in 11 and one in 12 people respectively. Pharmacy teams can hep customers be aware of the basic care they can do to manage their asthma effectively themselves.
Asthma UK says that just three elements of basic asthma care can prevent risk of emergency treatment:
1. Using a written asthma plan
According to Asthma UK, using a written asthma plan makes people up to four times less likely to end up in hospital due to asthma. Actions plans are available to download from the Asthma UK website.
2. Checking inhaler technique
A small change to technique can ensure enough medicine is reaching the lungs and make a big difference. Asthma UK and the NHS have videos on inhaler technique to help healthcare professionals and patients.
3. Booking an annual asthma review
An annual check up means asthma stays monitored. At a check up, customers can check their peak flow, review their medicines and even review their inhaler technique.
Lucy Bramwell, senior policy and project manager for the Taskforce for Lung Health, says: “Teams can discuss inhaler technique when people collect their medicines. They can ask ‘do you know how to use this properly?’, even if it’s a repeat prescription”.
A written asthma plan makes people four times less likely to end up in hospital due to asthma
Providing relief
Pharmacy teams have an opportunity to help people with asthma, and with deaths from the condition at their highest in a decade, it’s more important than ever for teams to get involved. Lucy says that pharmacy teams have a two-fold role in helping people with asthma. Firstly, teams can spot signs of asthma and flag it as a concern to people who don’t have a diagnosis. Then, be there to support people who do have a diagnosis.
World Asthma Day usually takes place in May each year, but this doesn’t have to be the only time teams can raise awareness. There are also plenty of resources available online that pharmacy teams can signpost customers to and use in the pharmacy. Lucy also recommends that pharmacy teams link asthma care to other events too such as Stoptober. “It’s good to talk to people about wider lung health, teams can signpost people to stop smoking services and give advice on that and the flu jab can really help as well”, she says.
Asthma attacks
Pharmacies can often be an important hub of health information, especially in deprived areas. “We know how important access to a pharmacy can be in reducing health inequalities,” says Lucy. “A lot of people can access them in a more flexible way than other health services. We estimate that 70 per cent of homes are within one kilometre, which is a short walk, of a community pharmacy.”
Pharmacy teams can put up recommended advice in the pharmacy so customers can easily have access to information about basic asthma care. For example, Asthma UK recommends that people who think they are having an asthma attack should:
- Sit up straight, not lie down and try to keep calm
- Take one puff of the reliever inhaler every 30-60 seconds, up to a maximum of 10 puffs
- Call 999 if they feel worse at any point, or if they don’t feel better after using 10 puffs of the reliever inhaler
- Take the reliever inhaler again after 15 minutes. If they’re waiting for the ambulance for longer than 15 minutes, they should take one puff every 30-60 seconds, up to a maximum of 10 puffs.
N.B. This asthma attack information is NOT for people on a SMART or MART regime.
Other good advice to give to customers is when to recognise that they are having an asthma attack. Customers should book and appointment with their GP if their symptoms are returning often, if they’re waking up at night due to asthma, if symptoms are getting in the way of their daily routine or if they are using their reliever inhaler (usually blue) three times a week or more.
Spacer usage for asthma attacks
Within all British Thoracic Society (BTS) and international guidelines a spacer (VHC) should be used for both mild and moderate attacks, more information can be found here: BTS 2019 Guidelines support for MDI and spacer.
- Children and adults with mild and moderate asthma should be treated by pMDI + spacer with doses titrated according to clinical response
- In children aged five to 12, a pMDI + spacer is as effective as any other hand-held inhalers
- In adults, a pMDI ± spacer is as effective as any other hand-held inhaler, but patients may prefer some types of DPI.
In children, a pMDI and spacer is the preferred method of delivery of β‚‚ agonists and inhaled corticosteroids. A face mask is required until the child can breathe reproducibly using the spacer mouthpiece. Where this is ineffective a nebuliser may be required. A pMDI + spacer is the preferred option in children with mild to moderate asthma.
If a child is having an asthma attack which has not been controlled by up to 10 puffs of salbutamol via a pMDI and spacer, parents or carers should seek urgent medical attention.
Improving inhaler technique
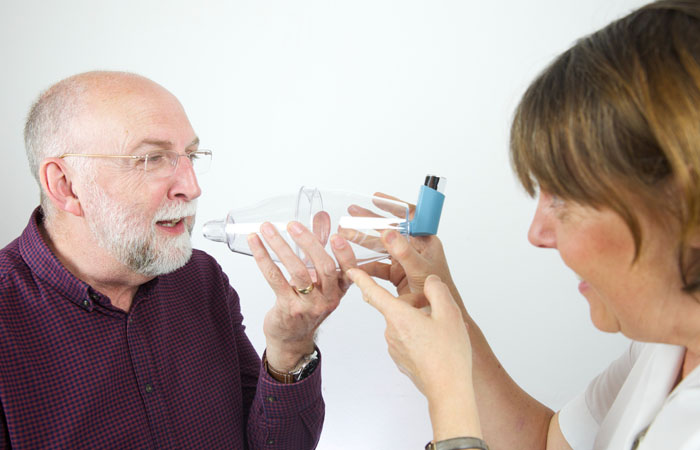
Asthma patients should have their technique checked at their annual inhaler review. Teams should also make customers aware of the common technique errors made when using an inhaler.
These may include:
- Not shaking or priming the inhaler before using
- Continuing to use an empty inhaler
- Not breathing out fully before inhaling
- Breathing in too fast or too slow
- Not holding their breath for long enough.
